Invited Perspective
POGO Travel Journal: Pediatric Orthopaedic Service Trip to Portoviejo, Ecuador
1Department of Orthopedics and Sports Medicine, Nemours Children’s Health, Jacksonville, FL; 2Department of Orthopaedics and Rehabilitation, University of Mississippi Medical Center, Jackson, MS
Correspondence: Anna Rambo, MD, Department of Orthopedics and Sports Medicine, Nemours Children’s Health, 807 Children’s Way, Jacksonville, FL 32207. E-mail: [email protected]
Received: February 28, 2023; Accepted: March 6, 2023; Published: May 1, 2023
Volume 5, Number 2, May 2023
Location
Portoviejo, Ecuador, in the coastal region of Manabí.
Fundación La Vida is a clinic in Portoviejo which is supported by Bayside Medical Missions (BMM). BMM was started 40 years ago by Drs. Bob Eubanks and Paul Fellers, orthopaedic surgeons from Fairhope, AL, who began making yearly trips overseas to different countries. In 2000, BMM committed to long-term volunteerism in Ecuador and worked with the community in Portoviejo to establish a free-standing clinic with operating rooms. Dr. Fellers’ wife, Flor Fellers, RN, also committed to providing outreach to this area and was instrumental in helping establish a community connection and the construction of the clinic. The Fellers divide their time between Ecuador and Fairhope.
La Vida provides orthopaedic care for pediatric and adult patients. The clinic is equipped with an X-ray suite, exam rooms, two operating rooms, three sterilizers, two C-arms, and a postoperative area where patients can spend the night. The building, built to California earthquake standards, has even survived a 7.8 magnitude earthquake. There are annual orthopaedic sports, arthroplasty, foot and ankle, and hand brigades. Pediatric orthopaedics has a spring and fall brigade due to increased need (Figure 1).
Figure 1. A pediatric brigade stands outside La Vida Fundación Clinic, October 2022.

Local Accommodations
We stayed in the beach town of Crucita, a 40-minute van ride to the clinic. The Fellers graciously host volunteers in their house across the street from the beach. The house is in a gated neighborhood, but we all felt comfortable venturing out and exploring the main street of Crucita and the beach. The top deck of the house has hammocks, a bar, and a beautiful view of the Pacific Ocean and the city of Manta (Figure 2).
Figure 2. The view from the top deck of the Fellers’ house, where volunteers stay.

Local Health Concerns
Mosquito-borne illnesses such as Zika and malaria are a concern during the rainy season months, which are from December to April on the coast. However, in Crucita there are strong winds and mosquitoes are less of a concern. The clinic and house are air-conditioned as well. We went during the end of the dry, cool season in October, and temperatures ranged from 50-70 degrees Fahrenheit with a nice breeze and no mosquitoes. There was also no time change from Central Standard Time. The flu and COVID-19 vaccines are recommended but otherwise, we did not take malaria pills or get any additional vaccines. The CDC and WHO officially recommend hepatitis A & B, typhoid, yellow fever, rabies, meningitis, polio, MMR, Tdap, chickenpox, shingles, pneumonia, and influenza.
Crucita and the area around the clinic in Portoviejo are safe, but we recommend being vigilant and not wearing flashy jewelry or carrying a large amount of cash at one time. Also, do not drink the water unless it has been boiled or is bottled.
Important Materials to Bring
Sunscreen is needed, as the equator runs through Ecuador, and the sun can be very strong. Depending on the time of year, bring a light raincoat or jacket. Suggested medical equipment includes your gloves, preferred suture, and any implants you can get your local implant representative to donate. The currency is U.S. dollars, and credit card machines are not always available. An anti-diarrheal kit is always helpful. BMM recommends downloading WhatsApp onto your phone. The messaging app allows you to communicate with other team members and family back home.
Previous Travel History
Dr. Anna Rambo has traveled to Portoviejo to volunteer twice—once as a resident, before deciding to pursue pediatric orthopaedics, and recently in October 2022, as a newly trained pediatric orthopaedic surgeon. She is also a member of the BMM Board. Her mother is from the Manabí area, and her grandfather grew up in Portoviejo. She has traveled to Ecuador multiple times since a young age and feels very connected to this specific location.
Dr. Kellie Leitch has also been twice and has plans to return in September 2023.
Outreach Goals
- Provide high-quality care to children with orthopaedic problems in Ecuador.
- Provide education to the local team of surgeons, surgical techs, and clinical staff in the field of pediatric orthopaedics and surgical techniques.
- Provide a unique educational and cultural experience to residents from North America. It is important that our trainees have an understanding of the needs of individuals who don’t live in North America (Figure 3).
- Develop a culture of charity and generosity amongst the next generation of orthopaedic surgeons.
Figure 3. Chief residents Dr. Walters (far left) and Dr. Badon (far right) with Dr. Leitch (middle left) and Dr. Rambo (middle right).

