Current Concept Review
Diagnosis and Management of Nerve Injuries Caused by Pediatric Upper Extremity Fractures
1Texas Scottish Rite Hospital, Department of Orthopaedics, University of Texas Southwestern Medical Center, Dallas, TX; 2Department of Surgery and Perioperative Care, Dell Medical School, University of Texas at Austin, Austin, TX; 3Nationwide Children’s Hospital, Columbus, OH; 4Shriners Hospital for Children-Portland, Portland, OR; 5Department of Orthopaedics, University of Connecticut School of Medicine, Farmington, CT
Correspondence: Christine A. Ho, MD, University of Texas Southwestern Medical Center, Dept. of Pediatric Orthopaedics, E2300-E2.01, 1935 Medical District Drive, Dallas, TX 75235. E-mail: [email protected]
Received: April 14, 2023; Accepted: April 17, 2023; Published: May 1, 2023
Volume 5, Number 2, May 2023
Abstract
Although nerve injuries occur commonly with pediatric upper extremity fractures, there is very little existing literature to guide the management of those nerve injuries that do not recover during routine fracture healing and follow-up, and even less guidance is available regarding the choice of diagnostic tests such as magnetic resonance imaging (MRI) with nerve sequences, electromyography (EMG), nerve conduction velocities, (NCV), ultrasound (US), or other modalities. In addition, patterns of nerve injury and timing of nerve recovery differ amongst different fractures. This review article describes the nerve injuries and specific details of humeral shaft, supracondylar, Monteggia fracture-dislocations, and forearm fractures as well as the various available diagnostic tests. We synthesize the available literature, of which most is in the adult population, as well as the extensive clinical experience of the authors, all of whom specialize in pediatric hand and upper extremity.
Key Concepts
- The vast majority of nerve injuries associated with pediatric upper extremity fractures are neuropraxias.
- The most common nerve injured in humeral shaft fractures is the radial nerve; in supracondylar humerus fractures, it is the median nerve/anterior interosseous nerve; in elbow dislocations, it is the ulnar nerve in conjunction with a medial epicondyle fracture, although the median nerve can become incarcerated during reduction of the dislocation; and in Monteggia fracture-dislocations, it is the posterior interosseous nerve. All nerves are at risk, depending on the apex of the deformity, in forearm fractures.
- Observation is the mainstay of early management; progressive documented nerve recovery does not require further diagnostic studies.
- Referral to a pediatric upper extremity surgeon or hand surgeon should be strongly considered when there is no documented nerve recovery after 3-4 months post-injury.
Introduction
Thankfully, most pediatric upper extremity injuries are not associated with nerve dysfunction, and fractures tend to heal well with appropriate nonsurgical and surgical treatment. When a child is seen with an associated nerve, both the complexity of treatment and the anxiety of the provider/parents increase. Providers are faced with making sure they make an accurate diagnosis and consider methods (immediacy of reduction, exploration) to mitigate long-term dysfunction. In the few nerve injuries that fail to improve with time, the provider has to consider the appropriate time to leverage expensive (MRI under anesthesia) and painful (EMG/NCV) studies in order to plan the next steps. A comprehensive understanding of the benefits of nerve exploration, neurolysis, nerve repair, grafting, or transfers is required as well as an understanding of when these methods are not appropriate and when it’s best to recommend later reconstruction. The purpose of this current paper is to provide a guide for the decisions required to manage our patients with concomitant nerve injury. Late reconstruction will be the topic of a subsequent paper and will include the release of contracted muscles, tendon transfer, innervated free muscle transfer, or skeletal stabilization.
Upper Extremity Injuries
Humerus Shaft Fractures
While the majority of humeral shaft fractures are treated nonoperatively with minimal complications, 4-5% have an associated radial nerve palsy.1 This is much lower than the 12% rate of radial nerve injury with adult diaphyseal humeral fractures.2 In fact, radial nerve palsies accounted for only 9% of pediatric peripheral nerve injuries in a level 1 trauma center.3
The radial nerve is at risk for tethering, as it pierces the lateral intermuscular septum at a distance of 35% of the arm length proximal to the lateral epicondyle in children.4 This is thought to make the nerve particularly prone to injury with distal 1/3 humerus fractures. In one paper, 38 children with this Holstein-Lewis fracture pattern demonstrated no cases of nerve palsies in one study, with the authors reasoning that thicker pediatric periosteum may be protective.5 When radial nerve palsy does occur, it is most often at the level of the distal main trunk in traumatic pediatric cases.
It is important to perform and document a relevant sensorimotor exam at the time of injury, yet this can prove surprisingly difficult in children. When checking wrist, thumb, and digital extension, one must differentiate the rebound extension that occurs from relaxing the flexors from true active extension. Furthermore, a cursory examiner can be fooled into thinking there is digital extension when it occurs only at the interphalangeal joints from intrinsic function (lumbricals) rather than true extension at the metacarpophalangeal joints (MCPJs), as only the latter confirms radial innervated extrinsic extensor function. Sensation testing can be limited by age, ability to communicate, and patient apprehension. It is important to recognize that a nerve injury can occur secondarily even during noninvasive treatment and does not necessarily represent a missed initial injury. This has been recorded in both adults during bracing,6 and in children, where in one case the palsy occurred 4 days after closed reduction and casting despite intact nerve function at the time of injury and immediately post reduction.7 As with most cases of secondary palsy, the palsy was due to traction and did resolve.
Minimal additional workup beyond serial clinical exams is warranted for pediatric radial nerve injuries, given that most fracture-associated injuries are neuropraxic. A report of three pediatric radial nerve palsies in a series of 80 humeral shaft fractures demonstrated all patients to have full spontaneous recovery by 154 days, with onset of recovery occurring at 41 days.8 While awaiting recovery, the wrist and MCP joints can be supported by extension bracing, and patients can be encouraged to perform motion exercises to limit contractures.
