Current Concept Review
Orthopaedics and Biomedical Engineering Design: An Innovative Duet toward a Better Tomorrow
1Department of Orthopaedic Surgery, Nemours Children’s Hospital, Delaware, Wilmington, DE; 2Department of Biomedical Engineering, University of Delaware, Newark, DE; 3Department of Biomedical Engineering, University of Wisconsin–Madison, Madison, WI; 4School of Medicine and Public Health, Department of Orthopedics and Rehabilitation, University of Wisconsin–Madison, Madison, WI
Correspondence: John P. Puccinelli, PhD, Department of Biomedical Engineering, University of Wisconsin–Madison, Engineering Centers Building, Rm. 2132, 1550 Engineering Drive, Madison, WI 53706-1609. E-mail: [email protected]; Alvin W. Su, MD, PhD, Department of Orthopaedic Surgery, Nemours Children’s Hospital, Delaware, 1600 Rockland Road Wilmington, DE 19803. E-mail: [email protected]
Received: March 21, 2023; Accepted: April 5, 2023; Published: May 1, 2023
Volume 5, Number 2, May 2023
Abstract
The main purpose of this article is to explore the benefits and dynamics of collaborations between orthopaedic surgeons and biomedical engineering (BME) undergraduates and faculties in the context of engineering design programs as well as clinical immersion programs. An outline of strategies to navigate the seemingly complex landscape of hospitals and universities is presented through models of orthopaedic-BME collaborations at two distinct academic practice settings in the United States. In addition to (four) examples of BME design projects sponsored by the clinicians, funding and intellectual property (IP), priority of time management, as well as the positive impact on student education are also discussed. Design collaborations can provide unique educational and research opportunities for the development of undergraduate engineering students to become future leaders; at the same time, this simultaneously facilitates innovative solutions fulfilling unmet clinical needs for orthopaedic clinicians. Overall, we hope to provide references and resources for pediatric orthopaedists who are interested in participating in similar orthopaedic-BME design framework for future innovation and student education in real-life orthopaedic research translation.
Key Concepts
- The “duet” partnership between orthopaedics and biomedical engineering can bring a paradigm shift in orthopaedic surgery.
- Such a collaboration model introduces the BME students to real-world clinical needs and a potential future career trajectory; in return, this also offers the orthopaedists the opportunity to fulfill unmet clinical needs, offer better patient care, as well as understand the process of research and design (R&D) in engineering.
- The IP issue is complex and often related to the funding source; it is well worth the time for both the orthopaedist and the BME student to comprehend and negotiate IP before the project commences.
- Making time and effort to “join the team” in person with BME is tremendous for the team morale, in addition to remotely providing clinical perspectives—albeit challenging for full-time orthopaedic surgeons.
- References #3 (ABET, United States) and #4 (Engineers Canada, Canada) provide a comprehensive list of contacts of BME programs that would be excellent partners for orthopaedic collaborations.
Introduction
The evolution of orthopaedic surgery has been closely tied to advances in technology via biomedical engineering (BME). BME encompasses “the application of engineering principles, practices, and technologies to the fields of medicine and biology, especially in solving problems and improving care.”1 Diagnostic imaging, various kinds of casts and braces, the gait laboratory, surgical instruments, and implants are all examples of successful biomedical solutions to meet the needs of daily orthopaedic surgery practice. It is this close collaboration between the two disciplines that has allowed advances in both fields, thus positively impacting the paradigm of patient care across generations.
In pediatric orthopaedics, we have the privilege of helping patients from babies to young adults. As a result, patients and their families have distinct expectations and needs at various stages of their life. The spectrum of clinical problems is wide, and there is always more to be learned and solved. Early immersion of young talents from BME programs into the clinical needs of pediatric orthopaedics enroots our future hope of groundbreaking solutions. Throughout this process, the surgeon also benefits from a better understanding of research and development (R&D) in BME.
Models of Orthopaedics-BME Collaboration
The number of BME programs has been rapidly growing.2 The latest list of accredited programs that would be excellent orthopaedic collaborators can be found in the U.S. through ABET3 and Canada through Engineers Canada.4 All accredited programs require at least one semester of senior capstone design where teams are usually composed of all undergraduate students working to solve real-world problems. Corporate senior design project sponsors often have specific medical device-related needs for which they engage with senior design teams. Alternatively, the problem can also be identified through a course where students participate in a clinical immersion experience to perform needs identification.5 In addition, teams may also have a clinical client, like an orthopaedic surgeon or a nurse practitioner, who proposes the biomedical problem to be solved (outside of the typical clinical immersion experience). The orthopaedic surgeons may come from an orthopaedic department under the same university umbrella or an independent institution; they serve as the “clinical sponsors” for the senior design project. Concurrently, each team and project will also have a faculty advisor (professor) from the same or an affiliated undergraduate engineering program.
