Quality Improvement Case Series
Loss of Fixation of a Type IV Supracondylar Humerus Fracture Treated with Three Divergent Lateral Pins
Baylor Scott and White Medical Center, Department of Orthopaedic Surgery, Temple, TX
Correspondence: Patrick M. Ryan, MD, Baylor Scott and White Medical Center, Department of Orthopaedic Surgery, 2401 South 31st St., Temple, TX 76508. E-mail: [email protected]
Received: February 8, 2023; Accepted: March 29, 2023; Published: May 1, 2023
Volume 5, Number 2, May 2023
Abstract
Supracondylar humerus fractures are common injuries encountered by orthopaedic surgeons. Closed reduction and percutaneous pin fixation is classically considered the standard of care treatment for these injuries, as this treatment method minimizes trauma to the soft tissues, are associated with few complications, and have a high rate of success. However, loss of fixation, when occurring, can lead to cosmetic, functional, and neurological complications. We present a case study of a displaced supracondylar humerus fracture initially treated with three lateral divergent pins that lost fixation and underwent subsequent surgical revision.
Key Concepts
- Failure to engage both the fracture fragment and the intact proximal shaft may lead to loss of fixation.
- Rotating the fluoroscopy machine while keeping the elbow fixed allows for obtaining intraoperative imaging while minimizing the risk of fracture displacement or subsequent loss of fixation.
- A trans-olecranon pin may be a helpful reduction tool in significantly unstable fracture patterns.
- Casting should be considered for postoperative immobilization in Gartland Type III or Gartland IV fractures.
Introduction
Supracondylar humerus fractures are the most common elbow fracture in children aged 5-7 years.1 Fractures are described as non-displaced or minimally displaced, Type I; displaced with intact cortex, Type II; or completely displaced, Type III. Most commonly, the distal fragment displaces posteriorly, as in an extension-type fracture. Extension type fractures encompass as much as 90-98% of all fractures.1–5 A Type IV fracture is unstable in both flexion and extension.3
Non-displaced fractures can be successfully managed with a long arm cast.2–4 Type II-IV injuries are routinely managed operatively. Surgical intervention is typically performed via closed reduction with percutaneous pinning using lateral, divergent pin fixation, which has become popular as a means to avoid iatrogenic ulnar nerve injury.2–4 Two to three divergent pins are successful in most supracondylar fractures. Rarely open reduction with an anterior or medial incision is necessary, such as in an irreducible fracture, failure of the pulse to return following reduction with a cool, pale hand, or an open fracture.2–4 While pin fixation is often successful, loss of fixation can lead to cosmetic and functional consequences.6–11 We present a case of loss of fixation of a supracondylar humerus fracture treated with three divergent lateral pins and this case serves as mechanism to discuss optimal pin strategy for these fractures.
Case Report
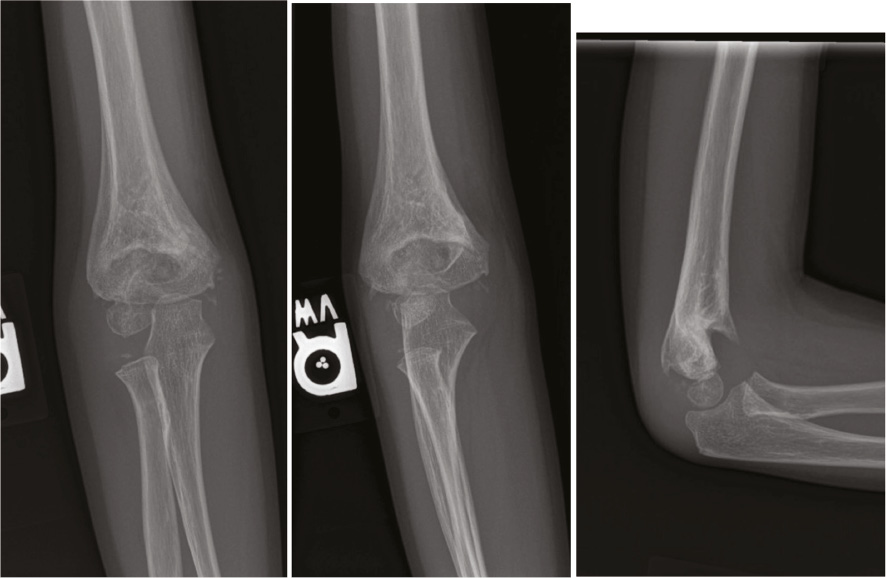
An otherwise healthy 5-year-old male sustained a right upper extremity injury after falling from the top bunk of a bunk bed. Physical exam was notable for gross deformity about the elbow with associated ecchymosis and a positive brachialis sign. Neurovascular exam revealed no palpable radial or ulnar pulse, but the hand and arm were pink and warm. On radiographic imaging, he was found to have a Gartland Type III supracondylar humerus fracture (Figure 1) and a displaced distal radius and ulnar fracture was also noted.
Figure 1. Anteroposterior (AP) (left), Oblique (middle), and lateral (right) radiographs of the initial injury demonstrating a Gartland III posterolateral supracondylar humerus fracture.