EMG for radial nerve injury in this clinical setting is not recommended by experts such as Bertelli until at least 6 months,9 which is still within the window of potential successful repair. Early surgical exploration is indicated in cases of suspected nerve discontinuity or entrapment based on injury mechanism, especially in open humeral shaft fractures. Previous indications, such as secondary palsy after closed reduction and distal 1/3 fractures, should no longer be utilized.10 Even iatrogenic cases are not definitively an indication as one study that involved a 40% rate of nerve palsy after intramedullary nailing reported 93% of cases to improve with time.11 One study of four closed and two open humerus fractures with associated palsy in children demonstrated all nerves to be in continuity, though surgical treatment was undertaken.1
Referral to an upper extremity specialist should occur if there are no clear clinical signs of recovery, such as an improving motor exam or migrating Tinel’s sign, after 6 weeks. Late exploration is acceptable as direct radial nerve repair can be successful even 6 months out given the shorter reinnervation distance to the extrinsic extensors compared to the median and ulnar innervation to the hand intrinsic musculature (Figure 1).
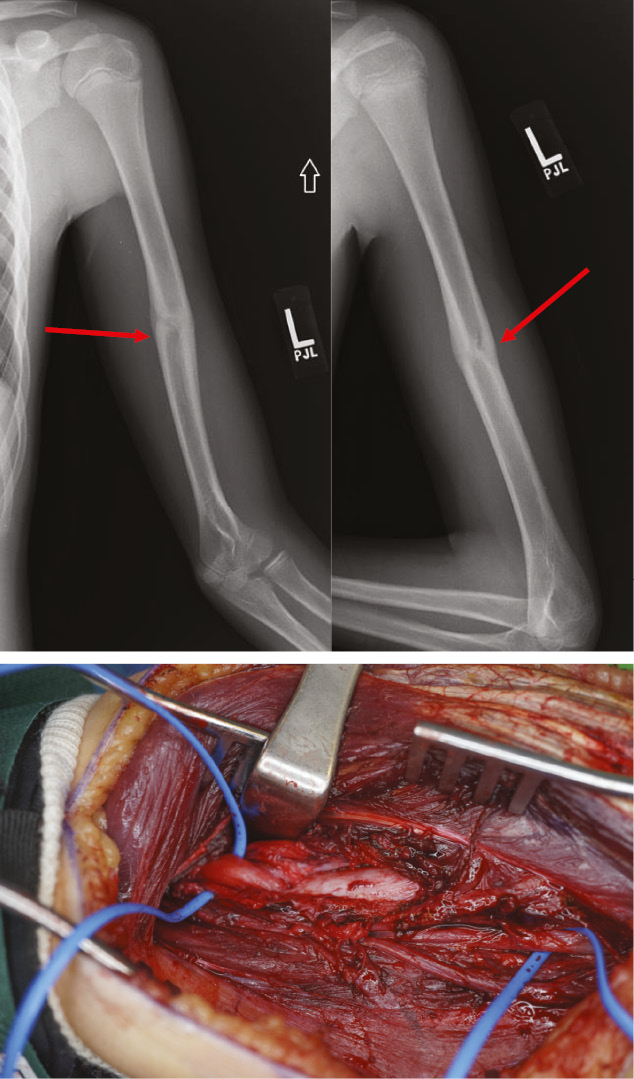
Figure 1. A 12-year-old male treated nonoperatively in a Sarmiento brace for a closed humeral shaft fracture with a concomitant radial nerve palsy. Patient was referred to a pediatric hand specialist after 3-4 months post injury with no clinical signs of radial nerve recovery as well as a radiographic suggestion of an entrapped nerve (red arrows pointing to lucency indicating probable entrapment of nerve in the fracture site). EMG/ NCV were obtained and showed no signs of nerve recovery or innervation. Surgical exploration revealed the radial nerve (blue loops) entrapped in the healed fracture site. (Figures courtesy of Krister Freese, MD)
Supracondylar Humerus Fractures
Nearly 10% of pediatric SCH fractures have associated neurovascular injuries, with severe SCH fractures yielding 20.6% concomitant neurovascular injury.12 The median nerve or its branch the anterior interosseous nerve (AIN) is the most at risk with extension-type fractures, while the ulnar nerve is most at risk with flexion-type fractures.13–15 In flexion-type fractures, rates of ulnar neuropraxia have been reported as high as 26%.16 Schultz and colleagues12 recently found that fractures with anteromedial bruising correlated with median nerve injury, and those with anterolateral bruising correlated with radial nerve injuries.
Although associated nerve injuries are common, over 90% of nerve injuries in extension-type SCH fractures recover within 6 months.17,18 Harris et al.19 found that 97% of patients with at least a 3-month follow-up had complete resolution of a preoperative AIN or median nerve palsy. Shore et al. reported the median time to nerve recovery is 2.3 months, with 60% of injuries having nerve recovery by 3 months and 92% recovering by 6 months.17 In their cohort of 218 children with isolated nerve injuries, the median nerve recovered the fastest, at a median of 2.1 months with 93% recovery at 6 months, followed by the radial nerve at a median of 3.2 months with 94% recovery by 6 months, and lastly the ulnar nerve at a median of 3.6 months with only 75% recovery by 6 months. This is not surprising given the longer distance that the ulnar nerve has to travel to innervate the intrinsic muscles of the hand versus the extrinsic flexor and extensor musculature of the proximal forearm for the median and radial nerves. It is the authors’ opinion that a nerve injury occurring at the time of the SCH Fx should be observed for 4 months prior to any further diagnostic testing (Figure 2).
Figure 2. A 7-year-old female with lack of recovery of concomitant median nerve injury with a posterolateral SCH Fx. Radial pulse was present throughout. Patient was lost to follow-up after 2 months and returned to clinic with incomplete return of median nerve function at 8 months post injury. Ultrasound revealed the median nerve to be incarcerated in the fracture site (median nerve isolated proximal and distal to the fracture site with blue vesi-loops, (yellow arrows show area of median nerve entrapment), with a freer elevator placed on fracture site, in left figure). A sural nerve cable graft (blue arrows) was used to graft between the proximal and distal segments (right figure). Return of 2-point discrimination at 8 mm was noted at 6 months postoperatively. (Figures courtesy of Christine A. Ho, MD)

Iatrogenic Injuries in Supracondylar Humerus (SCH) Fractures
There has been variable reporting of iatrogenic nerve injuries when treating SCH fractures, with reports ranging from as low as 0% to as high as 15%.15,20–23 In a meta-analysis by Babal and colleagues,15 ulnar nerve injuries occurred 3.2% of the time, followed by median nerve injuries (1.8%) and radial nerve injuries (1.6%).
