Current Concept Review
Best Practices for Gender-Affirming Care for Pediatric Orthopaedic Patients
1Scottish Rite for Children, Department of Developmental and Behavioral Pediatrics, Dallas, TX; 2Scottish Rite for Children, Department of Pediatric Orthopedics, Dallas, TX; 3Scottish Rite for Children, Department of Psychology, Dallas, TX
Correspondence: Megan Johnson, MD, Scottish Rite for Children, 2222 Welborn St., Dallas, TX 7529. E-mail: [email protected]
Received: March 3, 2023; Accepted: March 6, 2023; Published: May 1, 2023
Volume 5, Number 2, May 2023
Abstract
Transgender and gender-expansive youth may experience barriers to healthcare due to stress and anxiety associated with accessing healthcare coupled with a lack of awareness by providers of best practices for treating this population. The pediatric orthopaedic community has an opportunity to improve relationships and outcomes for transgender patients by understanding the distinctive qualities of this population and how to best support these patients via the provision of gender-affirming care. By following best practices for gender-affirming care, pediatric orthopaedic providers are uniquely positioned to provide affirming, supportive care for transgender patients within their practices, which may ultimately impact patient outcomes and patient satisfaction. Gender-affirming care should begin the moment the patient enters the healthcare facility, continue through all perioperative and follow-up care, and should be practiced by all members of a multidisciplinary care team. Synergizing the expertise of psychologists, developmental and behavioral pediatricians, and orthopaedic surgeons, this article offers best practices at each step in the care pathway for providers to consider. An interview with a pediatric patient with gender considerations who has previously undergone orthopaedic surgery is included at the end of this article to provide additional insight from the patient perspective.
Key Concepts
- Transgender and gender-expansive youth may experience barriers to accessing orthopaedic care.
- Orthopaedic providers should educate themselves on treatment considerations for this population in order to promote access to care in general and affirming care specifically.
- Transgender and gender-expansive pediatric patients require specific education on pre- and post-surgical topics, such as foley catheter placement and removal, and chest binding, packing, or tucking.
- Pediatric orthopaedic providers should be aware of how a patient’s current or planned hormonal and/or surgical gender-affirming intervention(s) may intersect with their orthopaedic needs.
Introduction
The term transgender describes a person whose gender identity is incongruent with their sex assigned at birth. Gender-expansive refers to a person who expresses traits that do not typically fit within the gender binary or with that of their sex assigned at birth. While estimates vary, recent surveys suggest over 1.6 million adults (age 18 and older) and approximately 300,000 youth (ages 13-17) identify as transgender in the United States.1 Transgender patients may experience barriers to healthcare for a variety of reasons, including stress associated with accessing healthcare2 as well as lack of awareness by providers regarding best practices for this population.3 From the first contact at check-in, through the navigation of clinical and surgical environments, the patient-centered orthopaedic care of a transgender person requires recognition of the unique characteristics of this population.
Transgender and gender-expansive youth are at significant risk for experiencing various psychological symptoms, with gender dysphoria as a commonly cited concern. Gender dysphoria refers to the sense of discomfort that results from a person’s gender identity not matching their physical body or sex assigned at birth, resulting in clinically significant distress or impairment, and lasts for at least 6 months.4 Additionally, transgender youth are at greater risk relative to their cisgender peers for experiencing general psychological distress, major depression, self-harm, and suicidal ideation, with large documented effect sizes.5–8 The theoretical basis commonly used to explain these differences is grounded in the Minority Stress Model, which posits that we live in a heteronormative, gender-normative culture.7 Individuals who exist outside of cisgender and heteronormative expectations often experience chronic stress, via ongoing experiences of stigmatization and discrimination at individual, familial, community, and national levels.7 In support of this theory, both transgender males and transgender females report extremely high rates of discrimination due to their gender identity (92% and 79%, respectively); transgender males (37%) and females (33%) also report high rates of being physically threatened or harmed due to their gender identity.5
Healthcare discrimination, reported in approximately one-quarter of transgender individuals, results in increased risk of physical and emotional symptoms and risk of postponing necessary care.9 Notably, young people with neurodevelopmental differences, particularly autism, have documented increased frequency of gender variance and psychiatric conditions.10 This is important for orthopaedic providers as youth with neurodevelopmental differences also frequently have associated musculoskeletal disorders for which surgery may be indicated.