The patient was taken urgently to the operating room by the orthopaedic surgeon on call. Attention was first given to the distal radius fracture, which was reduced with traction and manipulation without complication. Following this, attention was turned to the elbow. Multiple reduction maneuvers were performed, and the elbow was determined to be a Gartland Type IV. After adequate reduction was obtained, two bi-cortical pins were inserted. A third pin was placed between these two pins for added stability (Figure 2). After fixation, the radial pulse was not palpable and had weak but present triphasic doppler signals. A long arm splint was then applied. The patient was admitted for compartment checks and serial neurovascular evaluations. The patient was discharged home on postoperative day one.
Figure 2. Intraoperative AP (left), lateral column (left middle), medial column (right middle), and lateral (right) images of fixation from initial urgent index procedure.

The patient followed up in the on-call orthopaedic surgeon’s clinic on postoperative day 7, where repeat imaging was obtained (Figure 3). The images obtained were noted by the on-call surgeon to be imperfect but adequate enough to conclude the fracture to be stable at that time. At subsequent follow-up 8 days later (about 2.5 weeks from the index surgery), repeat imaging was obtained and, unfortunately, notable displacement was identified (Figure 4). Pediatric orthopaedic surgery was then consulted, and the patient was consented for revision fixation.
Figure 3. AP (left), oblique (center), and lateral (right) images obtained at postoperative day 7 following the index procedure.

Figure 4. AP (left), oblique (middle), and lateral (right) images obtained approximately 2.5 weeks following the index procedure demonstrating loss of reduction with interval displacement of the fracture.

The patient was taken to the operative room 17 days after the index procedure, and the pins were removed, but the abundant callus did not allow for closed manipulation. A 2.0 Steinmann pin was inserted posteriorly in the humerus at the fracture site. Osteoclasis was performed with the pin, and the fracture was manipulated with a trans olecranon pin temporarily holding the fracture. The fracture remained highly unstable, and the reduction was quite challenging. The fracture was held reduced and two divergent lateral pins were placed. The fracture was evaluated and found to still be unstable. A small incision was made medially, and the ulnar nerve was gently reflected posteriorly and protected. A medial pin was inserted anterior to the nerve across the fracture site (Figure 5). Following this, the fracture was found to be stable to rotational stress.
Figure 5. AP (left), lateral column (left middle), medial column (right middle), and lateral (right) fluoroscopic images taken at the time of revision fixation demonstrating the addition of the trans-olecranon and medial pins.