In a systematic review by Brauer et al.23, the probability of ulnar nerve injury is 5 times higher with medial entry pins compared to lateral entry pins. Slobogean et al.24 found that there is an iatrogenic ulnar nerve injury for every 28 patients treated with cross pinning compared with lateral pinning. Ozçelik and colleagues25 found a significant increase in ulnar nerve injury with anteroposterior insertion of the medial pin in the sagittal plane while the elbow is flexed. In contrast, others have demonstrated that the use of a mini-open approach can significantly decrease risk to the ulnar nerve.26,27
There is a lack of consensus on how to manage iatrogenic ulnar nerve injuries, with some authors advocating for early observation,28,29 others advocating for early K-wire removal or repositioning,30 and still others advocating for early exploration of the ulnar nerve.31 Approximately 90% of iatrogenic ulnar nerve palsies managed expectantly will return to full function.29
Elbow Dislocations/Medial Epicondyle Fractures
Elbow dislocations in the pediatric population generally occur with other elbow fractures, most commonly the medial epicondyle, although proximal radius, olecranon, and coronoid fractures may also be present. As spontaneous reduction of a pediatric elbow dislocation is common, often times only a careful physical exam of a grossly swollen, painful elbow and identification of associated elbow fractures and/or nerve injury may be the only signs of an elbow dislocation. The vast majority of simple elbow dislocations may be treated with closed reduction and limited (10-14 days) cast/splint immobilization, but those associated with bone or nerve injuries may require surgical intervention.
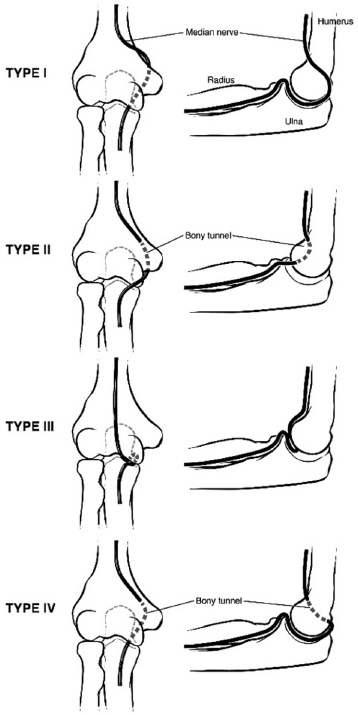
The ulnar nerve is the most commonly injured nerve, typically seen in conjunction with a displaced medial epicondyle fracture. The ulnar nerve may be compressed by the fibrous band that constrains the nerve to the posterior aspect of the displaced medial epicondyle or may become trapped in the joint with the medial epicondyle post-reduction. The median nerve can also become incarcerated in the elbow joint after reduction; three patterns were described by Fourrier: Type 1: dislocation between the trochlea and olecranon posteriorly, Type 2: encased in bone between the healed displaced medial epicondyle and its bony bed, and Type 3: entrapped between the medial condyle and olecranon anteriorly.32 Al-Qattan described a fourth type that is a combination of types 1 and 2 where the nerve is encased in the healed medial epicondyle fracture, enters the joint posteriorly, and exits anteriorly33 (Figure 3).
Figure 3. From Tachdjian’s, redrawn from original Al-Qattan article.
Careful physical exam pre- and post-reduction can identify an iatrogenic nerve injury caused by joint entrapment during reduction. Continued ulnar nerve symptoms in conjunction with a medial epicondyle fracture, especially when the fragment is incarcerated, is considered an indication for timely open reduction and fixation. The intact, but often contused, ulnar nerve can be gently extricated and neurolysis can be performed at the time of surgery with every expectation that the neuropraxia will resolve. If there are any signs of nerve injury pre-reduction, a detailed neurologic exam of both motor and sensation are warranted to ensure that the exam is the same and not worsened after reduction. Any new onset or worsening of median or ulnar nerve injury after reduction warrants surgical exploration with release of the nerve. A chronically displaced medial nerve can be diagnosed radiographically by Matev’s sign, a sclerotic depression over the posteromedial epicondyle.34 In these cases, release and neurolysis are insufficient, and nerve reconstruction with nerve grafting is required (Figures 4 and 5).
Figure 4. Developing Matev’s sign (white arrows) signifying median nerve entrapment following an elbow fracture dislocation of the medial epiconyle.
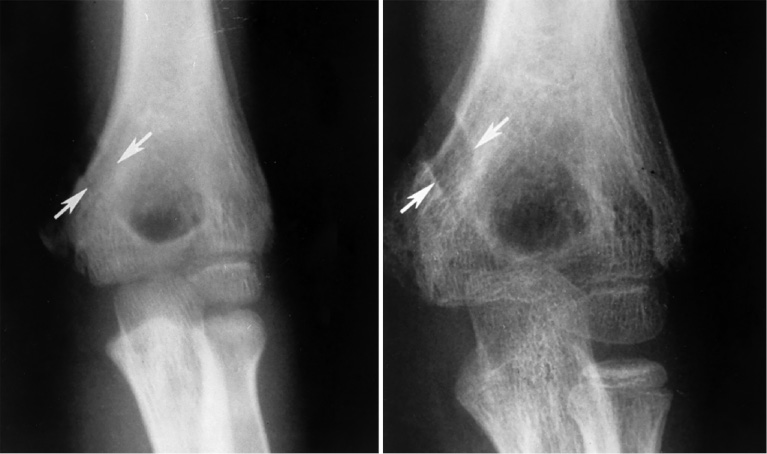
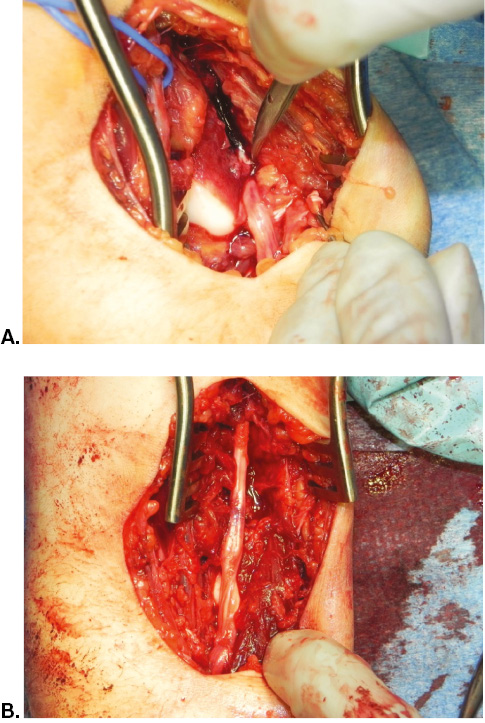
Figure 5. A 9-year-old female sustained a right elbow dislocation from a trampoline and underwent close reduction and splinting in the ED. She returned to the ED 24-48 hours later due to increasing pain and was noted at that time to have a new onset median nerve palsy. Ultrasound revealed that the median nerve dove posteriorly at the level of the elbow joint then re-appeared distal to the joint. She was brought to the operating room for exploration and retrieval of the median nerve that was incarcerated in the joint posteriorly. A). Blue vesi-loop is placed around the brachial artery proximal to the right elbow joint (proximal is at top of photo). A void is noted medial to the brachial artery where the median nerve should be. The median nerve is seen exiting distally from the ulnotrochlear joint. B). The extricated median nerve has an hourglass shape from the incarceration, and intraneural hemorrhage is present. Simple neurolysis was performed. Flexor pollicis longus function did not return until 6 months postoperatively although FDP to the index finger returned at 4 months. Return of 2-point discrimination was first documented to return at 10 months postoperatively. (Figures courtesy of Christine A. Ho, MD)
