Surgical/Technical Tips
Methods to Facilitate Reduction of Medial Epicondyle Fractures in the Supine Position
1Department of Orthopaedic Surgery, Dwight D. Eisenhower Army Medical Center, Fort Gordon, GA; 2Department of Pediatric Orthopaedic Surgery, Children’s Healthcare of Atlanta Scottish Rite, Atlanta, GA
Correspondence: K. Aaron Shaw, DO, Department of Orthopaedic Surgery, Dwight D. Eisenhower Army Medical Center, 300 E. Hospital Road, Fort Gordon, GA 30905. E-mail: [email protected]
Received: April 28, 2022; Accepted: June 12, 2022; Published: August 1, 2022
DOI: 10.55275/JPOSNA-2022-0081
Volume 4, Number 3, August 2022
Abstract:
Surgical treatment of medial epicondyle fractures aims for the restoration of the medial elbow osseous, muscular, and ligamentous anatomy, with the desired outcomes of obtaining a stable elbow with full range of motion and normal strength. Some surgeons have advocated for fixation in the prone position in order to relax the flexor pronator mass which tends to displace the fragment in the supine position. In this paper, we highlight methods that ease reduction without the increased time and anesthetic consideration needed to position the patient prone.
Key Concepts:
- The medial epicondyle fragment will be displaced distal and anterior secondary to the pull of the forearm flexor muscles. Prone positioning of the patient can reduce these forces and ease fixation.
- Supine positioning of the patient is easier for the entire surgical team yet attempts to expose and reduce the fragment can be thwarted by a natural tendency to place a valgus load on the elbow.
- We present methods to improve ease of fixation in the supine position.
Introduction
Medial epicondyle fractures account for 11–20% of pediatric elbow fractures and frequently present in association with an elbow dislocation.1 Operative management of displaced pediatric medial epicondyle fractures is a controversial topic. With the exception of incarcerated, intra-articular fragments and open fractures, there are no universally accepted displacement parameters for indicating operative management with reported acceptable displacements ranging from 5-20 mm in the literature.2–5 Associated elbow dislocation6 and participation as an overhead athlete7 have been cited as relative indications for surgical fixation in limiting range of motion loss and facilitating early functional recovery and return to activities. Although the indications may be disputed, the aim of surgical treatment, once decided upon, is to restore the medial elbow osseous, muscular, and ligamentous anatomy in order to obtain a stable elbow without functional comprise (Figure 1). The purpose of this paper is to demonstrate methods to aid reduction in the supine position.
Figure 1. Index case: A 12-year-old gymnast with a displaced medial epicondyle fracture who is indicated for fixation.

Description of the Method
Patient Positioning and Preparation
In the supine position, anesthesiologists are not normally required to use an endotracheal tube (ET) to manage the airway. Conversely, prone positioning requires careful positioning of the head and neck and use of muscle relaxation to place the ET (Figure 2). Muscle relaxation used to intubate the patient may help relax the forearm musculature to aide in reduction, but this may also block any twitching of the hand should inadvertent dissection occur near the ulnar nerve. We prefer to use the supine position with some simple methods to aid in reduction.
Figure 2. Prone positioning for medial epicondyle fracture fixation requires intubation and careful positioning of the head and neck. Fixation in this position does decrease the valgus moment on the elbow and facilitates reduction.

Once in the operating room, the child is positioned supine on an operating table with a radiolucent hand table. As the surgeon will be seated on the medial side of the arm, fluoroscopy monitors are positioned on the lateral side of the arm to facilitate viewing. The child’s operative arm is abducted 90 degrees and slightly externally rotated to expose the medial elbow. A sterile or non-sterile pneumatic tourniquet can be applied to facilitate surgical exposure based upon the size of the patient. For smaller children, a sterile tourniquet is preferred to ensure adequate surgical exposure can be obtained. Key Point: In order to relax the flexor pronator mass, we will flex the fingers and wrist and secure them in this position with sterile Coban (Figure 3). A sterile bump may be placed under the elbow to facilitate reduction and implant placement.
