JPOSNA® Special Edition
Advances in Pediatric Orthopaedic Education and Technical Training
Top Gun–A Novel Simulation Program to Test the Skills of Pediatric Orthopaedic Trainees
1Boston Children’s Hospital, Boston, MA
Correspondence: Benjamin J. Shore, MD, MPH, FRCSC, Boston Children’s Hospital, 300 Longwood Ave., Hunnewell 211, Boston, MA, 02115. E-mail: [email protected]
Received: April 18, 2022; Accepted: June 5, 2022; Published: August 15, 2022
DOI: 10.55275/JPOSNA-2022-0057
Volume 4, Number S1, August 2022
Introduction
Historically, orthopaedic surgery has been learned through a mentorship model, with didactic lectures followed by repeated practice on patients under careful supervision.1 Although this “See one, Do one, Teach one” model of education has been utilized in North America over the last century, there is growing evidence/emphasis on surgical simulation as a means of improving medical education, optimizing clinical outcomes, and promoting patient safety.2–5 Specifically in recent years, orthopaedic simulation has become an important component of the training process, providing a way for trainees to practice operative tasks in a protected environment without patients at risk.6 The potential impact of quality, safety, and value are magnified when dealing with the pediatric patient, given the relative infrequency of clinical conditions treated as well as the compounded morbidity associated with unsuccessful or suboptimal intervention a simulation platform for pediatric orthopaedic surgery is required.7
In 2012, during the International Pediatric Orthopaedic Symposium (IPOS®), Top Gun was introduced as a new pediatric orthopaedic simulation contest designed to test fundamental skills related to pediatric orthopaedics and highlight POSNA’s commitment to simulation and surgical education. Under the leadership of then IPOS® Course Director John (Jack) M. Flynn MD, this surgical simulation program was initially designed by Donald S. Bae, MD, with a focus to improve task performance, maximize clinical outcomes, promote patient safety, and optimize orthopaedic training. In the beginning, a series of four timed motor skill stations were developed to test fundamental skills related to pediatric orthopaedics. Specifically, trainees were tested on their ability to close reduce a distal radius and apply a short arm cast, pin a slipped capital femoral epiphysis bone model, instrument a lumbar pedicle screw for scoliosis surgery, and place an arthroscopic knot during knee arthroscopy. The IPOS® Top Gun program was inspired in part by a similar surgical skills competition held by the American Association of Neurological Surgeons. Over the last decade, the program has evolved to include six stations and 36 trainees with additional simulations focused on the application of a clubfoot cast, performance of an Achilles tenotomy, and the participation in a team challenge which involves group interaction to help solve a clinical problem, most recently surrounding the loss of neuromonitoring signals while performing a spinal fusion. In the past, a virtual reality septic hip module has been tested and validated using Top Gun participants.7
Argyris8 originally coined the terms “single-loop learning” and “double-loop learning” in his work as an organizational psychologist. Single-loop learning relates to skill acquisition and mastery of a known skill set (pinning a slipped capital femoral epiphysis, close reducing a distal radius fracture, or fixing an ankle fracture). Trainees practice and compare their performance against a sequence of steps as taught by senior residents, mentors, and attendings. Early iterations of Top Gun focused on single-loop learning, with participants being scored on their ability to master a sequence of steps in performance of a pediatric orthopaedic skill. In double-loop learning, learners (with skilled facilitation) attempt to “learn how the very way they act, communicate and interact within the team environment can be the source of problem in its own right.”8 The introduction of the “Team-Challenge” started to test participants in their double-loop learning method, designed to uncover significant differences in communication, team dynamics, and leadership.9