Monteggia Fracture-Dislocations
The most common nerve involved in Monteggia fracture-dislocations is the posterior interosseous nerve (PIN), due to its location in close proximity to the radial neck. Because the PIN branches off the radial nerve after the radial nerve innervates the wrist extensors, a PIN palsy will have intact wrist extension but loss of active finger and thumb extension as well as loss of supination. This occurs most commonly in Bado I (anteriorly dislocated radial head) and Bado III (laterally dislocated) fracture patterns with a reported incidence of 3-31%.35 The PIN palsy typically resolves with anatomic reduction of the radial head. It is the authors’ opinion that strong consideration should be given to acute surgical anatomic stabilization of the ulna to avoid further compression of the nerve in a cast molded with direct pressure on the nerve. While some have advocated for immediate surgical exploration in the setting of a PIN palsy with an irreducible Bado III pattern,36 this is controversial, and others have reported spontaneous resolution of the PIN after surgical stabilization without PIN exploration.35,37 There is one case report of successful nerve grafting of a PIN palsy 2 years after closed reduction of a Bado III Monteggia lesion.38
Tardy ulnar nerve palsies in the setting of remote (>40 years) Monteggia fracture dislocations with cubitus varus deformity and arthritis changes have been reported; anterior subcutaneous transposition of the ulnar nerve yielded good results, although the dislocated radial head and coronal plane deformity were untreated.39 Iatrogenic ulnar nerve and PIN palsies have also been reported after surgical treatment of chronic Monteggia fracture-dislocations,40–42 and because of this, some have advocated radial and ulnar nerve explorations at time of reconstruction.43,44
Forearm Fractures
Pediatric forearm fractures are a commonly treated fracture pattern, with the majority of them healing without complications. However, nerve injuries can be associated with these fractures and have been reported in the literature.45–48 As with any fracture or injured extremity, a comprehensive evaluation of the patient is crucial to identifying a nerve injury. Understanding the geographic anatomy and courses of the individual nerves will allow one to identify a nerve injury based on fracture pattern and location. Although beyond the scope of this article, we agree with our colleagues Drs. Bae and Waters that “it is imperative that all pediatric upper limb and hand surgeons know human nerve anatomy and innervation patterns.”49 Commonly described nerve injuries associated with midshaft forearm fractures include the posterior interosseous nerve, median nerve, or ulnar nerve, with the majority of these healing with complete resolution.46,48,50–52
It is difficult to state a true incidence for nerve injuries; however, constant vigilance and thorough neurologic examination from the start of the injury and subsequent follow-ups is paramount in identifying patients with an associated nerve injury. Fortunately, most neurologic deficits associated with closed pediatric fractures is contusion, which can be followed with nonoperative treatment and will resolve.53–56 On initial presentation to the ED or acute care facility, evaluation of open wounds should alert one to the possibility of a nerve injury. Federer et al.48 found an association with grade I open fractures with apex volar middle to distal one-third both-bone forearm shaft fractures and ulnar nerve deficit. In addition, they recommended acute operative intervention for a closed fracture pattern with distinct volar block to reduction in the setting of a dense ulnar nerve palsy.48 Suganuma et al.56 noted that ulnar nerve function can be affected by midshaft forearm fractures, especially in the middle and distal third of the diaphysis, secondary to close proximity between the nerve and the ulna. This has been corroborated by others who performed a cadaveric study noting the anatomic constraints in the middle to distal one-third forearm.48
Median nerve entrapment/injury has been described with associated radius and ulna shaft fractures. The location has been documented in proximal, midshaft, and distal third radius fractures as well as ulna fractures.57–59
Once a concomitant nerve injury has been identified, the next step is determining the type of injury: neuropraxia, neurotmesis, or axonotmesis. Majority of these will be a neuropraxia60 and as stated above, will resolve with non-operative treatment. Federer et al.48 developed an algorithm for ulnar nerve injuries associated with pediatric forearm fractures. They recommended serial neurological exams looking at nerve specific symptoms (Froment sign, ulnar clawing, hypothenar wasting, and advancing Tinel sign). They support EMG/NCS in age-appropriate children at 3-6 weeks from injury. This can also act as a baseline. Typically, there will be improvement between 8-12 weeks postinjury;48,56,61 however, if improvement is not seen after this time frame, then they recommended repeat EMG/NCS. If this shows monophasic motor unit action potentials and increased latency, then nerve exploration is recommended. If there are signs of nerve recovery, then one can continued with observation and conservative management61 (Figure 6).