Typical Clinical Cases
Most patients are from the coastal region of Manabí, but some travel very far from La Sierra or mountain region. La Vida has also treated patients from Peru and Columbia.
Typical clinical cases include:
- Children with neuromuscular orthopaedic issues, including hip dysplasia, upper and lower extremity spasticity, and associated contractures.
- Children with developmental dysplasia of the hip (DDH). The majority of DDH cases did not have infant screening and are older than patients typically seen in the United States (Figure 4).
- Children with deformity secondary to malunions and nonunions of fracture.
- Children with Blount’s disease.
- Children with deformities of the upper and lower extremities, including clubfoot (Figure 5).
Figure 4. Pre- and postoperative radiographs of a 3-year-old female with DDH, right femoral shortening osteotomy, acetabuloplasty, and open hip reduction. Implants: Two one-third tubular plates stacked.
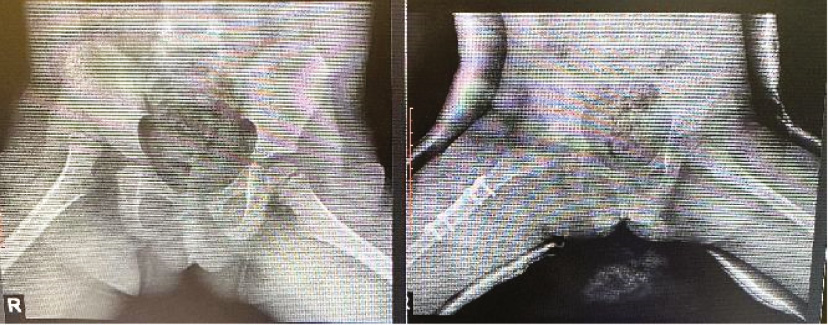
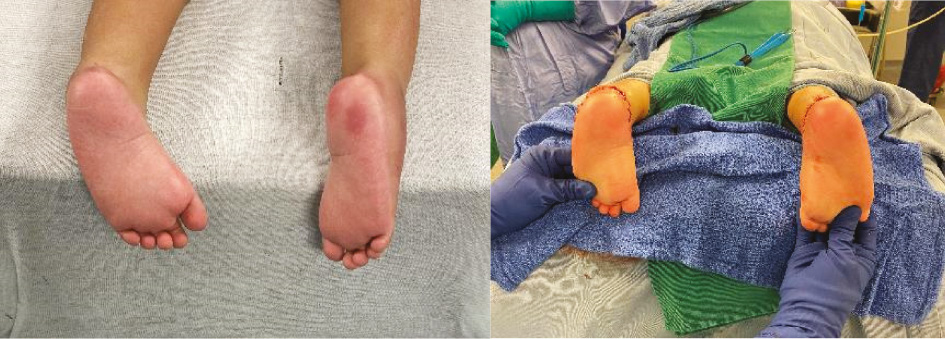
Figure 5. A 4-year-old female with spina bifida and recurrent clubfoot, before and after comprehensive clubfoot release.
Patients contribute for services on a scale, at a significantly lower price than local, private physicians charge. The idea is to help pay forward to the next patient.
Team Members
The Home team at La Vida includes 15 local full-time staff. Dr. Fellers helps screen surgical patients and provides Ponseti casting. Dr. Andres Cabral, a local orthopaedic surgeon fellowship-trained in sports medicine and trauma, also helps screen patients, perform surgeries, and provide postoperative follow-up. Flor Fellers serves as clinic director and Matt Green serves as chaplain, translator, counselor to staff and patients, OR circulator, and C-arm operator.
For each brigade, we aim to have three anesthesia providers, two surgeons, and two scrub techs. Upper-level residents or fellows are also welcome. For this trip, we had three excellent CRNAs: Dianna “Kaye” Graber, Bridget Wolfe, and Barbara Scalet; four surgeons:
Drs. Rambo, Leitch, Badon, PGY V, and Walters, PGY V; and one experienced scrub tech, Kendra Wright, who has been on 17 surgical trips to Ecuador. Dr. Martin Pita, a local anesthesiologist, was also hired to help for the week.
Partner Organizations
La Vida’s main partner is Bayside Medical Missions (BMM), which has partnerships with Samaritan’s Purse; TECH; and its members, Hospital Sisters Outreach; AmeriCares; Hope Haven International; MAP International; Eastern Shore Presbyterian Church (PCA), Fairhope, AL; PET International; Sponsors of the Jubilee Race for Life; and Fundación CASA, Portoviejo.
Community Support
La Vida and BMM work closely with Reales Tamarindos Rotary Club. The club participates by providing volunteers for programs and events, which include the surgical brigades and their organization. The Missionary Alianza Church, on whose campus La Vida is erected, also participates, particularly in the distribution of specialty wheelchairs about every 18 months. The Provincial Government of Manabi, through its Prefectura, has collaborated through yearly agreements reached with La Vida that provide funding for care of certain patient populations. In addition to surgeries, the Prefectura and La Vida collaborate by making programmed trips to outlaying smaller towns and areas. During these trips, patients are treated, and some are identified as surgical candidates.
Local Clinical Support
Excellent follow-up is provided by Drs. Fellers and Cabral. Dr. Cabral lives in Portoviejo and is able to provide consistent clinical follow-up and communication with surgeons if needed. Pre- and postoperative medical care are also provided by
Dr. Juan Avila, who is on staff.
Mission Travel Journal
Murphy Walters, MD
Pre-Trip Preparations