Orthopaedic surgeons typically find it a very rewarding experience to guide students in addressing an unmet need in their practice, explaining why the need is important and how the result would help patients. While a lot of prototyping happens virtually or on the university campus, some teams also come to shadow surgeons in the clinics or in the operating room. Every so often, the students identify potential areas of improvement while they observe the clinical practice and even come up with a creative “flash of genius” that is distinct from traditional perspectives. While surgeons provide valuable feedback in terms of what will or will not work in real life, they also learn how to better translate the constraints and wants into clearly defined engineering goals and action items. Overall, this is an excellent model of mutual learning that sets the foundation for greater future impact in orthopaedic engineering translation.
The scope of this manuscript focuses on the BME Student–Orthopaedic Surgeon model, of which we provide two examples below: University of Delaware (UD) and Nemours (duPont) Children’s Hospital, Delaware as well as the University of Wisconsin–Madison (UW), College of Engineering and UW Health System.
University of Delaware–Nemours (A.I. duPont) Children’s Hospital
The BME program at the University of Delaware (UD) includes a sophomore course which introduces students to the fundamentals of medical device design. In the “junior design” course, teams of three to five students work to come up with their own independent solution for the same problem. This prepares them for the “senior design” course,6 where each team works with their own project sponsor (i.e., different design projects for different teams) and they complete their individual design project in one semester. Senior design is interdisciplinary in nature, with biomedical, mechanical, electrical, as well as civil and environmental engineering students participating based on the scope and nature of the project. If needed, teams have the option to continue working on the project as an independent study course over the next semester. Efforts culminate into conference proceedings, publications, patents, as well as full-time employment opportunities. These courses prepare students to be competitive in the real-life job market, where clinicians and medical device companies expect results in a matter of months.
The partnership between Nemours Children’s Hospital (Nemours) and UD–BME has over 6 years of history. Senior design students meet weekly with the faculty advisor and their clinical mentor (project sponsor) to review progress and design prototype. Four deliverables are expected: Problem Definition, Concept Generation, Design Details, and Design Validation. In addition, four internal and external oral deliverables are expected. While internal reviews are opportunities for feedback from faculty on the teaching and manufacturing team, external reviews require students to present their work to industry scientists, engineers, and clinicians. Lastly, the team is expected to present a working prototype at the end of the semester. We provide two example projects below.
Project 1: Design of an Adaptable Device to Help Bicycle Steering with One Hand for Children with Unilateral Congenital Below Elbow Deficiency, sponsored by Dr. Jennifer Ty
Background: Approximately 1 in 1,900 babies are born with unilateral congenital below-elbow deficiencies (UCBED) in the United States.7 Children with this condition are able to partake in almost all everyday activities without difficulty, and many choose not to wear a prosthesis on a daily basis.8–11 However, learning to ride a bicycle can pose a special challenge, as these children may have trouble establishing steering control and balance. The few solutions to this clinical need are costly and not typically geared or sized for children or are “medicalized.” Adaptive mounts or bicycles can be expensive and are either sized for adults or do not grow with the child, which can make this an inaccessible choice for families. Some children may obtain a special prosthesis or orthosis specifically for this need, but this can be costly. Lastly, while steering dampers are safe and effective, they do not help children learn motor control skills. Of note, during the development of our project, a children’s bicycle manufacturer had also begun to design customizable bicycles with modifications for children with UCBED.12
The unmet need: To develop a device to help children with unilateral congenital below-elbow deficiencies to independently and safely ride a bike.
Design constraints and wants: This device must be safe in the event of a fall, adjustable, portable, compatible with existing children’s bicycles, a guaranteed fit for the end user, reasonably mobile, prototyped within the allocated budget ($500), with a cost of less than $50. This device should be one singular device, aesthetically pleasing, durable, comfortable, inexpensive, breathable, easy to clean, easy to use, and have substantial longevity. Additionally, the device should neither be swallowable nor should it use sub-components that are hard to replace.
Final design deliverables: The final design was a multi-part assembly of a sized silicone socket, retractable aluminum tubing, a ball and socket joint, and a handlebar clamp. The device was secured together via a locking clamp and the silicone socket, adjustable tubing, and handlebar clamp were held together with medium-strength magnets. Candidate materials for each component were rigorously tested individually and then as a completed device to ensure that the device met all requirements (Figure 1).
Figure 1. Fully assembled final device showing multiple socket sizes and adjustable tubing to help children with unilateral congenital below-elbow deficiencies to independently and safely learn how to ride a bike.

Design goal check: As shown in Video 1, the device secures to a children’s bicycle (Figure 2) easily, is adjustable in height to allow for residual limb lengths of different lengths, allows for appropriate range of motion (with the option to tighten the range if children are just learning to ride), and is compatible with sockets of different sizes. Additionally, if there is a fall, the device detaches, decreasing the risk to the rider. The device passed adjustability, portability, compatibility, range of motion, and safety metrics, and the device was projected to cost $56.44.
Figure 2. Device attached to a bike.

Future directions: The device has some areas of improvement, including but not limited to adjusting manufacturing processes to reduce per unit costs. Based on feedback from end users and their families, this device can be adjusted as needed.