Figure 6. Grade I open left forearm fracture in an 11-year-old treated with I&D, closed reduction and casting, and intravenous antibiotics. Note volar gapping of ulna on reduction fluoroscopy. At 4-week follow-up, she was noted to have tethering of extrinsic finger flexors as well as decreased sensation in ulnar nerve distribution. Intraoperatively, the Flexor Digitorum Profundus muscle belly and ulnar nerve were entrapped in the gapped ulna fracture site (red arrow). Extrinsic finger contractures and ulnar nerve symptoms resolved after release of the muscle belly and nerve and ORIF of the ulna fracture. (Figures courtesy of Hilton P. Gottschalk, MD)

Management of Nerve Injuries
In the immediate postoperative period, careful, targeted serial clinical examinations are all that is needed to document nerve recovery. Examination of motor strength with gravity eliminated, especially in radial nerve injuries, improvement of clawing (in ulnar nerve injuries), and a progressing Tinel’s sign can help to identify early recovery. The authors do not obtain further studies as long as there is clear identification and documentation of progressive nerve recovery. If there are absolutely no signs of recovery in 3-4 months, the authors agree that timely referral to a pediatric hand/upper extremity surgeon or hand surgeon should be considered in addition to further diagnostic studies.
Diagnostic Studies
Physical Exam
A careful physical examination is important to identify nerve injuries in the setting of a pediatric upper extremity fracture. In the pediatric patient, examination of the peripheral nervous system can be challenging, especially in the acute setting. In children older than four, a patient clinician can usually obtain a thorough examination. Examining the uninjured side first can inform the clinician as to the child’s ability to follow instructions and comply with the exam. Examination prior to intervention, either a reduction attempt or surgical intervention, aids the surgeon in counseling parents and prevents confusion about the time of onset of the nerve injury.
In the acute setting, the physical examination should focus on first identifying and then localizing the nerve injury. The anterior interosseous (AIN), Posterior interosseous (PIN), and ulnar nerves are assessed with a series of instructions that are age appropriate. Patients are asked to give a thumbs up (PIN), make an OK sign (AIN), and to spread their fingers wide (ulnar). Young patients will rapidly learn adaptive maneuvers in the setting of a peripheral nerve injury that can falsely reassure the examiner. For instance, they may use tenodesis to aid in thumb and finger extension. Isolating the thumb to examine IP joint flexion (FPL, AIN) and extension (EPL, PIN) allows a precise exam of two nerves without causing undue pain to the injured child. Examination of sensation can be challenging in young patients. When possible, we attempt to examine autonomous areas of sensation: dorsal first web space for the radial nerve, volar index finger for the median nerve, and volar small finger for the ulnar nerve. The wrinkle test can also be used to identify nerve injuries and is especially useful in the young patient. Intact nerves mediate normal skin wrinkling when exposed to moisture. A hand placed in warm water will not wrinkle in the distribution of an injured nerve, while the uninjured distributions will have normal skin wrinkles. Careful tactile examination and comparison of the sweat pattern of the fingers can also identify nerve injury, especially in the nonverbal age group. The sudomotor function of the sweat glands is lost immediately in the distribution of an injured nerve. In chronic dense nerve palsies, the affected fingers will be cool, dry, have flaking skin, and even have dystrophic nails.
In the subacute setting, physical examination aims to identify signs of recovery. Serial examination may demonstrate an advancing Tinel’s sign.62 The location of the Tinel’s sign is measured from a fixed point (e.g., wrist flexion crease) and documented at each appointment. Nerve recovery occurs at approximately 1 mm per day or about 1 inch per month after a lag time of 1 month post injury. Additionally, knowing the order of innervation of the muscles in the upper extremity can aid the clinician in physical examination. Knowing the rate of recovery and order of innervation allows the examiner to predict timing of nerve recovery or lack thereof.
EMG/NCV
Electrodiagnostic studies (EDx) can be a useful adjunct to clinical examination when evaluating pediatric patients with a peripheral nerve injury. The exact timing of obtaining nerve conduction (NCS) and electromyogram (EMG) studies remains controversial. In the young or anxious pediatric patient, sedation may be required to obtain EDx. This is supported by a retrospective review of 725 electrodiagnostic studies performed in the pediatric population,63 where 94.5% of patients underwent an awake EDx with 4.8% of studies terminated early for patient intolerance. The authors concluded that early termination was more likely in patients less than 10 years old. If sedation is required, the volitional part of the exam, namely the EMG, may not be obtainable. Interestingly, Alshaikh and colleagues found that pediatric patients perceived pain as moderate during EDx.64 In their study, the NCS was tolerated better than the EMG portion of the examination. EMG sampling of more than one muscle and proximal sampling was associated with increased perception of pain. Anecdotally, the authors’ institutions have a low threshold for sedation if the child is unwilling or uncooperative with the nerve conduction test. Access to an experienced pediatric neurologist or physiatrist helps mitigate these issues. In addition, normative values for nerve conduction velocity are significantly different than those in adults, and care must be taken in interpreting study results.65
The timing of initial EDx remains variable. Some authors have suggested baseline studies after a peripheral nerve injury. However, given the potential difficulties in obtaining EDx in pediatric patients the authors have waited to obtain studies when recovery has not occurred at the expected time or has failed to progress. Given that most pediatric nerve injuries are neuropraxias this strategy avoids unnecessary testing. However, if no recovery is seen at 3-4 months post injury, EDx are obtained. Another useful rule is that nerve recovery should occur at about 1mm per day or approximately 1 inch per month. The interpretation of EDx is beyond the scope of this review. However, excellent reviews are available for the interested reader.66
Nerve MRI
While not routinely indicated, MRI has been advocated by some to help identify nerve entrapment and the extent of nerve injury.48,58,59,67,68 The small caliber and winding course of peripheral nerves in the upper extremity make evaluation particularly challenging in children.69 Imaging can be optimized by neurography techniques, using a 3-T scanner, and use of the smallest body coil that fits tightly around the area of interest. A fusiform neuroma of an intact nerve will demonstrate enlargement with intermediate T1 signal and higher T2 signal, along with a ring-like fascicular pattern on axial T2 images. Meanwhile, a nerve with partial or complete transection will show an entering nerve ending in bulbous enlargement. In addition to the nerve itself, resultant muscle denervation can be apparent after about 1 month with hyperintensity on T2 sequences acutely. After 12 months, chronic denervation will be apparent by fatty infiltration on T1 images. What these studies have in common and support is that if the course of the nerve is affected by the fracture, then that can be evaluated on MRI and will show deviation of the nerve and entrapment.
One retrospective study found MRI to detect and prognostically classify upper extremity nerve lesions with associated fractures in 10 of 12 children.70 Practical considerations include the potential need for anesthesia to reduce motion artifact in younger children, as acquisition times range from 45-90 minutes.70 Most children over age 9 can tolerate a non-sedated study,71 with some as young as 5-7 able to have minimal motion artifact if the extremity is immobilized.