Figure 3. The wrist and fingers are flexed and held in this position during ORIF in order to decrease pull on the medial epicondyle. Surgical fixation for this fracture is usually short in duration and thus we have not had any issues with median nerve compression.

A 2-4 cm longitudinal incision is made overlying the medial epicondyle’s origin of the distal humerus. During the incision, the authors prefer to slightly extend the elbow less than 90 degrees to allow the ulnar nerve to relax posterior to the fracture bed. Key Point: Try to avoid excessive valgus stress on the elbow during reduction, as this tends to displace the fragment. The ulnar nerve should be visualized and carefully protected. The surgeon does not need to release the cubital tunnel, but visual confirmation is important to ensure adequate protection throughout the case. The fracture fragment is identified and the fracture bed on the distal humerus is prepared with removal of any interposed soft tissue. Key Point: We advocate for the removal of the apophyseal cartilage with a curette from the undersurface of the fragment and the distal humerus to facilitate faster osseous union. To obtain fracture reduction, the fracture fragment may be manipulated with a dental pick. Key Point: A #1 vicryl suture inserted through the tendinous insertion can facilitate reduction (Figure 4).
Figure 4. Clinical image demonstrating the use of a suture and dental pick to facilitate reduction of a displaced medial epicondyle fracture fragment to the distal humerus.

When dealing with fractures that are fixed more than 10 days from injury, the contracted muscles may make reduction difficult. Key Point: Fascial lengthening of the flexor mass can be done to increase length to facilitate the reduction with less tension on the medial epicondyle fragment (Figure 5). Care is needed to incise only the fascia and have visual protection of the ulnar nerve.
Figure 5. Chronically displaced medial epicondyle fractures may be difficult to reduce without a fascial release.

With the fracture held in its reduced position, taking into consideration its posterior anatomic location, the preferred implant can used to obtain fixation. The authors prefer to obtain rigid fixation using a cannulated screw construction unless the fragment is deemed too small to accept a screw without risk of fragmentation, in which case suture anchor fixation is preferred. Prior to screw placement, the reduction is confirmed under biplanar radiography, ensuring that the guidewire for screw insertion avoids the olecranon fossa. To obtain rigid fixation, a 1.25 mm guidewire is placed carefully to avoid the olecranon fossa for a 4.0 mm fully threaded cannulated screw. The authors prefer a fully threaded screw in lag by technique fashion as they can be easier to remove at a later date compared to partially threaded screws. Based upon the size of the fracture fragment, smaller sized screws can be utilized to avoid fragmentation during screw placement. Key Point: A second guidewire may be used if the fracture is of sufficient size to provide provisional fixation and also rotational stability during drilling and early screw insertion (Figure 6).
Figure 6. Clinical image demonstrating the medial epicondyle fracture fragment reduced and held in place with two 1.25 mm guide wires for cannulated screw.