Project 2: Development and Optimization of a Low-Cost Motion Capture System to Analyze Joint Kinematics During Martial Arts Movement, sponsored by Dr. Alvin Su
Background: Youth participation in martial arts has been increasing, and so have the related orthopaedic injuries, which commonly involve the knee, the hip, the shoulder, and the elbow.13 Understanding the kinematics and kinetics of injury and examining correct technique execution may benefit injury prevention as well as return-to-martial arts after injury.14,15 There are a number of expensive, high-end laboratory-based motion capture systems on the market.16–18 On the other end of the spectrum, there are lower-cost animation systems such as the Wii remotes.19 The data extraction process can be challenging, and the reliability of such data for martial arts is uncertain.
The unmet need: A motion capture system that is handy for clinicians and martial arts instructors to analyze martial arts movement of youth practitioners. Ideally, the system should be affordable and highly portable to where the youth practitioners are (clinics, laboratories, martial arts studios).
Design constraints and wants: The system should be low cost (less than $2,000) and portable, with an accuracy, precision in 95% agreement compared to gold standard, data collection speed above 100 Hz, and the ability to perform in a less controlled environment. The system should consider the comfort and safety of the tested subject wearing the device, ability to capture motion (kinematics) specific to martial arts, have a simple user interface, be suitable for multiple styles of martial arts, easy to set up, have easy data output and reduction, and the ability to capture kinetic data.
Final design deliverables: An exo-suit was developed with eight Inertial Measurement Units (IMUs) that are connected to an Arduino (microcontroller) in parallel via wires (Figure 3). Each IMU was secured in lightweight acrylic casings that were attached to the body via VELCRO® Brand strips and nylon webbings. IMU data was transmitted wirelessly to a computer, where joint angles are calculated and converted into a user-friendly Graphical User Interface (GUI, Figure 4). Clinical advice and input were invaluable to the team while determining design details, such as the number and location of IMUs to best capture martial arts movements and potential injuries. Simultaneous data acquisition on martial arts movements at a well-established motion laboratory at the University of Delaware was performed to serve as the gold standard for calibration.
Figure 3. Exo-skeleton concept of applying multiple IMUs (yellow) that are wired to the central Arduino (microcontroller, green); note that the IMUs are housed in acrylic cases and secured to the body using nylon straps and VELCRO® Brand strips.

Figure 4. (A) Workflow of application under GUI: acquiring the motion data, comparing the motion to the same technique done by experienced instructors, and identifying the discrepancies for technique correction and improvement. (B) An example of analyzing “axe kick” and comparing one person’s motion to another.

Design goal check: The system was comfortable for the subject wearing it and posed no electrical hazards, as shown in Video 2. It was easy to set up (less than 30 minutes) and easy to operate using the Python program in the laptop. It functioned well for three martial arts styles: Karate, Taekwondo, and boxing throughout the range of motion in these styles. It was portable and low profile. The final design cost was within budget, and the accuracy was at the margin of 95% agreement with the gold standard.
Future directions: Remaining goals may be achieved by using more advanced IMUs and microcontrollers, incorporating load cells for impact loading data, and Bluetooth transmission to eliminate wiring, thus expanding the use to grappling styles of martial arts such as Jiu-jitsu, Judo, and wrestling.
University of Wisconsin–Madison
Since 1999, the BME program at the University of Wisconsin (UW-BME Design) has had seven course curriculum where students starting in their first year.20,21 Student teams work to solve real-world biomedical problems with only their spring sophomore year being a semester in which the whole class works to solve the same problem while building technical and professional skills along the way.22 Over their 4 years, students are able to seamlessly continue projects from one semester to the next, resulting in the ability for design iteration and project completion. Senior teams always work on the same problem for the entire year with the goal of patenting and/or publishing their work. Project ideas for these courses are solicited from UW-Health professions on campus, industry, BME faculty and affiliates, as well as the community.23 Additionally, UW-BME Design collaborates with other programs in the college of engineering (e.g., mechanical engineering) forming cross-disciplinary design teams when needed. The general structure of UW-BME Design mirrors UD-BME, where teams have a design build test model with weekly meetings and a product design specification (PDS) that forms a contract-like agreement between the team and the client. Teams develop design ideas, presenting them to their classmates, faculty, and their client, and submit a preliminary design report. Prototypes are developed and shared with classmates in a Show and Tell session to gather feedback.24 At the end of each semester, teams present their work in a public poster presentation and submit their final report with a detailed design notebook.25
In the last 3 years, over 650 students have worked on 150 unique projects with over 65 projects running in a given semester (sophomore level and higher).23 Our collaboration with UW-Orthopedics and Rehabilitation began in 2010 and has spanned 55 projects with 19 different clients. Over the past almost 25 years, these projects have resulted in a significant number of publications, news stories, patents, company formation, and licensing, as well as open-source solutions to biomedical problems. Below are two examples of UW-BME Design projects in collaboration with UW-Orthopedics and Rehabilitation.