Ultrasound
Neuromuscular ultrasound (US) is relatively inexpensive, painless, avoids the need for sedation in a young child, is not limited by the presence of metal implants, and can aid in localization and diagnosis of traumatic nerve lesions in sonographically accessible regions of the upper limb. US can determine if the nerve is in continuity and identify transected ends as well as anatomic landmarks. US can identify a neuroma in continuity or neuroma at a transected end, and visualize compression of the nerve by bone, scarring, implants, or other structures. Neuromas-in-continuity can be evaluated with some accuracy for the lack of continuity of axons, endoneurium, and perineurium with intact epineurium, which give information regarding prognosis and surgical planning.72
US evaluation of an acute nerve transection can allow early, direct nerve repair, while US evaluation in the chronic setting can also allow localization of the contracted, transected ends as well as estimation of gap length to plan for graft length and type preoperatively. Quality of the images and interpretation is of course user-dependent and requires both an experienced and skilled US technologist as well as radiologist. Given the increased access of US in the operating room to allow anesthesiologists to safely perform peripheral nerve blocks, US could potentially be used intraoperatively to safely identify nerve entrapment or tethering that might prompt immediate nerve exploration/decompression at the time of surgical fixation73 (Figure 7).
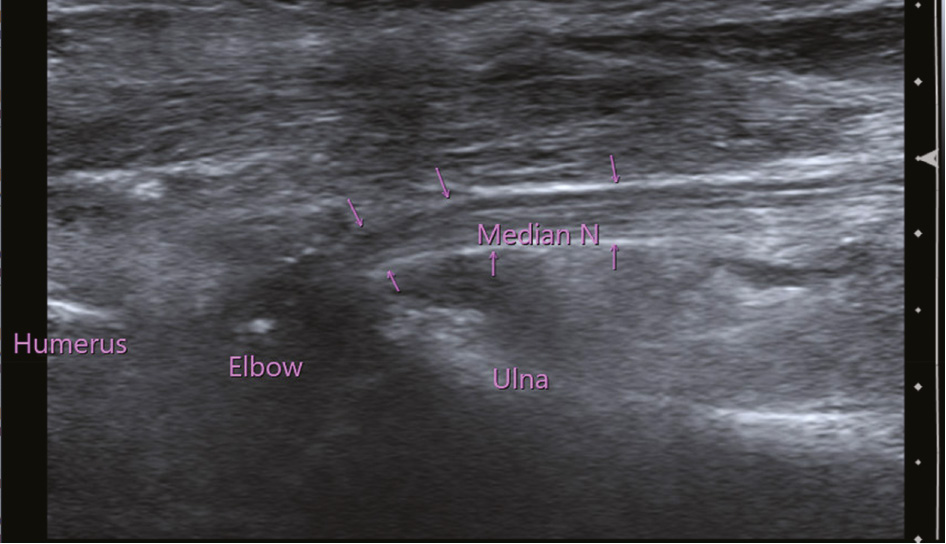
Figure 7. New onset dense median nerve palsy after closed reduction of an isolated elbow dislocation. Ultrasound demonstrated an incarcerated median nerve exiting the elbow joint from a lateral view. (Figure courtesy of Christine A. Ho, MD)
Summary
While nerve injuries occur not infrequently with pediatric upper extremity fractures, the level of comfort regarding management of the nerve injuries varies amongst pediatric orthopaedists, especially when the nerve injury does not show clinical signs of improvement within the first 4-6 weeks. Ultrasound and nerve MRI can help show structural entrapment and nerve continuity, while EDx are useful in determining return of nerve conduction, especially when used serially in the setting of lack of clinical improvement. It is the hope of the authors that this review article offers reassurance as well as guidance to our colleagues as when these patients should be referred to a colleague who specializes in pediatric hand/upper extremity.
Disclaimer
No funding was received. The authors have no conflicts of interest to report related to this manuscript.
*POSNA QSVI Hand/Upper Extremity Committee: Christine A. Ho, MD; Sonia Chaudhry, MD; Krister P. Freese, MD; Hilton P. Gottschalk, MD; Julie Balch Samora, MD, PhD, MPH; Selina Poon, MD.
References
- Wiktor L, Tomaszewski R. Treatment of radial nerve palsy in paediatric humeral shaft fractures. STROBE-Compliant Investigation. Medicina (Kaunas). 2022;58(11):1571.
- Shao YC, Harwood P, Grotz MR, et al. Radial nerve palsy associated with fractures of the shaft of the humerus: a systematic review. J Bone Joint Surg Br. 2005;87(12):1647-1652.
- Aman M, Zimmermann KS, Boecker AH, et al. Peripheral nerve injuries in children-prevalence, mechanisms and concomitant injuries: a major trauma center’s experience. Eur J Med Res. 2023;28(1):116.
- O’Shea R, Panwar J, Chu Kwan W, et al. Establishing safe zones to avoid nerve injury in the approach to the humerus in pediatric patients: a magnetic resonance imaging study. J Bone Joint Surg Am. 2019;101(23):2101-2110.
- Singh V, Hayes HV, Kazemi N, et al. The Holstein-Lewis humerus shaft fracture in children: are they different from adults? J Pediatr Orthop B. 2022;31(3):274-280.
- Koch PP, Gross DF, Gerber C. The results of functional (Sarmiento) bracing of humeral shaft fractures. J Shoulder Elbow Surg. 2002;11(2):143-150.
- Runner R, Whicker E, De S. Delayed radial nerve palsy after closed reduction of a pediatric humeral shaft fracture. Case Rep Orthop. 2017;2017:9723497.
- O’Shaughnessy MA, Parry JA, Liu H, et al. Management of paediatric humeral shaft fractures and associated nerve palsy. J Child Orthop. 2019;13(5):508-515.
- Bertelli J, Soldado F, Ghizoni MF. Outcomes of radial nerve grafting in children after distal humerus fracture. J Hand Surg Am. 2018;43(12):1140 e1141-1140 e1146.
- Chaudhry S, Ipaktchi KR, Ignatiuk A. Updates on and controversies related to management of radial nerve injuries. J Am Acad Orthop Surg. 2019;27(6):e280-e284.