The surgery suites at La Vida were surprisingly well-stocked. Other than everything being reusable, it was not much different from our operating rooms back home. However, in preparation for the trip, we decided to bring a few specific things that we might need. In particular, we brought a set of blade plates (non-cannulated), drills, batteries, and as many gloves as we could get away with. Fortunately, the customs officers did not ask too many questions.
Day 1–Friday
Dr. Leitch, Justin [Dr. Badon, fellow resident], and I arrived in Quito, Ecuador, on a Friday night and stayed in a hotel next to the airport. At the hotel restaurant, we met one of our CRNAs, Bridget, who had flown in from Virginia.
Day 2–Saturday (Clinic Day)
We woke up early Saturday morning to catch a 6 AM flight into Manta, where we were greeted by one of our bus drivers who would be with us for the rest of the trip. After about a 30-minute bus ride, we arrived at the La Vida surgery center in Portoviejo. As we disembarked, there were already about 30 patients sitting in the waiting room. We quickly met the rest of our team and split into two groups with Drs. Leitch and Rambo as the attending physicians with a resident in each group as well.
In the months prior to our arrival, each patient had previously been determined as a possible surgical candidate by one of the full-time physicians at La Vida (Dr. Fellers or Dr. Cabal). We would review the patient chart and pull up their radiographs as one of the nurses brought the patient back. Knowing some Spanish was helpful, but translators were available for every patient. After taking a history and getting an exam, we would determine a treatment plan and, when indicated, schedule them for surgery that week. I was overall very impressed by the parents and their level of insight. For instance, I remember the parents of a 6-year-old girl who was battling a septic tibial nonunion. She had suffered a pathologic fracture, which was plated at the last mission trip 6 months prior. The plate was now bent, and she continued to have pain with a nonunion radiographically. The mother had fashioned a rather high-quality brace out of bamboo sticks which she wrapped around her daughter’s leg. The child had never complained of pain; however, the father explained that they hoped the brace would impart stability to help her body fight off the infection. Overall, we saw ∼60 patients and scheduled ∼20 surgeries. After clinic, we hopped back onto the bus to drive 30 minutes into Crucita, where we would stay at the Fellers’ house. That night, we walked to a pizza place down the road for dinner.
Day 3–Sunday
We took Sunday off to recover our strength after a long day in clinic. Several of us woke up early and went for a run on the beach. The tide is low in the morning, so there is plenty of room to run on the sand. Later that day, we walked around Crucita and ate some ceviche for lunch at a local restaurant. That night, and most nights, Flor Fellers cooked an excellent Ecuadorian dinner for us.
Day 4–Monday
This was the first day in the OR. We woke up in time
to eat a quick breakfast and catch the 6 AM bus to La
Vida. Once we arrived at the surgery center, there was a short morning devotional time and then a group meeting at the OR board to go over cases for the day. Then,
Dr. Rambo and I started with bilateral posteromedial club foot releases via the Cincinnati approach (Figure 5). She did one side and let me take the other. Dr. Leitch and my fellow resident were busy with an open hip reduction with a Dega and femoral shortening osteotomy in the other room (Figure 4). At the end of the day, we did another open hip reduction with just a femoral shortening osteotomy. During each case, Dr. Leitch or Dr. Rambo would supervise, while my co-resident or I would perform the majority of the case (Figure 6). I was continually reminded not to throw anything away as nearly everything gets reused. After a long first day in the OR, we got back on the bus around 6 PM to go back to the house in Crucita (Figure 7).
Figure 6. Drs. Rambo and Leitch assist Drs. Murphy and Badon in the operating room.