Project 3: Development of Distal Radius Reduction Model with Simulated Fluoroscopy, sponsored by Dr. James Stokman
Background: Distal radius fracture (DRF) reduction is one of the most common procedures performed by orthopaedic surgeons.26–29 Traditionally, a physician’s reduction technique is acquired through trial-and-error and observation of senior practitioners. Development of a simulator that can reliably teach surgical residents how to reduce and cast a DRF could greatly improve residents’ competency and patient outcomes. Currently, there are several life-like DRF models on the market.30–33 If accessible, fluoroscopy can be used to evaluate reduction alignment after casting is complete.31 While the Sawbones® model has been well-received by the orthopaedic community in terms of its validity,30,34 current evaluation of the training procedure is subjective,35 and there is growing interest for objective testing the orthopaedic trainees’ competency of hands-on skills.36,37
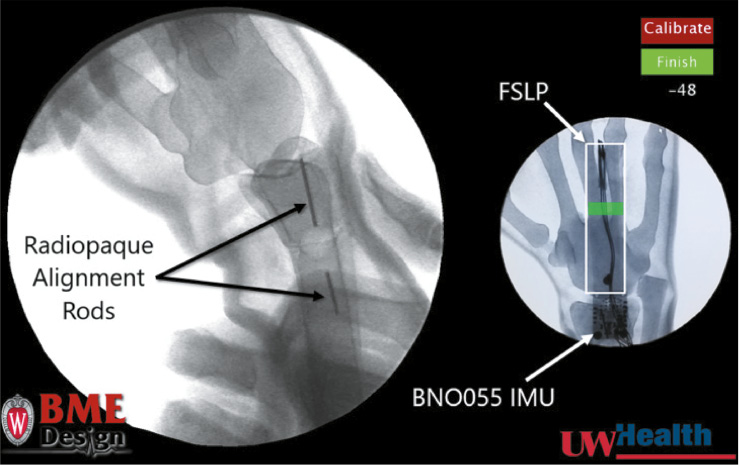
Project description and outcome: The design team developed a modified Sawbones DRF trainer that provides quantitative, real-time feedback to the trainee about their reduction quality in hopes of improving their casting proficiency. Feedback was incorporated in this via the use of live simulated fluoroscopy in conjunction with a force sensor and IMUs to capture relevant data, such as force applied and bone realignment angle (Figure 5). During use, a custom GUI displays a responsive x-ray video to simulate the reduction of the fracture based on the angle using images captured previously with fluoroscopy (Figure 6). A dynamic force indicator shows whether a participant is applying proper force to an acceptable location as determined by expert physician data (Video 3). Upon completion of casting, force and angle data pertaining to bone realignment can be graphed as a function of time to show the user how their technique varied throughout the procedure. Analysis of the collected casting data provides an objective measurement of trainee competency. Video 3 showcases an initial version of the GUI in use while the distal radius fracture model arm is being reduced. The fluoroscopic view updates in real-time and shows the view corresponding to the angle between the two radiopaque alignment rods as calculated by the orientation sensor. The angle is shown as a continually updating value on the left side of the interface, and an early implementation of force tracking is shown by the stacking bars on the right. The student team presented and tested the device twice at the International Pediatric Orthopaedic Symposium (IPOS®). In another instance, the students were funded to visit and market the device to executives and engineers at Sawbones, whose DRF model was the foundation of the prototype.
Figure 5. Distal radius fracture model arm and exterior processing and computing hardware in use during a trial reduction and casting experiment.
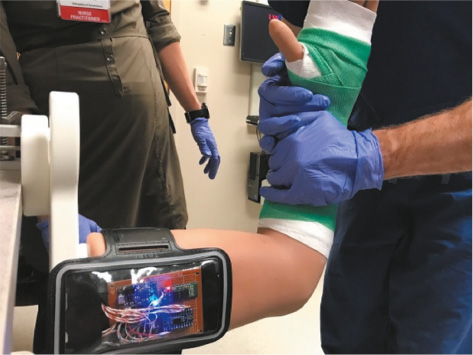
Figure 6. Graphical user interface (GUI) of the distal radius fracture model. Left panel depicts the previously captured simulated fluoroscopy that updates the fluoroscopic view as the reduction occurs in real time. Radiopaque alignment rods come pre-installed on each Sawbones model to qualitatively guide reduction efficacy. Right panel depicts internal hardware location within the arm—the Force Sensitive Linear Potentiometer (FSLP) and an absolute orientation sensor to track reduction angle (BNUO055 IMU)—as well as the clinician force localization along the FLSP and the magnitude of force applied via a continually updating heatmap bar. “Calibrate” button is used to zero the FLSP and orientation sensor prior to casting. “Finish” button is used to close the casting trial, export FLSP and orientation sensor data to a spreadsheet, and return to GUI main menu where another trial can be initiated.