- Grass G, Kabir K, Ohse J, et al. Primary exploration of radial nerve is not required for radial nerve palsy while treating humerus shaft fractures with unreamed humerus nails (UHN). Open Orthop J. 2011;5:319-323.
- Schultz JD, Rees AB, Wollenman LC, et al. Bruise location in supracondylar humerus fractures predicts specific neurovascular injuries. J Pediatr Orthop. 2022;42(3):e250-e256.
- Garg S, Weller A, Larson AN, et al. Clinical characteristics of severe supracondylar humerus fractures in children. J Pediatr Orthop. 2014;34(1):34-39.
- Cramer KE, Green NE, Devito DP. Incidence of anterior interosseous nerve palsy in supracondylar humerus fractures in children. J Pediatr Orthop. 1993;13(4):502-505.
- Babal JC, Mehlman CT, Klein G. Nerve injuries associated with pediatric supracondylar humeral fractures: a meta-analysis. J Pediatr Orthop. 2010;30(3):253-263.
- Kim KY, Conaway W, Schell R, et al. Prevalence of ulnar nerve palsy with flexion-type supracondylar fractures of the humerus. J Pediatr Orthop B. 2020;29(2):133-136.
- Shore BJ, Gillespie BT, Miller PE, et al. Recovery of motor nerve injuries associated with displaced, extension-type pediatric supracondylar humerus fractures. J Pediatr Orthop. 2019;39(9):e652-e656.
- Ozcan M, Altinoz O, Erem M, et al. Prognosis and risk factors of nerve injuries in displaced pediatric supracondylar humerus fractures. Niger J Clin Pract. 2020;23(5):647-653.
- Harris LR, Arkader A, Broom A, et al. Pulseless supracondylar humerus fracture with anterior interosseous nerve or median nerve injury-an absolute indication for open reduction? J Pediatr Orthop. 2019;39(1):e1-e7.
- Skaggs DL, Hale JM, Bassett J, et al. Operative treatment of supracondylar fractures of the humerus in children. The consequences of pin placement. J Bone Joint Surg Am. 2001;83(5):735-740.
- Joiner ER, Skaggs DL, Arkader A, et al. Iatrogenic nerve injuries in the treatment of supracondylar humerus fractures: are we really just missing nerve injuries on preoperative examination? J Pediatr Orthop. 2014;34(4):388-392.
- Dekker AE, Krijnen P, Schipper IB. Results of crossed versus lateral entry K-wire fixation of displaced pediatric supracondylar humeral fractures: a systematic review and meta-analysis. Injury. 2016;47(11):2391-2398.
- Brauer CA, Lee BM, Bae DS, et al. A systematic review of medial and lateral entry pinning versus lateral entry pinning for supracondylar fractures of the humerus. J Pediatr Orthop. 2007;27(2):181-186.
- Slobogean BL, Jackman H, Tennant S, et al. Iatrogenic ulnar nerve injury after the surgical treatment of displaced supracondylar fractures of the humerus: number needed to harm, a systematic review. J Pediatr Orthop. 2010;30(5):430-436.
- Ozcelik A, Tekcan A, Omeroglu H. Correlation between iatrogenic ulnar nerve injury and angular insertion of the medial pin in supracondylar humerus fractures. J Pediatr Orthop B. 2006;15(1):58-61.
- Rees AB, Schultz JD, Wollenman LC, et al. A mini-open approach to medial pinning in pediatric supracondylar humeral fractures may be safer than previously thought. J Bone Joint Surg Am. 2022;104(1):33-40.
- Green DW, Widmann RF, Frank JS, et al. Low incidence of ulnar nerve injury with crossed pin placement for pediatric supracondylar humerus fractures using a mini-open technique. J Orthop Trauma. 2005;19(3):158-163.
- Khademolhosseini M, Abd Rashid AH, Ibrahim S. Nerve injuries in supracondylar fractures of the humerus in children: is nerve exploration indicated? J Pediatr Orthop B. 2013;22(2):123-126.
- Graff C, Dounas GD, Sung J, et al. Management of iatrogenic ulnar nerve palsies after cross pinning of pediatric supracondylar humerus fractures: a systematic review. J Child Orthop. 2022;16(5):366-373.
- Royce RO, Dutkowsky JP, Kasser JR, et al. Neurologic complications after K-wire fixation of supracondylar humerus fractures in children. J Pediatr Orthop. 1991;11(2):191-194.
- Rasool MN. Ulnar nerve injury after K-wire fixation of supracondylar humerus fractures in children. J Pediatr Orthop. 1998;18(5):686-690.
- Fourrier P, Levai JP, Collin JP. [Median nerve entrapment in elbow dislocation]. Rev Chir Orthop Reparatrice Appar Mot. 1977;63(1):13-16.
- al-Qattan MM, Zuker RM, Weinberg MJ. Type 4 median nerve entrapment after elbow dislocation. J Hand Surg Br. 1994;19(5):613-615.
- Matev I. A radiological sign of entrapment of the median nerve in the elbow joint after posterior dislocation. A report of two cases. J Bone Joint Surg Br. 1976;58(3):353-355.
- Demirel M, Saglam Y, Tunali O. Posterior interosseous nerve palsy associated with neglected pediatric Monteggia fracture-dislocation: a case report. Int J Surg Case Rep. 2016;27:102-106.
- Li H, Cai QX, Shen PQ, et al. Posterior interosseous nerve entrapment after Monteggia fracture-dislocation in children. Chin J Traumatol. 2013;16(3):131-135.
- Yoshida N, Tsuchida Y. Posterior interosseous nerve palsy due to Bado type-III Monteggia fracture. BMJ Case Rep. 2018;2018:bcr2018226254.
- Copeland AE, Gormley J, Chin B, et al. Nerve grafting for chronic PIN palsy due to radiocapitellar joint entrapment 2 years following closed reduction of a pediatric monteggia fracture-dislocation: a case report with 1-year follow-up. Hand (N Y). 2021;16(6):NP10-NP14.
- Nishimura M, Itsubo T, Horii E, et al. Tardy ulnar nerve palsy caused by chronic radial head dislocation after Monteggia fracture: a report of two cases. J Pediatr Orthop B. 2016;25(5):450-453.
- Tan SHS, Low JY, Chen H, et al. Surgical management of missed pediatric monteggia fractures: a systematic review and meta-analysis. J Orthop Trauma. 2022;36(2):65-73.