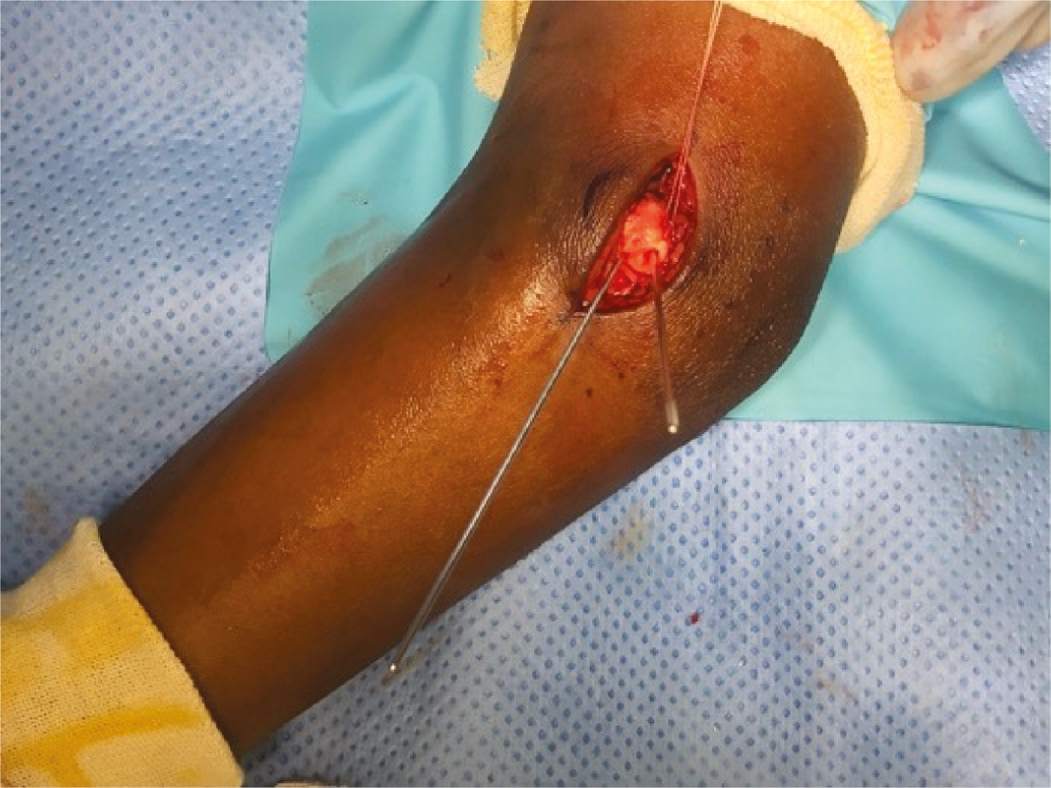
The authors prefer obtaining anteroposterior, lateral, internal oblique, and external oblique images to confirm implant placement in the medial column of the distal humerus. Once confirmed, an appropriate length screw is selected and the guidewire is over-drilled using size-specific cannulated drill bits, using lag-by-technique fixation with a fully threaded screw which is then inserted over the guidewire. A washer may be used at the discretion of the surgeon in conjunction with the screw to increase the surface area of fixation. Key Point: If a provisional guidewire is used to maintain the reduction, it is removed just prior to compressing the fragment. The screw guidewire is then removed after fully seating the screw and final radiographic images are obtained (Figure 7).
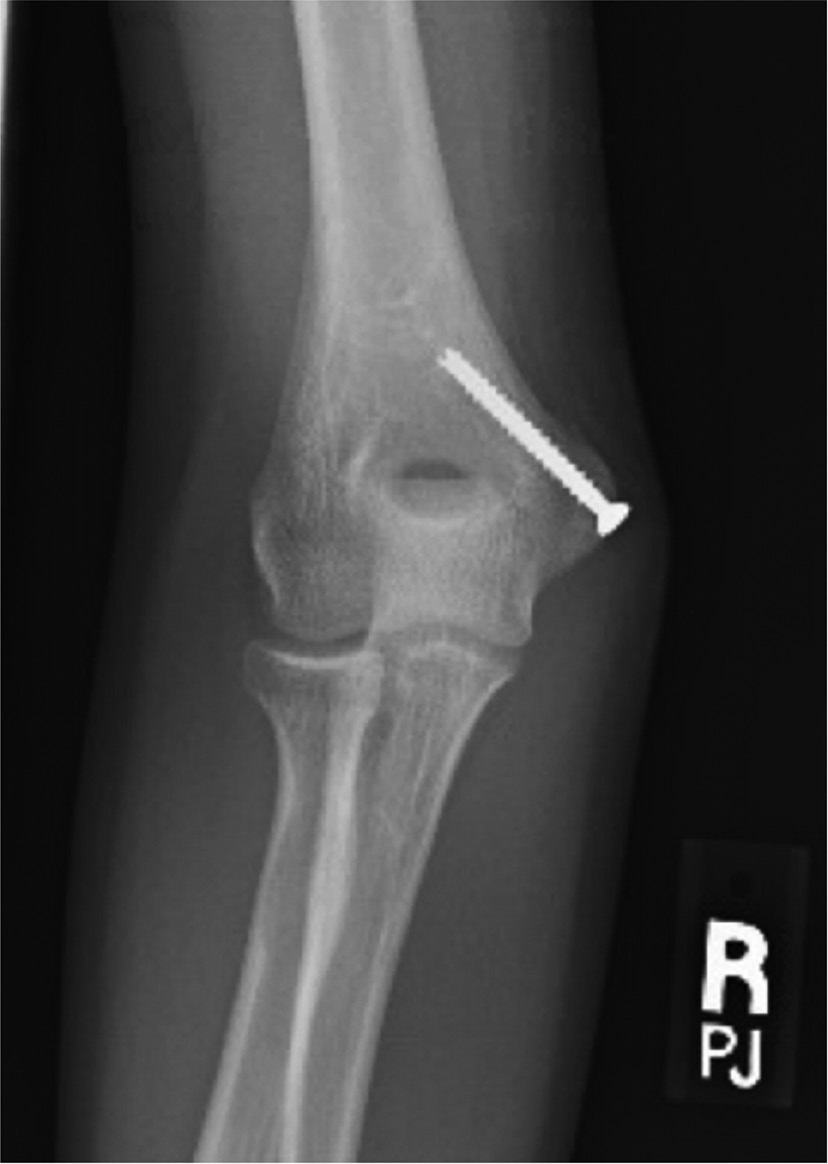
Figure 7. Healed anteroposterior radiograph showing screw fixation following ORIF of medial epicondyle fracture.
Once the procedure is completed, it is vital to check the range of motion as well as to perform a secondary evaluation for valgus instability. Prior to closure, the ulnar nerve should be directly inspected to ensure that it is not entrapped within the fracture bed. The incision then undergoes standard, layered closure and placement of surgical dressings, followed by placement of a long arm cast or posterior splint.
Postoperative Care
The use of immobilization following surgery depends on the type of fracture and the rigidity of fracture fixation. In cases of rigid fixation with a compliant patient, a hinged elbow brace can be utilized in the immediate postoperative period, protecting the elbow from valgus stress while allowing early elbow flexion and extension. If there is concern regarding the rigidity