Project 4: Rapid Liquid 3D Printing of Patient-Specific Wrist Orthoses, sponsored by Dr. Zachary French and Dr. Eamon Bernardoni
Background: After upper extremity injury or surgery, there is often a need for a custom orthosis created by hand therapists who have extensive training using moldable materials. With recent advances in 3D scanning and printing technology, there is potential to make customized wrist orthoses from a scan of the patient’s arm faster than what has been previously possible through manual molding. The known challenges of 3D printing of orthoses include costs, the know-how of managing the hardware and software, and the waiting time required for final production.38 The purpose of this project was to develop a system by which an orthopaedic surgery clinic can quickly fabricate patient-specific splints using a new 3D printing technology known as Rapid Liquid Printing (RLP). Rapid Liquid Printing has the capacity to dramatically increase the speed with which medium- and large-sized items are printed.39,40 RLP deposits the printed material into a support medium where it is cured and then removed, a faster and more easily scalable process than traditional 3D printing methods. Upper-extremity orthosis are a natural area for integration of this technology given that production time remains the greatest detriment to 3D printing customized orthoses in a clinical setting.
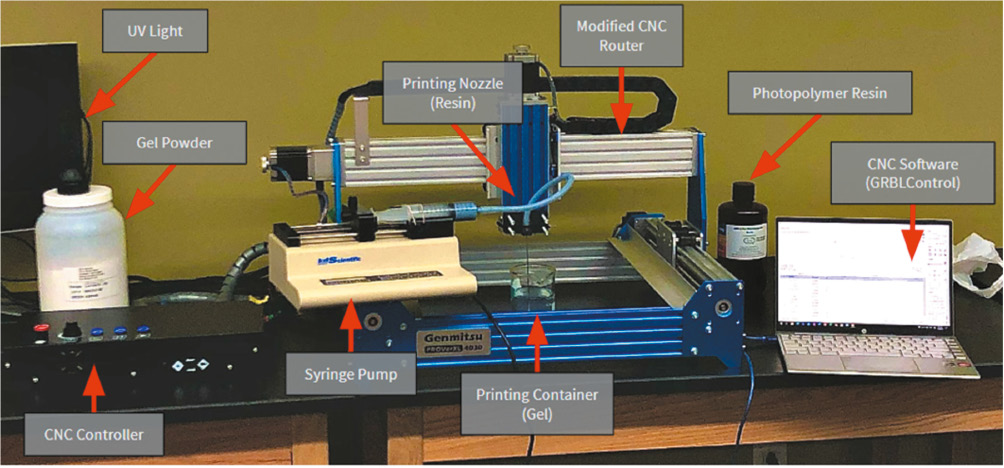
Project description and outcome: The students were tasked with designing and creating a new type of 3D printer that could utilize RLP to quickly print customized, removable wrist orthoses from a scan of the patient’s wrist in less than 1 hour to imitate a single clinic visit. The materials used should be skin safe, comfortable, rigid, and durable enough to provide support for the healing wrist. No commercially available printers exist that can print via RLP, so the students creatively chose to retrofit a CNC router for the purpose. The CNC cutting apparatus was removed and a 3D print head was designed by the students (Figure 7). The print material is extruded from a nozzle and suspended in a particular media that is quite viscous. Through optimization of material properties, concentrations, print speed, and extrusion rate, the ideal parameters were chosen for printing. Video 4 includes the print mechanism: Real-time video of the rapid liquid printing process. Future directions for the project include the creation of the software portion of the project, which will automatically apply a printable 3D model to a patient’s 3D surface-scanned upper extremity. Then, of course, printing a wrist orthotic.
Figure 7. The Rapid Liquid 3D printer setup.
Funding and Intellectual Property
The design courses are part of the undergraduate curriculum in college. However, to execute a design project, the team needs funding to support the materials, administrative costs, and the time-effort of the students and the advisors. Moreover, extramural investment may be instrumental if the final product is going to benefit the sponsor, either commercially or not.
Handling intellectual property (IP) can be daunting. Only a number of clinicians are familiar with the issue, while engineers who work with the industry may have a more in-depth understanding. In general, when working with an academic institution, there are certain rules already set in place. There may be room for negotiation, which should be settled before commencing the project.
At the University of Delaware, both industry and clinical sponsors submit a project proposal 3 months before the start of the senior design. In most cases, the sponsors contribute a sponsorship amount to be paired with a senior design team and sponsors can also have non-disclosure agreements (NDAs) in place with the senior design team. The sponsorship amount helps with senior design logistics, public-facing community events related to senior design, and to ensure that senior design teams have continued access to all materials and equipment in the design studio needed for low-level prototyping, including 3D printing, machining, basic raw materials, electronic and programming equipment, as well as material testing and sensing equipment used for verification and validation. This is usually feasible and the preferred option for partners in industry as well as most clinical sponsors. However, funding for sponsorship can sometimes pose a challenge to healthcare partners in the community, where the foremost mission of such institutions is healthcare delivery and not necessary R&D investments. If federal funding or any other type of support from the university is involved, for example, through the Institute of Engineering Driven Health (EDH),41 the clinical sponsor or the entity that the clinical sponsor is affiliated with establishes contracts defining the exact nature of collaboration with the University, with the assistance of Office of Economic Innovation and Partnerships (OEIP).42 These partnerships are established upfront, before the start of senior design, to avoid potential process-related delays. These senior design partnerships have resulted in patents (typically one a year for BME) as well as spin-offs and spin-ins at the University of Delaware.43 For either sponsor (industry or clinical), all material expenses for high-level prototyping are typically funded by the sponsors (clients).