- Rodgers WB, Waters PM, Hall JE. Chronic Monteggia lesions in children. Complications and results of reconstruction. J Bone Joint Surg Am. 1996;78(9):1322-1329.
- Di Gennaro GL, Martinelli A, Bettuzzi C, et al. Outcomes after surgical treatment of missed Monteggia fractures in children. Musculoskelet Surg. 2015;99 Suppl 1:S75-S82.
- Zheng ET, Waters PM, Vuillermin CB, et al. Surgical reconstruction of missed Monteggia lesions in children. J Pediatr Orthop. 2020;40(10):e916-e921.
- Ring D, Jupiter JB, Waters PM. Monteggia fractures in children and adults. J Am Acad Orthop Surg. 1998;6(4):215-224.
- Rennie L, Court-Brown CM, Mok JY, et al. The epidemiology of fractures in children. Injury. 2007;38(8):913-922.
- Nunley JA, Urbaniak JR. Partial bony entrapment of the median nerve in a greenstick fracture of the ulna. J Hand Surg Am. 1980;5(6):557-559.
- Neiman R, Maiocco B, Deeney VF. Ulnar nerve injury after closed forearm fractures in children. J Pediatr Orthop. 1998;18(5):683-685.
- Federer AE, Murphy JS, Calandruccio JH, et al. Ulnar nerve injury in pediatric midshaft forearm fractures: a case series. J Orthop Trauma. 2018;32(9):e359-e365.
- Waters PM, Bae DS. Pediatric Hand and Upper Limb Surgery: A Practical Guide. Lippincott Williams & Wiklins; 2012.
- Luhmann SJ, Schootman M, Schoenecker PL, et al. Complications and outcomes of open pediatric forearm fractures. J Pediatr Orthop. 2004;24(1):1-6.
- Lichter RL, Jacobsen T. Tardy palsy of the posterior interosseous nerve with a Monteggia fracture. J Bone Joint Surg Am. 1975;57(1):124-125.
- Hutchison RL, Wester CJ. Median nerve entrapment in the ulna in a both-bone pediatric forearm fracture: case report and review of the literature. Pediatr Emerg Care. 2019;35(11):e220-e222.
- Omer GE, Jr. Injuries to nerves of the upper extremity. J Bone Joint Surg Am. 1974;56(8):1615-1624.
- Quan D, Bird S. Nerve conduction studies and electromyography in the evaluaiton of perepheral nerve injuries. Univ Pennsylavania Orthop J. 1999;12:45-51.
- Stahl S, Rozen N, Michaelson M. Ulnar nerve injury following midshaft forearm fractures in children. J Hand Surg Br. 1997;22(6):788-789.
- Suganuma S, Tada K, Hayashi H, et al. Ulnar nerve palsy associated with closed midshaft forearm fractures. Orthopedics. 2012;35(11):e1680-e1683.
- al-Qattan MM, Clarke HM, Zimmer P. Radiological signs of entrapment of the median nerve in forearm shaft fractures. J Hand Surg Br. 1994;19(6):713-719.
- Fourati A, Ghorbel I, Karra A, et al. Median nerve entrapment in a callus fracture following a pediatric both-bone forearm fracture: a case report and literature review. Arch Plast Surg. 2019;46(2):171-175.
- Yeo G, Prodger S, Latendresse K. Median nerve entrapment in a paediatric fracture of the ulna demonstrated by magnetic resonance imaging. J Hand Surg Eur Vol. 2011;36(4):329-330.
- Stavrakakis IM, Daskalakis II, Magarakis GE, et al. Ulnar nerve injuries post closed forearm fractures in paediatric population: a review of the literature. Clin Med Insights Pediatr. 2019;13:1179556519841876.
- Mohler LR, Hanel DP. Closed fractures complicated by peripheral nerve injury. J Am Acad Orthop Surg. 2006;14(1):32-37.
- Hoffmann P, Buck-Gramcko D, Lubahn JD. The hoffmann-tinel sign. 1915. J Hand Surg Br. 1993;18(6):800-805.
- Joyal KM, MacGregor JV, Hayawi LM, et al. Not so shocking: electromyography in pediatrics remains feasible and diagnostically useful. Can J Neurol Sci. 2022;49(5):696-702.
- Alshaikh NM, Martinez JP, Pitt MC. Perception of pain during electromyography in children: a prospective study. Muscle Nerve. 2016;54(3):422-426.
- Ryan CS, Conlee EM, Sharma R, et al. Nerve conduction normal values for electrodiagnosis in pediatric patients. Muscle Nerve. 2019;60(2):155-160.
- Pripotnev S, Bucelli RC, Patterson JMM, et al. Interpreting electrodiagnostic studies for the management of nerve injury. J Hand Surg Am. 2022;47(9):881-889.
- Sneag DB, Curlin J, Saltzman EB, et al. Role of high-resolution peripheral nerve magnetic resonance imaging in diagnosing median nerve tethering in a case of both-bone forearm fracture in a child. Pediatr Radiol. 2021;51(1):148-151.
- Yanagibayashi S, Yamamoto N, Yoshida R, et al. Magnetic resonance imaging visualizes median nerve entrapment due to radius fracture and allows immediate surgical release. Case Rep Orthop. 2015;2015:703790.
- Cortes C, Ramos Y, Restrepo R, et al. Practical magnetic resonance imaging evaluation of peripheral nerves in children: magnetic resonance neurography. Radiol Clin North Am. 2013;51(4):673-688.
- Sondermann S, Bäumer T, Suss J, et al. Detection of Traumatic and Postoperative Nerve Lesions following Upper Extremity Fractures in a Pediatric Cohort Using MR Neurography. Eur J Pediatr Surg. 2022 Jul 19. doi: 10.1055/s-0042-1751221. Epub ahead of print. PMID: 35853469.
- Chaudhry S. Upper extremity care for children: unique medical and psychosocial aspects. J Hand Surg Am. 2019;44(7):606-609.
- Zhu J, Liu F, Li D, et al. Preliminary study of the types of traumatic peripheral nerve injuries by ultrasound. Eur Radiol. 2011;21(5):1097-1101.
- Tokutake K, Okui N, Hirata H. Primary radial nerve exploration determined by ultrasound in pediatric supracondylar humerus fracture: a report of two cases. J Hand Surg Asian Pac Vol. 2021;26(2):284-289.