of fixation or patient compliance, a fiberglass cast that is univalved or bivalved is placed with the elbow in 70-80 degrees of flexion for 2 weeks, followed by early, guided range of motion in a hinged elbow brace. For cases treated with K-wire or suture fixation, the elbow should be protected in a splint or cast for 3 weeks or until the surgeon is satisfied with the radiographic appearance or until the K-wire(s) are removed.
What to Avoid
- The ulnar nerve courses posterior to the medial epicondyle fragment through the cubital tunnel. It should be carefully identified and protected throughout the case, ensuring to avoid placing unnecessary tension on the nerve.
- Screw placement should avoid traversing the olecranon fossa, an error which can limit elbow extension. The authors prefer confirming guidewire placement with AP, Lateral, Internal Oblique, and External Oblique images to ensure accurate placement in the medial column.
- Prolonged immobilization can result in significant arthrofibrosis. Stability of the elbow imparted through fracture fixation should permit early protected motion to minimize the risk of elbow stiffness.
- When placing the guide pin, it is important to avoid advancing it beyond the far cortex, as this has the potential to injure the radial nerve and can cause a postoperative radial nerve palsy.8
Discussion
While the operative indications for displaced, pediatric medial epicondyle fractures remain controversial, surgical intervention continues to have an important role in their management. The ability to obtain an anatomic reduction while restoring valgus stability to the elbow is vital. Open reduction with rigid internal fixation performed can aide in early mobilization and functional recovery for the appropriately indicated patients.