Description of Simulation
The International Pediatric Orthopaedic Symposium (IPOS®) is an annual meeting hosted by POSNA in Orlando, FL, at the beginning of December. This meeting is the pinnacle of pediatric orthopaedic education with a robust faculty of international educators. Top Gun is hosted in the evening of the second night and the simulation is open to trainees (orthopaedic residents and fellows) who are scholarship recipients of the IPOS® meeting. For this simulation, each trainee is scored based on their performance in each of the six simulations. Scores are tallied and prizes are awarded for the top three performers of the simulation.
There are currently six simulation stations with six judges (content expert attendings) grading participants on their simulation performance. Prior to the meeting, participants receive background educational information on each of the simulation stations, which serves as the trainee’s “toolkit.” In the educational packet, participants receive background reading on the technique including indications, rationale, and steps to the procedure. Participants also are given the opportunity to review video(s), which demonstrate each simulation station, and learn the scoring rubric, which will be used by the judges at each station. Each station is approximately 13 minutes in duration with an additional 3-minute debrief at the end to facilitate discussion, learning, and reflection for the trainee. Each station is scored out of 100 total points, and the scores for all six stations are tallied at the end of the simulation.
1. Distal Radius
Participants start this simulation using a distal radius model with a cast already in place. The trainee demonstrates safe removal of the cast using a cast saw. Points are given for proper technique, attention to the soft tissues under the cast, and cooling of the cast saw blade. Once the cast is removed, the participant is then scored on application of a short arm cast to treat a displaced distal radius fracture. Points and attention are made to applying a well-molded cast with the appropriate amount of padding and molding in the correct locations. There are also points awarded for cast application/removal proficiency and cast index. At the end of cast application, the simulation is complete and the debrief takes place.
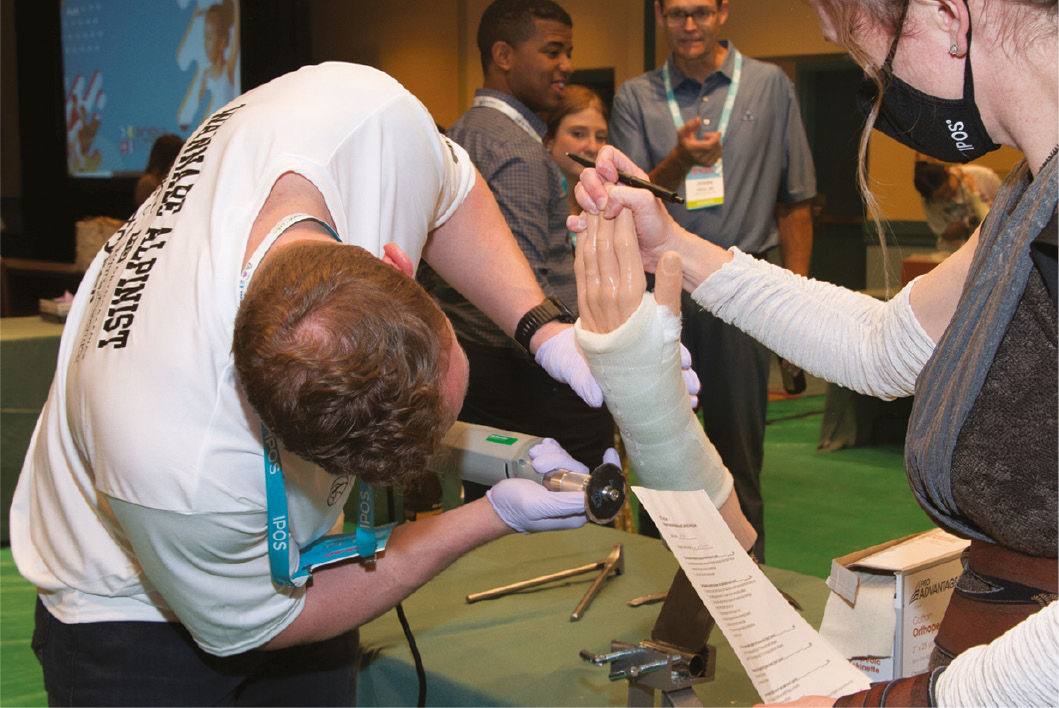
Figure 1. A participant in the distal radius section demonstrates safe cast removal with an oscillating saw.
2. Clubfoot
Here, the participant is using a clubfoot model to apply a long leg cast (MD Orthopaedics, Wayland, IA). During the application, the participant outlines the critical steps for treatment of a clubfoot, specifically outlining the sequence of casting to correct the Cavus, Adductus, Varus, and then Equinus commonly seen with club foot pathology. In addition, important anatomic landmarks are to be identified by the participant during the simulation. Points are awarded for correct cast application and molding in the appropriate anatomic positions over the talar head. At the end of the casting simulation, applicants are tested on their performance of performing a percutaneous tendoachilles lengthening, where points are subtracted for incomplete tenotomy, laceration of the skin, and damage to neurovascular structure.
Figure 2. The Ponseti session with faculty observer and non-clinical volunteer debriefing on the performance of the participant.