The pediatric orthopaedic community has an opportunity to improve relationships and outcomes with transgender and gender-expansive patients by better understanding the specific characteristics of this population as well as how to best support these patients through clinical and perioperative encounters. This starts with gender-affirming language as most transgender youth want their preferred name and pronouns documented widely across the electronic medical record,11 and the use of gender-affirming language is associated with improved mental health outcomes.12 Other medically important considerations include the impact of hormone replacement therapies on bone health and perioperative cardiac and venous thromboembolism risk,13 the anatomic changes accompanying prior gender-affirming surgery, and the high rates of violence and risk of traumatic injuries for transgender people.14 Importantly, it requires a multidisciplinary team to appropriately provide “whole-person” care that incorporates a patient’s physical, mental, and emotional health needs. As such, this paper provides multidisciplinary best practices on the treatment of transgender children and adolescents from the perspective of a fellowship-trained behavioral and developmental pediatrician, pediatric orthopaedic surgeons, and pediatric psychologists.
Gender Identity Terminology Glossary
Appropriate use of terminology and language surrounding gender identity is crucial to creating a supportive experience for transgender patients (Table 1).15,16 All providers should be fluent in this terminology while also recognizing that language is fluid and preferred terms may change over time.
Table 1. Gender Identity Terminology
| Term | Definition |
|---|---|
| Gender Identity | A person’s internal understanding of their gender |
| Gender Expression | The way a person outwardly presents their gender to others |
| Transgender | A person whose gender identity differs from their sex assigned at birth |
| Cisgender | A person with a gender identity that is congruent with their sex assigned at birth |
| Nonbinary | An umbrella term for a person whose gender identity is not exclusively male or female but may exist on a spectrum |
| Gender Expansive, Fluid | A person who expresses traits that do not typically fit within the gender binary or with that of their sex assigned at birth |
| Transgender Male, Affirmed Male | A person who was assigned female at birth but identifies as male |
| Transgender Female, Affirmed Female | A person who was assigned male at birth but identifies as female |
Best Practices for Gender-Affirming Care
Please see Appendix 1 for a checklist that can be adapted across institutions to ensure the delivery of high-quality gender-affirming care to transgender and gender-expansive patients. This checklist provides general guidance and by no means is exhaustive. The approach to care for transgender patients must be tailored to individual cases and should be performed by a team that is committed to ongoing training and education on the latest mental health, medical, and surgical evidence.
Physical Environment
All staff members should undergo training to work with Lesbian Gay Transgender Queer Questioning Intersex Asexual Plus (LGTBQIA+) patients. This training should be provided on a regular and ongoing basis. Identify your hospital and clinic providers’ support of LGTBQIA+ patients and families by creating a welcoming, equitable, and inclusive space.17,18 This includes visible signage throughout the hospital and clinic rooms that affirms patients of all genders and sexual orientations are safe and welcome.17,18 Photography and art pieces posted throughout the hospital should be inclusive in nature (depicting nonheteronormative families), and non-gendered bathroom space (e.g., all gender, single occupancy restrooms) should be available and easily accessible.17,18 Additionally, providers may choose to wear lanyards, pins, or badge clips to nonverbally communicate an affirming and supportive environment for LGBTQIA+ patients and their families.
Patient Identification and Documentation
Throughout the hospital stay, from preoperative clinic visits to follow-up care, providers should ask a patient for their name and pronouns and also consider introducing themselves using their preferred pronouns as a means to present a welcoming environment.17–21 With patient permission, consistent use of a patient’s stated name and pronouns is indicated by the staff in all interactions, even if the patient’s parents or caregivers use a different name or pronouns when referring to the patient.17–21 Furthermore, it is important to recognize that a patient’s stated name and pronouns may change, as gender and sexual orientation are fluid constructs that develop and may even fluctuate over time.20 As such, patients should be provided with consistent and routine opportunities to update this information for the medical team as desired.17,18
Concerning documentation, ask permission to use the patient’s stated name and pronouns in the medical chart. If permission has been received, ensure consistent use of a patient’s stated name and pronouns throughout all documentation in the electronic medical record.17–21 Ideally, a patient’s stated name should be the primary name that appears in the demographics section of their chart.20,21 The patient’s stated gender (e.g., cis-female, nonbinary, transgender female-to-male) should also be visible and their pronouns delineated17–20 (Figure 1). It should be the expectation that all members of a patient’s care team will utilize the patient’s stated name and pronouns throughout all clinical consultations as well as written communication and charting.17–21
Figure 1. Gender documentation within the electronic medical record. A. Example of gender identity as it appears on the front page of a patient’s electronic medical record. B. Example of a gender identity smart form that can be filled out for any patient to ensure the medical team is aware of gender identity, preferred pronouns, and gender-affirming treatments.