In recent years, prone position for ORIF of pediatric medial epicondylar fractures has gained considerable attention.9–11 Proponents of this method report that the positioning avoids the inherent supination force and valgus load experienced at the elbow with supine positioning.9 However, there has been no statistically significant differences identified between supine and prone position in patient outcomes for the treatment of pediatric medial epicondylar fractures,11 indicting that both methods are viable options based upon the treating surgeon’s experience and comfort. In this paper we demonstrate some simple methods to more easily obtain reductions in the supine position.
Additional Links
- POSNAcademy: Medial Epicondyle Fracture: Operative Technique, David L. Skaggs, MD, MMM—https://bit.ly/3Pc8fWM
- POSNAcademy: Pediatric Medial Epicondle Humerus Fracture: Open Reduction and Internal Fixation, James D. Bomar, MPH; Andrew T. Pennock, MD; Eric W. Edmonds, MD—https://bit.ly/3ADguqI
- POSNAcademy: Medial Epicondyle Fractures: Should We Operate or Not?, Joshua M. Abzug, MD—https://bit.ly/3bXZ65Q
Disclaimer
No funding was received for the completion of this project. K. Shaw: Committee member for AAOS and NASS; J. Murphy: Consultant for DePuy and OrthoPediatrics, stock options from Alphatec, research support from Epic and OrthoPediatrics, committee member for POSNA, editorial board member for JPO and Journal of Spine Deformity.
References
- Stans AaM, Todd. Dislocations of the Elbow and Medial Epicondylar Humerus Fractures. 9 ed. Peter M. Waters DLS, John M. Flynn, eds. Philadelphia, PA: Wolters Kluwer; 2020.
- Farsetti P, Potenza V, Caterini R, et al. Long-term results of treatment of fractures of the medial humeral epicondyle in children. J Bone Joint Surg Am. 2001;83(9):1299-1305.
- Lee HH, Shen HC, Chang JH, et al. Operative treatment of displaced medial epicondyle fractures in children and adolescents. J Shoulder Elbow Surg. 2005;14(2):178–185.
- Dias JJ, Johnson GV, Hoskinson J, et al. Management of severely displaced medial epicondyle fractures. J Orthop Trauma. 1987;1(1):59-62.
- Hines RF, Herndon WA, Evans JP. Operative treatment of medial epicondyle fractures in children. Clin Orthop Relat Res. 1987;(223):170-174.
- Knapik DM, Fausett CL, Gilmore A, et al. Outcomes of nonoperative pediatric medial humeral epicondyle fractures with and without associated Elbow dislocation. J Pediatr Orthop. 2017;37(4):e224-e228.
- Cain EL, Jr, Liesman WG, Fleisig GS, et al. Clinical outcomes and return to play in youth overhead athletes after medial epicondyle fractures treated with open reduction and internal fixation. Orthop J Sports Med. 2021;9(2):2325967120976573.
- Hallwachs A, Weber M, Liu R, et al. Operative management of pediatric medial epicondyle fractures: lessons better learned the easy way. J POSNA. 2021;3(4).
- Glotzbecker MP, Shore B, Matheney T, et al. Alternative technique for open reduction and fixation of displaced pediatric medial epicondyle fractures. J Child Orthop. 2012;6(2):105-109.
- May CJ, Shore BJ. Open reduction and internal fixation of pediatric medial epicondylar humeral fractures in the prone position. JBJS Essent Surg Tech. 2021;11(2):e19.00069.
- Baghdadi S, Weltsch D, Arkader A, et al. Open reduction of medial epicondyle fractures in the pediatric population: supine versus prone position. J Pediatr Orthop. 2021;41(5):273-278.