At the University of Wisconsin–Madison, projects are also funded by the clients (sponsors). The department provides student access to its own teaching labs and equipment as needed. A project budget, typically at least $100, is requested at the time of project submission which is reviewed along with the project description prior to posting the project for student selection. Clients fund their projects out of pocket, use department discretionary funds, or grant funding. Regardless of which kind of funding source was used, all IP-related proceedings or issues need to be reported to the Wisconsin Alumni Research Foundation (WARF)44 per university policy and federal statutes. If WARF determines that they wish to pursue patenting, they will initiate an equity review to determine the source of funding. If federal funds were commingled in the pursuit of the invention, the inventors must utilize WARF in the patenting process; however, if they were not used, then the inventors can decide to pursue patenting on their own (which is rare due to the cost associated with filing and protecting a patent). WARF is a valuable resource for the University, supporting both BME and the School of Medicine and Public Health, giving 20% of the gross royalty income back to the inventors, 15% back to the department, and the rest is used to cover expenses and fund research, development, and accelerate startups for their patent portfolio. Approximately 30% of the BME Design projects go to WARF (10-20 projects annually), resulting in a few patents per year. Several companies have also been formed as a result of the UW-BME Design program.45
Most orthopaedic surgeons join the effort of engineering designs with one single motivation: to improve patient care and to make the lives easier for both the patients and the surgeons. It is worth noting that when a product really works, it typically carries potential commercial value. While most of the hard work is done by the engineering team, the clinical perspective from the surgeons is equally valuable. Healthcare institutions may have a designated office that processes IP-related tasks. This can be a valuable resource for surgeons under hire. On top of the agreement between the BME program and the surgeon or the hospital, the surgeon’s employment contract under the healthcare institution may be defined to determine IP, especially for full-time employees. Such a contract may allow the surgeon to claim part or all of the IP if the IP-related work was done outside of the working hours that are paid by the employer. The employer may also claim 100% of the IP generated by full-time employees regardless of how the work is done. As exhausting as this may seem, understanding the money and IP issues and handling appropriate negotiation and arrangement proactively may be the best course to pursue these fruitful collaborations.
Education, Immersion, and Future Leaders
Students can be highly motivated to partner with a clinician for a variety of reasons. This type of clinician-sponsored project provides an opportunity for the engineering students to incorporate theory and practice. Design courses are unique in that they bridge the transition from students to professionals when compared to regular college courses, perhaps even culminating future career trajectory and job offers in the biomedical fields. Of note, some of the bioengineering students are interested in pursuing a career in medicine. In addition to senior design collaborations, clinical immersion opportunities also help connect students with clinical mentors, help them understand what medicine is like, and understand how engineering can impact true patient care. Programs such as the winter term clinical immersion program between the University of Delaware and Nemours Children’s Hospital, give students the opportunity to work with clinical staff and learn about medicine through shadowing opportunities in both the clinic and the operating room.
The mentoring of these BME students has also been fulfilling for the surgeons. The surgeons educate the students on clinical pathology and the whys and hows of what needs to be done to help the patient. In return, the students often share insights distinct from those from medical student, residents, or clinical fellows. As engineers, their approach to a scenario is quite creative yet methodical, which complements well with the art and science of medicine. Throughout this mutual process, we may be nurturing clinician-scientists or clinical bioengineers who may bring a paradigm shift in our field in the future.
Time management can be challenging for the orthopaedic surgeons. The time and energy investment from the surgeon’s side depends on several factors: the nature of the project, the need of in-person visits (such as to examine or test clinical equipment), the expectation from the students, and obviously, what the surgeons see their role to be—that is, if the surgeon wants to be involved merely as a project sponsor or also a true mentor to the team. From the students’ perspective, working with doctors creates more motivation because it feels less like a school project and more like a tangible advancement that is applicable to the real world, in addition to fulfilling the requirement of completing the project and thus finishing the design course successfully.
Theoretically, this whole BME design process can be done with just adequate input from the surgeon, as there is an engineering faculty advisor in place to help the students. However, it would be fair to say that it can mean a lot to the students and the faculty advisor if the surgeon is willing to be “part of the team.” Particularly, in the post-COVID era, being able to join the design process in person for a few times may drastically boost the team morale. This involves strategic arrangement of administrative time versus clinical duties. While protected academic time is rare nowadays, these highly educational activities improve patient care as well as introduce intangible benefit to the surgeon’s institution in the long run. We educate orthopaedic residents and medical students to mold future healthcare leaders. The time and effort spent on collaborating with BME students can be equally fruitful in advancing healthcare and making a true difference in our field.