Multidisciplinary Team Approach
Given that transgender children and youth with orthopaedic conditions may present with numerous non-orthopaedic medical issues, research supports the role of integrated multidisciplinary care, including psychological assessment and preparation of pediatric surgical patients. Such evaluations allow the medical team to learn more about the patient, including relevant familial factors, information on academic and social functioning, and identify the presence of any psychological symptoms. Pre-existing mood, anxiety, and/or trauma-related symptoms may put a patient at risk for a difficult postoperative course as patients may struggle with pain management or postoperative adherence. Given the disproportionately high rates of psychological symptoms experienced by LGTBQIA+ patients together with their increased exposure to acute and chronic stressors, victimization, and even trauma, assessing for these symptoms is strongly advised.18–21 Further, if the planned surgery is not emergent, surgery may be postponed until the patient is connected with local mental health resources and appropriately stabilized from the mental health perspective.
Preoperative psychological evaluations also allow for specific surgical considerations to be discussed with the patient. These discussions may include information regarding room preferences specific to gender; the potential for foley catheter placement; possible menstrual spotting; the use of binding, taping, packing, or tucking; as well as preparation for any medical media, which will all be discussed in further detail in the next section. Collaboration with Child Life specialists is especially beneficial when providing this education, given their expertise in medical play and targeted preparation and education in anticipation of interventions. Moreover, preoperative evaluations allow the psychosocial support team to develop sufficient rapport with the patient to act as a source of ongoing support and assist with liaising with the rest of the medical team if needed.
Perioperative Concerns
Room Preferences: If a patient’s surgery requires postoperative hospital admission, it is important to proactively speak with the patient about their room assignment preferences.18,21 Transgender patients should be offered the option of a private room, especially if the patient has concerns about their safety and/or comfort due to their gender identity or presentation.18,21 This should be presented as one of multiple options to ensure the patient does not feel ostracized or singled out.21 Transgender patients may feel more comfortable with care team members of a certain gender and should be asked about their preferences prior to admission.
Foley Catheter: If a patient requires a foley catheter, education should be provided preoperatively regarding catheter use. Specifically, patients should be educated on when and by whom the catheter will be placed as well as expectations regarding the duration of catheter use. For transgender patients, the presence of a foley catheter may induce feelings of gender dysphoria as it may draw attention to their sex assigned at birth. As such, a plan should be developed with the patient that indicates when the catheter will be removed and by whom. Additionally, a formal plan should also be developed for providing affirming mental health intervention in the event the patient begins to exhibit or report symptoms of gender dysphoria. Engagement in collaborative decision-making with the patient and family is particularly important surrounding this topic, as some patients may wish to remove the catheter themselves while being coached by a member of the medical team.
Menstrual Spotting: For those patients with uteruses, it is imperative that the potential for postoperative menstrual spotting is discussed. For transgender males, gender nonconforming and/or nonbinary patients, the experience of unexpected menstrual spotting may be alarming and potentially induce feelings of gender dysphoria. Patients should be prepared for this possibility, and a plan should be developed collaboratively between the patient and the medical team regarding how menstrual spotting and the potential for dysphoric feelings will be managed.
Gender Affirming Supports (Binding, Packing, Tucking): Some transgender and gender-expansive patients don gender-affirming supports, such as chest binders, prosthesis packing, and other adhesives or bandages to mask the presence of breast tissue or genitalia (Figure 2).17,18,20,21 It is important to discuss these topics preoperatively to determine (1) what anatomical or gender-affirming physical supports the patient typically uses, (2) if they have any history of skin breakdown or pulmonary challenges consistent with the anatomical supports they use, and (3) to create a plan for who will assist the patient in donning and doffing the gender affirming materials, and when the donning/doffing can safely occur.18,20,21 Some patients may wish to don and doff their gender-affirming supports themselves, while others may wish to have their surgeon or nurse doff and don the supports while they are under anesthesia. Consideration of how the patient’s gender-affirming supports may cover their surgical incision is also important, as it may relate to healing, risk for infection, and potential gender dysphoria.