Figure 7. The group on the bus after a long day of operating. We would go over the cases for the next day and stop to buy some beverages on the way home.

Day 5–Tuesday
We woke up at the usual time to catch the 6 AM bus to La Vida. After the morning devotional, we went to round on the patients from the day before. The patients with open hip reductions were surprisingly very calm and had hardly any complaints. This is in stark contrast to most patients we see back in Mississippi where additional
pain meds are usually requested. However, both the
children and the parents demonstrated more gratitude
than anything else. After rounds were completed,
we started the day with an open hip reduction in one room and a total hip arthroplasty, which was one of Dr. Cabal’s private patients, in another. I got to assist
Dr. Cabal. We did a Hardinge approach, and after he did the acetabulum, he let me do the femoral component.
I then assisted the team to close out the day with another open hip reduction with a femoral shortening osteotomy. We took the bus home and enjoyed one of Flor’s home-cooked meals.
Day 6–Wednesday
The day started as usual with the 6 AM bus to La Vida followed by the morning devotional. Dr. Leitch and I started the day with bilateral VDROs. We used the non-cannulated plates that we had brought from home. This was certainly more technically challenging than the cannulated sets I had used previously. The first side went well. We started by placing a wire in the superior aspect of the femoral head and followed with the chisel inserted beneath the wire. We then made the bone cut and replaced the chisel with the plate. The contralateral side proved more difficult, as we did not have the appropriately sized plate to gain sufficient purchase into the proximal segment. To address this, we used a different plate that allowed placement of screw into the inferior aspect of the neck/calcar region. Our next case was the septic tibial nonunion in a 6-year-old girl. We removed the bent plate and took cultures. We had to remove a segment of bone that appeared nonviable and decided to osteotomize the fibula to allow us to gain compression without creating a varus deformity. We then placed a longer plate in compression mode. We closed out the day with some adductor and hamstring releases. We took the bus home and ate a home-cooked dinner together.
Day 7–Thursday
This was our biggest day in the OR. After starting the day with a morning devotional and rounding, we had an open hip reduction in one room and bilateral achilles and hamstring lengthening in the other. Dr. Rambo and I did the open hip reduction. In this case, she had been chronically dislocated and had formed an impressive pseudoacetabulum with marked capsular hypertrophy. After the femoral shortening osteotomy, we started our anterior hip dissection. Our first attempt at reduction was unsuccessful, so we continued with our dissection and found that we had not adequately released the capsule from the pseudoacetabulum proximally. Once this was accomplished, we were able to easily reduce the hip. Our next case was bilateral femoral shortening osteotomies with bilateral Dega osteotomies. My co-resident and I did the femoral shortenings simultaneously for this one while Drs. Leitch and Rambo supervised. We then took turns doing bilateral Dega osteotomies followed by the spica cast. Our final case was bilateral femoral shortening osteotomies that my co-resident and I took turns doing. That night we drove into Manta and had dinner at a nice restaurant with local seafood (Figure 8).
Figure 8. The group enjoys a celebratory dinner with local seafood on their final day.

Day 8–Friday
This was our final day in Ecuador, and we took it easy in the OR. After morning devotional and rounding, we started with adductor and Achilles releases. The final case was bilateral calcaneal osteotomies with hamstring releases. My co-resident and I each took a side. The crew at La Vida put on a going-away celebration for us at the end of the day. One of the anesthesiologists gave us each some homemade cocoa. We left Crucita in the early afternoon, so we had time to visit Montecristi and get some genuine Panama hats before our flight home out of Manta.
What Are Five Challenges You Experienced During This Trip and How Did You Deal With Them?
- Problem: Did not have the appropriately sized blade plate for a VDRO.
Solution: Use a smaller plate but with a screw option to gain purchase into the calcar region of the proximal segment. - Problem: Not enough staff present to manage the OR.
Solution: Drs. Leitch and Rambo acted as scrub techs for several cases (Figure 9). - Problem: Difficulty reducing a chronically dislocated hip.
Solution: Ensure that you have adequately released the psoas from the lesser trochanter as well as taken down the capsule from the
pseudoacetabulum proximally. - Problem: Starting on time in the morning.
Solution: Allow the CRNAs to go straight into the preop area to get patients ready for the day instead of rounding. - Problem: Unsure what instrument to ask for.
Solution: Have Kendra as your scrub tech. She knows what you need after participating in 17 brigades (Figure 10).
Figure 9. Dr. Leitch fills in as scrub tech while Dr. Walters helps open trays.
Figure 10. Dr. Rambo with scrub tech extraordinaire Kendra Wright.

Case or Tip of the Trip
When preparing for a VDRO, make sure that you have the correct-sized plates. If not, make sure you have screw options for proximal fixation.
Tips for Trainees
- Never get in a rush.
- Don’t be afraid to say you’re not comfortable doing something.
- The most important thing is always the safety and well-being of the patients. Take ownership of each patient and know that any potential complications will be managed and followed by the full-time doctors at La Vida. Do all you can to prevent them from happening.
Additional Links
Interested in joining a pediatric brigade?
Website: https://www.baysidemedicalmissions.org
Instagram: @centromedicolavida
E-mail: [email protected]
Disclaimer
The authors have no conflicts of interest to disclose related to this manuscript.