Acknowledgements
UD-BME Design would like to thank members of the two teams represented in this paper: Brendan Cohen, Zach Hill, Suzannah Hoguet, Maddie Lennon, Gavin McMahon, Stephen Mondoro, Catherine Peluso, Michael Trainor, and Nicholas Wickersham, as well as our numerous clinical partners, faculty, and administrators who have supported us over the years to deliver a wonderful and symbiotic experience for biomedical engineering students and healthcare professionals.
UW-BME Design would like to thank the two teams represented in this paper: Team Casting force: Mensah Amuzu, Andrew Baldys, Keshav Garg, Trace Jocewicz III, Marshall Schlick and client: Dr. James Stokman; and Team RLP: Jacob Arlandson, Benjamin Armstrong, Cate Fitzgerald, Kenzie Germanson, George Halunen, Lance Johnson, Julia Mastej, Emma Neumann, Warunyoo Nijjarungul, Gabrielle Snyder and clients Dr. Zachary French and Dr. Eamon Bernardoni; as well as, all of the orthopaedic physicians that have served as clients in the past, present, and future and the design faculty that provide mentorship to the student teams.
Project 2, sponsored by Dr. Alvin Su, supported by a POSNA Micro Grant.
Disclaimer
The authors have no conflicts of interest to report related to this manuscript.
References
- Merriam Webster Dictionary. Biomedical Engineering. Available at: https://www.merriam-webster.com/dictionary/biomedical%20engineering. Accessed March 23, 2023.
- Linsenmeier RA, Saterbak A. Fifty years of biomedical engineering undergraduate education. Ann Biomed Eng. 2020;48(6):1590-1615.
- ABET. Accredited Engineering Programs. Available at: https://www.abet.org/. Accessed March 20, 2023.
- Engineers Canada. Accredited Engineering Programs in Canada. Available at: https://engineerscanada.ca/accreditation/accredited-programs. Accessed March 20, 2023.
- Kotche M, Felder AE, Wilkens K, et al. Perspectives on bioengineering clinical immersion: history, innovation, and impact. Ann Biomed Eng. 2020;48(9):2301-2309.
- University of Delaware. Capstone Design Program. Available at: https://engr.udel.edu/undergraduate-education/senior-design/. Accessed March 20, 2023.
- Facts about Upper and Lower Limb Reduction Defects. Centers for Disease Control and Prevention. Available at: https://www.cdc.gov/ncbddd/birthdefects/ul-limbreductiondefects.html. Accessed September 8, 2022.
- James MA. Unilateral upper extremity transverse deficiencies: prosthetic use and function. J Pediatr Orthop. 2010;30(Supplement 2):S40-S44.
- Sheffler LC, Hanley C, Bagley A, et al. Comparison of self-reports and parent proxy-reports of function and quality of life of children with below-the-elbow deficiency. J Bone Jt Surg-Am Vol. 2009;91(12):2852-2859.
- James MA, Bagley AM, Brasington K, et al. Impact of prostheses on function and quality of life for children with unilateral congenital below-the-elbow deficiency. J Bone Jt Surg. 2006;88(11):2356-2365.
- Shoghi A, Bagley A, Wagner LV, et al. Patient-reported outcomes for children with unilateral congenital below elbow deficiency. J Pediatr Orthop. 2022;42(9):e949-e953.
- Adaptive Strider Program. Strider Bikes. Available at: https://striderbikes.com/adaptive/. Accessed March 20, 2023.
- Demorest RA, Koutures C, COUNCIL ON SPORTS MEDICINE AND FITNESS. Youth Participation and injury risk in martial arts. Pediatrics. 2016;138(6):e20163022.
- Tulendiyeva A, Saliev T, Andassova Z, et al. Historical overview of injury prevention in traditional martial arts. Sport Sci Health. 2021;17(4):837-848.
- Vacca L, Rosso V, Gastaldi L. Risk assessment in different Judo techniques for children and adolescent athletes. Proc Inst Mech Eng H. 2020;234(7):686-696.
- Chafetz RS, Warshauer S, Ulman S, et al. Inter & intra tester reliability of motion capture of six sports task used for return-to-sport testing. Orthop J Sports Med. 2022;10(5_suppl2):2325967121S0044.
- Gavagan CJ, Sayers MGL. A biomechanical analysis of the roundhouse kicking technique of expert practitioners: a comparison between the martial arts disciplines of Muay Thai, Karate, and Taekwondo. Carlson ME, ed. PLoS One. 2017;12(8):e0182645.
- Koshida S, Ishii T, Matsuda T, et al. Kinematics of judo breakfall for osoto-gari: considerations for head injury prevention. J Sports Sci. 2017;35(11):1059-1065.
- Kharitonova Y. Wii-Trieve: Retrieving Motion Sequences Using Acceleration Data of the Wii Controllers. Hilo: University of Hawaii.