Figure 2. Gender affirming supports. A. Transtape used to mask the presence of breast tissue or genitalia. B. Chest binder used to mask the presence of breast tissue.

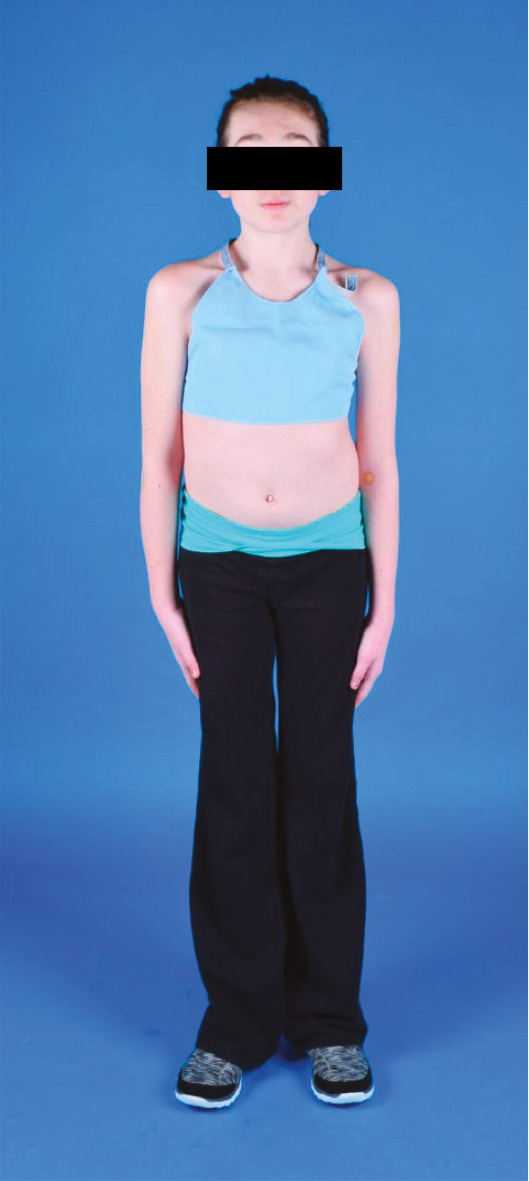
Clinical Media: Pediatric orthopaedic patients are sometimes asked to take clinical photos and videos for documentation purposes before and after surgery. For transgender, gender diverse, and intersex patients, this may be an uncomfortable experience and they should be provided with as much agency throughout the process as possible. For example, patients should be notified in advance when the medical team is requesting a clinical photo or video, and patients should have the ability to decline such a request. If they consent, patients should be provided with a choice of photographers of different genders if staffing allows. Patients should also be permitted to select who will accompany them to the media department (e.g., parent, caregiver, nurse, etc.). Furthermore, hospitals should be mindful of the garments that patients are expected to wear in photos and videos as many hospitals require cisgender female patients to don a “halter top” style garment for photos (Figure 3).
Figure 3. Example of “halter top” that some female patients are asked to don for clinical photos.
Similarly, patients that are transgender males may feel uncomfortable with a request to remove their shirt without being provided a garment to cover up with, especially if they have developed secondary sex characteristics.
Puberty Blocking Hormones, Gender Affirming Hormones, and Prior Gender Affirming Surgeries
Along with social affirmation (e.g., gender pronouns, clothing), transgender patients may also undergo medical and surgical interventions to support their gender identity. Puberty blockers are used during puberty and are reversible, hormone therapy (e.g., testosterone hormones for birth-assigned females and estrogen hormones for birth-assigned males) are used beginning in early adolescence and are partially reversible, and gender-affirming surgeries are typically used in adulthood and are not reversible (Rafferty et al. 2018).22 Some of these treatments have implications for patients undergoing orthopaedic surgery. As such, it is critical for all members of the care team to be aware of which treatments the patient is currently undergoing, has undergone, and/or has planned for the future.