3. Slipped Capital Femoral Epiphysis (SCFE)
For the SCFE simulation, a sawbones model (OrthoPediatrics, Warsaw, IN) is used which has a moderate SCFE built into the femur model with posterior slippage of the femoral head. First, the participant is asked a series of short answer didactic questions, which test the participant’s knowledge on associated conditions, what the fluoroscopic images should look like when a perfect lateral is obtained, and how to measure the slip angle. Once this is completed, the applicant has a chance to place a single cannulated screw for fixation for the treatment of the aforementioned SCFE. Points are awarded for centrality of the screw, location of entry point being intracapsular, and efficiency. The fewer attempts the applicant needs to get the screw in the correct position the higher their score.
Figure 3. In the SCFE station, a participant demonstrates the optimal guidewire position for cannulated screw fixation.

4. Scoliosis Instrumentation and Correction
For the spine simulation, participants are tested on their ability to prepare the lumbar spine for pedicle screw instrumentation. Points are awarded for a correct facetectomy, starting point for the probe, and correct use of the pedicle finder. Points are also awarded for screw position in the pedicle and avoiding a breach of one of the walls of the screw tract. Participants are then presented a Lenke I curve with hypokyphosis and points are awarded for rod contouring and correct attachment to the spine. Points are awarded for bending the rod into hyperkyphosis, and the final product position is scrutinized in the coronal and sagittal planes.
Figure 4. A participant demonstrates the technique for preparation of the spinal facets prior to pedicle screw insertion.

5. Arthroscopic Knee Meniscal Fixation
Participants use a Scorpion arthroscopic meniscal repair device (Arthrex, Naples, FL) to place a series of sutures across a meniscal tear and secure using an arthroscopic Weston knot. Participants are graded on the location of sutures across the meniscal tear, assessing spacing of sutures and orientation perpendicular to the tear. The quality of the suture and strength of the knot is tested using a probe to make sure the knot doesn’t displace. In addition, a global rating score is used to assess a participant’s ability to handle the instruments, the flow of the procedure with demonstration of anticipation of future steps, and the overall technical ability of the applicant.
6. Team Challenge
The team challenge is designed to simulate “double-loop” learning for the participant, where they are tested with a difficult clinical scenario and have to interact with other team members to solve the problem and care for the patient. Most recently, participants were faced with the clinical scenario of a loss of neuromonitoring signals during a spinal surgery. They were tested on their ability to manage the event as a team, collect information, and work together to solve the problem. The participants were given the spine checklist and were scored as a team on their ability to run through the checklist in a timely fashion, communicate with other team members, and consider a wake-up test. Individual scoring was given to how well each team member participated in the team and acted as a supportive team member (Appendix 1). This simulation is a marriage of both Zone 1 and Zone 2 simulation principles where trainees are not only rehearsing a series of orchestrated steps but interacting together as a group and making real-time clinical decisions.
Figure 5. The team challenge involves a group of three participants working together to achieve a common goal, working on Zone 1 and Zone 2 simulation principles.

Over the last decade, the Top Gun program has continued to evolve and improve but not without hurdles and some struggle. We have added techniques and skills commensurate with the current evolution seen within pediatric orthopaedics. With experience, we have begun to appreciate the importance of debriefing and have worked hard to build in quality time to allow faculty to give feedback and debrief appropriately with participants. In doing this, we realized that faculty also need training in how to debrief effectively. Furthermore, in an effort to help stimulate healthy competition amongst participants and faculty and to lighten the simulation atmosphere, we have introduced a parallel competition for the faculty—a costume competition. We believe that by engaging all participants of the simulation in healthy competition, we avoid a potentially stressful situation for trainees (performing observed skills in front of subject experts) and exchange it for a fun, light-hearted environment to foster healthy competition amongst colleagues. It seems clear that this “light and fun” environment brings out the best performance in our trainees and their comments below highlight these observations.
Figure 6. To lighten the atmosphere, faculty participate in a costume competition.

Summary
The use of surgical simulation as an adjunctive educational tool for the curriculum of orthopaedic surgical trainees is on the rise. Simulations allows for iterative, deliberate, and problem-based learning and feedback without risk to real patients. In 2013, the American Board of Orthopaedic Surgery required U.S. residency programs to incorporate formal surgical skills education into their curricula. The American College of Surgeons’ strong belief in simulation has led to the creation of the American College of Surgeons Accredited Education Institutes with a goal “to promote patient safety through the use of simulation.”10 Systematic reviews have demonstrated that simulation and virtual reality leads to an improvement of technical skills in orthopaedic surgery,11 further validating the importance of Top Gun and other simulation programs within pediatric orthopaedics.
Over the last decade, the Top Gun surgical simulation program has trained over 300 orthopaedic trainees in the discipline of pediatric orthopaedics. The premise of this program at its onset was to create a fun, interactive learning environment which introduced trainees to simulation and allowed for skill development and mentorship simultaneously. Top Gun has been widely successful over the last decade and is considered one of the highlights of the IPOS® meeting. Here are the perspectives of recent Top Gun winners on what made this simulation experience special for them.

2014 Top Gun Winner
Jennifer Bauer, MD
Spine Surgeon, Seattle Children’s Hospital, Seattle, WA
“There is no better pediatric orthopaedic conference than IPOS®, and as a trainee, there is no better session than Top Gun. Highlights included the one-on-one interaction with multiple field experts while they watch your skills with competition in the air. Surgical coaching is an undervalued aspect of continued growth as a surgeon, one that I seek out now, and started 6 years ago back at Top Gun when I was a PGY4.”