- Tompkins WJ, Beebe D, Gimm JA, et al. A design backbone for the biomedical engineering curriculum. In: Proceedings of the Second Joint 24th Annual Conference and the Annual Fall Meeting of the Biomedical Engineering Society] [Engineering in Medicine and Biology. IEEE; 2002:2595-2596.
- Tompkins W. Implementing design throughout the curriculum. In: Proc. Annual Conference of the Biomedical Engineering Society; 2006.
- Wille C, Hess D, Levin J, Nimunkar A, Puccinelli J. Impact of a Sophomore BME Design Fundamentals Course on Student Outcome Performance and Professional Development. In: 2017 ASEE Annual Conference & Exposition Proceedings. ASEE Conferences; 2017:28457.
- Puccinelli J. University of Wisconsin-Madison. Biomedical Engineering Design Projects. Available at: https://bmedesign.engr.wisc.edu/. Accessed March 20, 2023.
- Alcock R, Puccinelli J. Benefits of a low-stakes Show and Tell session in BME Design. In: ASEE Annual Conference & Exposition Proceedings. ASEE Conferences; 2023.
- Puccinelli J, Nimunkar A. An Experience with Electronic Laboratory Notebooks in Real-World, Client-Based BME Design Courses. In: 2014 ASEE Annual Conference & Exposition Proceedings. ASEE Conferences; 2014:24.156.1-24.156.9.
- Court-Brown CM, Heckman JD, McQueen MM, et al. eds. Rockwood and Green’s Fractures in Adults. 8th ed. Lippincott Williams & Wilkins/Wolters Kluwer Health; 2015.
- Handoll HH, Elliott J, Iheozor-Ejiofor Z, et al. Interventions for treating wrist fractures in children. Cochrane Bone, Joint and Muscle Trauma Group, ed. Cochrane Database Syst Rev. 2018;2018(12).
- Elmi A, Tabrizi A, Rouhani A, et al. Treatment of neglected malunion of the distal radius: a cases series study. Med J Islam Repub Iran. 2014;28:7.
- Prommersberger KJ, Froehner SC, Schmitt RR, et al. Rotational deformity in malunited fractures of the distal radius. J Hand Surg. 2004;29(1):110-115.
- Egan C, Egan R, Curran P, et al. Development of a model for teaching manipulation of a distal radial fracture. J Bone Joint Surg Am. 2013;95(5):433-438.
- Seeley MA, Fabricant PD, Lawrence JTR. Teaching the basics: development and validation of a distal radius reduction and casting model. Clin Orthop. 2017;475(9):2298-2305.
- Colles Fracture Reduction and Casting Technique Trainer. Sawbones. Available at: https://www.sawbones.com/chop-colles-fracture-reduction-and-casting-technique-trainer-arm-left-soft-tissue-with-bones.html. Accessed March 20, 2023.
- Fracture Education | Management Principles. The Royal Children’s Hospital Melbourne. Available at: https://www.rch.org.au/fracture-education/management_principles/Management_Principles/. Accessed March 20, 2023.
- Ho K, Chimutengwende-Gordon M, Hardy JRW. A simple model to demonstrate the method of reduction and immobilization of forearm fracture in an adult or child. Ann R Coll Surg Engl. 2006;88(2):224-225.
- Boyd AS, Benjamin HJ, Asplund C. Principles of casting and splinting. Am Fam Physician. 2009;79(1):16-22.
- Angelo RL, Ryu RKN, Pedowitz RA, et al. A proficiency-based progression training curriculum coupled with a model simulator results in the acquisition of a superior arthroscopic bankart skill set. Arthroscopy. 2015;31(10):1854-1871.
- Cannon WD, Garrett WE, Hunter RE, et al. Improving residency training in arthroscopic knee surgery with use of a virtual-reality simulator. A randomized blinded study. J Bone Joint Surg Am. 2014;96(21):1798-1806.
- Li J, Tanaka H. Feasibility study applying a parametric model as the design generator for 3D–printed orthosis for fracture immobilization. 3D Print Med. 2018;4(1):1.
- Hajash K, Sparrman B, Guberan C, et al. Large-scale rapid liquid printing. 3D Print Addit Manuf. 2017;4(3):123-132.
- Zhao J, He N. A minireview of embedded 3D printing: supporting media and strategies. J Mater Chem B. 2020;8(46):10474-10486.
- University of Deleware. Institute of Engineering Driven Health. Available at: https://edh.udel.edu/. Accessed March 20, 2023.
- University of Deleware. Office of Economic Innovation and Partnerships. Available at: https://www.oeip.udel.edu/. Accessed March 20, 2023.
- University of Deleware. Office of Economic Innovation and Partnerships | Special Programs. Available at: https://www.oeip.udel.edu/special-programs/. Accessed March 20, 2023.
- Wisconsin Alumni Research Foundation. WARF. Available at: https://www.warf.org/. Accessed March 20, 2023.
- Puccinelli J. University of Wisconsin-Madison. Biomedical Engineering Design Projects | News. Available at: https://bmedesign.engr.wisc.edu/projects/news. Accessed March 20, 2023.