Transgender patients may be taking Gonadotropin-Releasing Hormone agonists (GnRHa) for severe gender dysphoria symptoms or to suppress secondary sex characteristics.23 Affirmed females may be taking puberty blockers to allow utilization of lower doses of estradiol when the first stages of hormone affirmation begins.
In the context of orthopaedic surgery, GnRHa influences bone health. In a recent study, bone mineral density was noted to decrease during GnRHa treatment and to increase during gender-affirming hormone treatment, with recovery among affirmed boys but persistent reduction among affirmed females after 3 years of treatment with estradiol.24 When GNRHa are used in young people who are candidates for orthopaedic surgery, it is essential to include an endocrinologist in the multidisciplinary team to measure and monitor bone density and provide recommendations to reduce risks and optimize outcomes. Pertinent interventions may include mineral and vitamin supplementation along with weight-bearing exercise.25
Some young people who undergo puberty suppression (which is fully reversible and provides time for further evaluation within the context of a multidisciplinary team) will ultimately elect to also pursue gender-affirming therapy. Recommendations vary regarding the age at which gender-affirming hormone therapy should be started, with The Endocrine Society Guidelines noting that although it may be started before age 16, there is scarce literature pertaining to initiation prior to 13.5-14 years.23,26 The physical changes associated with these types of therapy are only partially reversible; thus, diligent family-centered mental health assessment regarding the readiness of the young person is crucial. With respect to young people planning orthopaedic surgery, those who are receiving gender-affirming treatment require preoperative assessment of cardiovascular and coagulation risks that may be increased secondary to hormone therapy.23
In the case of female-affirming hormonal treatment, estradiol is used and necessitates a close review of past medical and family history of hypercoagulability and clotting dysfunction. Should a positive history be identified, laboratory evaluation is indicated to delineate causes of hypercoagulability/clotting and/or a hematology evaluation, to be completed prior to beginning the therapy. Care teams must be aware of this clotting risk when orthopaedic surgery is being considered. Once deemed safe, low-dose estradiol is begun, with gradual increases over 3-6 months.23 In the case of female-affirmed individuals who are already in advanced puberty, puberty blockers are optional, with most providers using spironolactone or bicalutamide to decrease the action of testosterone. With respect to side effects that have medical and surgical implications, spironolactone increases urination and produces depressive symptoms in some individuals. In addition, hyperkalemia may occur, although uncommonly, and has been reported during the initial 6 months of treatment, with subsequent resolution irrespective of the dose being taken (Millington et al. 2019). Another agent administered by some clinicians, bicalutamide, acts as a potent androgen receptor blocker that also has the positive side effect of gynecomastia in this clinical context.23 However, it is potentially toxic to the liver; thus, liver function tests must be monitored frequently when it is prescribed.27
Moreover, gender reassignment and genital-affirming surgeries may be sought by individuals with the following considerations: well-documented persistent gender dysphoria who have reached the legal age of maturity; have responsibly and continuously used gender-affirming therapy for 12 months; have demonstrated successful, full-time living in their new gender role for 12 months; present with well-controlled medical and mental health issues; and exhibit knowledge of all practical aspects of the surgery, including costs, extent of hospitalization, side effects, and postsurgical rehabilitation.26 When a candidate for orthopaedic surgery has had prior gender-affirming surgery, central issues to explore include prior responses to anesthesia, previous surgical complications, course of recovery, and the psychological disposition to yet another surgery, which may change one’s physical appearance and function as well as carry risks.
Conclusion
Orthopaedic providers are more likely to see transgender and gender-expansive patients today and it is imperative that providers are well-informed regarding care considerations relevant to this patient population.28 The pediatric orthopaedic community can improve relationships and outcomes for transgender and gender-expansive patients by understanding and supporting gender-affirming care throughout the entire episode of care, from outpatient clinical encounters to inpatient surgical care and extending into recovery as applicable. The myriad considerations include appropriate and dignified use of language and definitions, optimizing the environment of care to reflect respect, safety, and compassion, and a thorough and up-to-date understanding of psychological, medical, and surgical dimensions that characterizes this population. Mental health, medical, and surgical risks must be carefully weighed and holistically addressed. This is best done within the framework of a multidisciplinary team that includes developmental-behavioral pediatricians, pediatric orthopaedic surgeons, and pediatric psychologists who are committed to thoughtfully implementing best practice guidelines as outlined in this paper.