2015 Top Gun Winner
Kenneth D. Illingworth, MD
Pediatric Spine Surgeon, Cedars-Sinai Children’s Hospital, Los Angeles, CA
“I am going to win that competition—I remember practicing my arthroscopic Weston knot tying in my hotel room in Orlando, with suture anchored to the chair leg and knot pushers I got off the internet, until my fingers were bleeding. My experience with trainee simulation and the Top Gun competition has inspired me to continue to dedicate my career to improving education and simulation for the next generation of residents.”

2018 Top Gun Winner
Chrissy M. Goodbody, MD, MBE
Pediatric Orthopaedic Surgeon, Children’s Hospital of Philadelphia, Philadelphia, PA
“The chance to practice your skills in front of the leaders in the field, and to get immediate feedback on how to improve, was invaluable. The ability to practice important skills in a controlled, low-risk, low-stress, carefully observed setting before performing them in high-stakes situations on a real patient in a real operating room is invaluable. The dedication and effort that the faculty at Top Gun puts toward education, training, and mentoring the next generation of pediatric orthopaedic surgeons is extraordinary.”
The future for simulation in pediatric orthopaedics is bright. Developing alternative simulation strategies to enhance trainee education, engagement, and participation should continue to be a priority of POSNA and all of its members. In addition to testing and training our future pediatric orthopaedic surgeons, the Top Gun program serves as a model for trainees to learn how to improve skill, enhance communication/teamwork, and optimize patient safety in a safe environment, which allows for continued repetition without patient harm.
Disclaimer
The author has no conflicts of interest to report.
References
- Kneebone R, Aggarwal R. Surgical training using simulation. BMJ. 2009;338:b1001.
- Brubacher JW, Karg J, Weinstock P, et al. A novel cast removal training simulation to improve patient safety. J Surg Educ. 2016;73(1):7-11.
- Atesok K, Mabrey JD, Jazrawi LM, et al. Surgical simulation in orthopaedic skills training. J Am Acad Orthop Surg. 2012;20(7):410–422.
- Pedowitz RA, Marsh JL. Motor skills training in orthopaedic surgery: a paradigm shift toward a simulation-based educational curriculum. J Am Acad Orthop Surg. 2012;20(7):407-409.
- Bae DS, Waters PM. Pediatric orthopedic surgical simulation at Boston Children’s Hospital. J Pediatr Orthop B. 2016;25(4):292-295.
- Sugand K, Mawkin M, Gupte C. Validating touch surgery: a cognitive task simulation and rehearsal app for intramedullary femoral nailing. Injury. 2015;46(11):2212-2216.
- Shore BJ, Miller PE, Noonan KJ, et al. Predictability of clinical knowledge through mobile app-based simulation for the treatment of pediatric septic arthritis: a pilot study. J Pediatr Orthop. 2018;38(9):e541-e545.
- Argyris C. Teaching smart people how to learn. Harv Bus Rev. 1991;May-June:99-109.
- Glassman PA, Kravitz RL, Petersen LP, et al. Differences in clinical decision making between internists and cardiologists. Arch Intern Med. 1997;157(5):506-512.
- Accredited Education Institutes ACoS. Available at: http://www.facs.org/education/program/simulation-based.2017.
- Aim F, Lonjon G, Hannouche D, et al. Effectiveness of virtual reality training in orthopaedic surgery. Arthroscopy. 2016;32(1):224-232.
Appendix 1. Team Challenge Scoring Sheet Name:
Neurological Alert: Use of IOMN Alert Checklist
| NB: All participants in Group Receive Same Score | Score |
|---|---|
TEAM SKILLS:
|
/25 |
SUCCESFULLY RUNS THE CHECKLIST, INCLUDING:
|
/15 |
| Identifies salvage techniques | /5 |
| Total | /45 |
Adverse Event Troubleshooting
| NB: All participants in Group Receive Same Score | Score |
|---|---|
TEAM SKILLS:
|
/25 |
| Prepares for flip/CPR | /5 |
| Total | /30 |
Teamwork: Individual Score
| Score | |
|---|---|
| Actively participates in role without dominating | /10 |
| Listens to others and seeks to engage all members | /5 |
| Offers ideas and solutions that enhance performance of task | /5 |
| Uses closed loop communication (use of specific names, directed questions, verbal responses) and double loop feedback (to ask for an action, participant says what they want done and why they feel it should be done that way) | /5 |
| Total | /25 |
Total Score
| Score | |
|---|---|
| Neurologic Alert/Checklist | /45 |
| Adverse Event | /30 |
| Individual Performance | /25 |
| Total | /100 |