The patient was then placed into a long arm cast and followed in pediatric orthopedic clinic. The pins were removed at 4 weeks postoperatively. There was no nerve deficit, and the radial and ulnar pulses were 2+. Through the patient’s postoperative course, reduction was maintained, and successful union of his fracture was achieved. The patient was cleared for follow-up as needed 3 months following surgery (Figure 6).
Figure 6. AP (left), oblique (middle), and lateral (right) radiographs taken 3 months after revision fixation demonstrating healing of the fracture within acceptable coronal plane alignment.
Discussion
Supracondylar humerus fractures are the most common elbow injury treated by orthopaedic surgeons. Treatment with closed reduction includes manipulation with traction, reducing the fracture in the coronal plane, followed by flexion and percutaneous lateral-based pin fixation. While often quite successful, lateral pinning has a loss of reduction rate of as high as 15%.9 This case is an unfortunate example of such loss of reduction ultimately requiring additional surgery in the form of revision fixation.
Type IV supracondylar fractures present a unique challenge and are unstable in multiple planes with torn periosteum that cannot assist with reduction. In a Type IV fracture, there may be interposed periosteum and possible soft tissue within the fracture. These fractures are difficult to reduce with traditional maneuvers. A common error occurs when struggling with achieving appropriate length of the fracture by hyperflexing the elbow, leading to impaction and comminution of the anterior cortex with mal reduction.
During reduction of supracondylar humerus fractures, fluoroscopic imaging is utilized. The arm is often gently rotated in order to obtain AP and lateral images. In a Type IV fracture, manipulating the arm in external rotation to achieve a lateral view may not be possible, as the fracture can rotate. It is important to recognize if a fracture is unstable and rotating during positioning for x-rays, have the room set up to instead move the fluoroscopy beam, and leave the arm in the reduced position.
There are multiple risk factors found to be associated with potential loss of reduction following pin fixation. Many of these factors are related to the placement and trajectory of the pins. Sankar et al.’s retrospective review found that all cases with subsequent loss of reduction had at least one of the following errors: failure to capture both fragments with at least two pins, failure to obtain bicortical fixation with at least two pins, pin spread of less than 2 mm across the fracture site.6 In addition to appropriate pin spread across the fracture site, pin convergence is also a notable risk factor for subsequent loss of reduction.8 In this case, the initial two superior pins appear parallel, while the inferior pin appears convergent with the middle pin. Moreover, it appears only one initial pin engaged the dominant inferomedial fragment.
The efficacy and safety of medial pins continue to be debated. Many studies have suggested that the stability and functional outcome of cross-pin fixation or medial pin constructs are no different from lateral pins alone.7,10 However, biomechanical analysis has shown increased torsional strength with medial pin additions.12 While the risk of iatrogenic ulnar nerve injury is as high as 5%, various “mini-open” techniques have been described to minimize iatrogenic injury to the ulnar nerve.11 In light of this, while initial treatment options may steer away from the use of a medial pin, in the revision setting, with the initial inability to capture the dominant inferomedial fragment, a medial pin was added. The medial pin was an important contributor to the stability and success of the revision fixation, and no iatrogenic injury to the ulnar nerve was encountered postoperatively.
The use of a splint versus a cast in postoperative immobilization following elbow pinning has not been extensively studied. While splinting may be less expensive and may be associated with fewer soft tissue complications,13 Lee et al. have shown a small but statistically significant increase in the re-operation rate of supracondylar humerus fractures treated with a splint as opposed to a cast.14 Given the significant amount of initial displacement and amount of inherent instability, immobilization with a cast may have potentially aided maintenance of initial post-operative reduction after the index procedure. Additional studies are necessary to fully understand the contribution of immobilization method to the success of treatment.
Additional Links
- JPOSNA® May 2023, Commentary to Quality Improvement Case Series: Loss of Fixation of a Type IV Supracondylar Humerus Fracture Treated with Three Divergent Lateral Pins
- POSNA Study Guide, Supracondylar Humerus Fractures
- POSNAcademy, POSNA Community Webinar - Pediatric Supracondylar Fractures
- POSNAcademy, The Pink, Pulseless Pediatric Supracondylar Humerus Fracture
Disclaimer
The authors report no conflicts of interest related to this manuscript.
References
- Omid R, Choi PD, Skaggs DL. Supracondylar humeral fractures in children. J Bone Joint Surg Am. 2008;90(5):1121-1132.
- Price CT, Flynn JM. Management of fractures. In: Lovell & Winter’s Pediatric Orthopaedics. Ed 6. Philadelphia, PA: Lipincott Williams & Wilkins; 2006:1450-1452.
- Green N, Swiontkowski. Supracondylar fracture. In: Green’s Skeletal Trauma in Children. Ed 4. Elsevier; 2008. Chapter 9.
- Abzug JM, Herman MJ. Management of supracondylar humerus fractures in children: current concepts. J Am Acad Orthop Surg. 2012;20(2):69-77.
- Otsuka NY, Kasser JR. Supracondylar fractures of the humerus in children. J Am Acad Orthop Surg. 1997;5(1):19-26.
- Sankar WN, Hebela NM, Skaggs DL, et al. Loss of pin fixation in displaced supracondylar humeral fractures in children: causes and prevention. J Bone Joint Surg Am. 2007 Apr;89(4):713-717.
- Bitzer AM, Belkoff SM, LiBrizzi CL, et al. Sagittal plane alignment affects the strength of pin fixation in supracondylar humerus fractures. Medicine (Baltimore). 2021 Jun 4;100(22):e26173.
- Venkatadass K, Maji M, Sangeet G, et al. Factors determining loss of reduction in paediatric supracondylar humerus fractures treated by closed reduction and percutaneous pinning. J Pediatr Orthop B. 2022 May 1;31(3):289-295.
- Pennock AT, Charles M, Moor M, et al. Potential causes of loss of reduction in supracondylar humerus fractures. J Pediatr Orthop. 2014 Oct-Nov;34(7):691-697.
- Prashant K, Lakhotia D, Bhattacharyya TD, et al. A comparative study of two percutaneous pinning techniques (lateral vs medial-lateral) for Gartland type III pediatric supracondylar fracture of the humerus. J Orthop Traumatol. 2016 Sep;17(3):223-229.
- Green DW, Widmann RF, Frank JS, et al. Low incidence of ulnar nerve injury with crossed pin placement for pediatric supracondylar humerus fractures using a mini-open technique. J Orthop Trauma. 2005 Mar;19(3):158-163.
- Lee SS, Mahar AT, Miesen D, et al. Displaced pediatric supracondylar humerus fractures: biomechanical analysis of percutaneous pinning techniques. J Pediatr Orthop. 2002 Jul-Aug;22(4):440-443.
- Sawyer JR, Ivie CB, Huff AL, et al. Emergency room visits by pediatric fracture patients treated with cast immobilization. J Pediatr Orthop. 2010;30:248-252.
- Lee HA, Buczek MJ, Talwar D, et al. Post-operative splinting versus casting of pediatric supracondylar humerus fractures. Cureus. 2021;13(9):e17635.