Additional Links
Disclaimer
The authors report no conflicts of interest related to this manuscript.
References
- Herman JL, Flores AR, O’Neill KK. How many adults and youth identify as transgender in the United States? June 2022. Available at: https://williamsinstitute.law.ucla.edu/wp-content/uploads/Trans-Pop-Update-Jun-2022.pdf. Accessed December 19, 2022.
- Hatzenbuehler ML, Phelan JC, Link BG. Stigma as a fundamental cause of population health inequalities. AM J Public Health. 2013;103(5):813-821.
- Gonzales G, Henning-Smith C. Barriers to care among transgender and gender nonconforming adults. Milbank Q. 2017;95(4):726-748.
- American Psychiatric Association. DSM-5-TR Fact Sheets. Available at: https://www.psychiatry.org/psychiatrists/practice/dsm/educational-resources/dsm-5-tr-fact-sheets. Accessed February 26, 2023.
- Price-Feeney M, Green AE, Dorison S. Understanding the mental health of transgender and nonbinary youth. J Adolescent Health. 2020;66(6):684-690.
- Veale JF, Watson RJ, Peter T, et al. Mental health disparities among Canadian transgender youth. J Adolescent Health. 2017;60(1):44-49.
- Carmel TC, Erickson-Schroth L. Mental health and the transgender population. J Psychosoc Nurs Ment Health Serv. 2016;54(12):44-48.
- Connolly MD, Zervos MJ, Barone II CJ, et al. The mental health of transgender youth: advances in understanding. J Adolescent Health. 2016;59(5):489-495.
- Reisner SL, Hughto JM, Dunham EE, et al. Legal protections in public accommodations settings: a critical public health issue for transgender and gender-nonconforming people. Milbank Q. 2015;93(3):484-515.
- McPhate L, Williams K, Vance A, et al. Gender variance in children and adolescents with neurodevelopmental and psychiatric conditions from Australia. Arch Sex Behav. 2021;50:863-871.
- Sequeira GM, Kidd K, Coulter RW, et al. Affirming transgender youths’ names and pronouns in the electronic medical record. JAMA Pediatr. 2020;174(5):501-503.
- Russell ST, Pollitt AM, Li G, et al. Chosen name use is linked to reduced depressive symptoms, suicidal ideation, and suicidal behavior among transgender youth. J Adolescent Health. 2018;63(4):503-505.
- Gomes MP, Deitcher SR. Risk of venous thromboembolic disease associated with hormonal contraceptives and hormone replacement therapy: a clinical review. Arch Intern Med. 2004;164(18):1965-1976.
- Stotzer RL. Violence against transgender people: a review of United States data. Aggress Violent Beh. 2009;14(3):170-179.
- Baldwin A, Dodge B, Schick VR, et al. Transgender and genderqueer individuals’ experiences with health care providers: what’s working, what’s not, and where do we go from here? J Health Care Poor Underserved. 2018;29(4):1300-1318.
- Center for Disease Control and Prevention. Sexually Transmitted Infections Treatment Guidelines, 2021. Available at: https://www.cdc.gov/std/treatment-guidelines/trans.htm. Accessed: December 19, 2022.
- Lapinski J, Covas T, Perkins JM, et al. Best practices in transgender health: a clinician’s guide. Prim Care-Clin Off Pract. 2018;45(4):687-703.
- Tollinche LE, Van Rooyen C, Afonso A, et al. Considerations for transgender patients perioperatively. Anesthesiol Clin. 2020;38(2):311-326.
- Ramsey DC, Lawson MM, Stuart A, et al. Orthopaedic care of the transgender patient. J Bone Joint Surg Am. 2021;103(3):274-281.
- Roque RA. Transgender pediatric surgical patients—Important perioperative considerations. Pediatr Anesth. 2020;30(5):520-528.
- Tollinche LE, Walters CB, Radix A, et al. The perioperative care of the transgender patient. Anesth Analg. 2018;127(2):359.
- Rafferty J, Yogman M, Baum R, et al. Ensuring comprehensive care and support for transgender and gender-diverse children and adolescents. Pediatrics. 2018;142(4):e20182162.
- Diaz A, Figueredo V. Transgender in pediatrics: a narrative review. Pediatr Med. 2022. Available at: https://pm.amegroups.com/article/view/6803.
- Schagen SE, Wouters FM, Cohen-Kettenis PT, et al. Bone development in transgender adolescents treated with GnRH analogues and subsequent gender-affirming hormones. J Clin Endocr. 2020;105(12):e4252-e4263.
- Ciancia S, Dubois V, Cools M. Impact of gender affirming treatment on bone health in transgender and gender diverse youth. Endocr Connect. 2022;11:e220280.
- Hembree WC, Cohen-Kettenis PT, Gooren L, et al. Endocrine treatment of gender-dysphoric/gender-incongruent persons: an endocrine society clinical practice guideline. J Clin Endocr. 2017;102(11):3869-3903.
- Neyman A, Fuqua JS, Eugster EA. Bicalutamide as an androgen blocker with secondary effect of promoting feminization in male-to-female transgender adolescents. J Adolescent Health. 2019;64(4):544-546.
- Bustos VP, Bustos SS, Mascaro A, et al. Regret after gender-affirmation surgery: a systematic review and meta-analysis of prevalence. Plast Reconstructive Surgery-Glob Open. 2021;9(3):e3477.
Appendix
Gender-Affirming Care Checklist for Medical Care Teams
GENERAL CONSIDERATIONS
- Consider posting visible gender-affirming signage throughout clinic and inpatient spaces.
- Consider donning visible LGBTQIA+/pride pins, stickers, buttons, lanyards.
- Provide more inclusive intake questionnaires that ask about preferred name, gender identity and pronouns.
- Verbally ask/confirm with the patient the name they go by.
- Verbally ask/confirm with the patient how they identify re: gender.
- Verbally ask/confirm the patient’s pronouns.
- Query patient about whom this information may be shared with.
- Documentation in the chart should be consistent with patient preferences regarding their name, gender and pronouns.
- Ensure that each team member is being consistent regarding the patient’s preferred name, gender identity and pronouns (e.g., MAs, nurses, advanced practice providers, therapy services, mental health providers, etc.).
PRE-OPERATIVE CONSIDERATIONS
- Query use of current and planned gender-affirming supports.
- Physical exam
- Provide the patient with gender neutral exam attire.
- Query use of patient’s language regarding their body and use the terminology they provide.
- Explain what the physical exam will consist of and obtain patient’s consent before starting.
- Clinical Media
- Provide the patient with gender neutral media attire.
- Allow the patient to choose who is present in the room.
- Catheterization
- Educate patient regarding their need for a catheter.
- Develop a plan regarding catheter removal.
- Gender-Affirming Supports (binding, packing, tucking)
- Educate patient regarding when gender-affirming supports (e.g., binder) will be doffed and donned.
- Develop a plan regarding who will assist with these activities.
- Mental Health & Suicidality
- Consider evaluation by psychologist to assess for any mental health concerns, including risk for suicide.
- If patient endorses significant mental health symptoms, be prepared to provide targeted resources.
- Consider evaluation by psychologist to assess for any mental health concerns, including risk for suicide.
- Physical exam
- Provide patient with regular opportunities to affirm or update their gender information.
- Provide patient with support resources.
PERI-OPERATIVE CONSIDERATIONS
- Provide a handoff from the clinic team to the surgical and inpatient teams regarding patient’s name and pronouns, as well as documentation of preferences.
- Ensure that each team member is being consistent regarding the patient’s preferred name, gender identity and pronouns.
- Assess patient’s comfort in having a shared inpatient room (if necessary) and offer a private room (if available).
- Confirm and execute previously created plan regarding when/how patient will doff and don gender-affirming supports.
- Confirm and execute previously created plan regarding catheter removal.
POST-OPERATIVE CONSIDERATIONS
- Provide a handoff from the surgical team back to the clinic/outpatient team regarding patient’s name and pronouns, as well as documentation of preferences.
- Ensure that each team member is being consistent regarding the patient’s preferred name, gender identity and pronouns.
- Continue to assess patient’s use of current and future gender-affirming supports.
- Continue to assess patient’s mental health and suicidality.
- Continue to provide patient with regular opportunities to affirm or update their gender information.
- Continue to make support resources available and easily accessible.
