Current Concept Review
Management of Upper Extremity Manifestations of Cerebral Palsy
Boston Children’s Hospital, Boston, MA
Correspondence: Carley Vuillermin, MBBS, MPH, FRACS, Boston Children’s Hospital, 300 Longwood Ave., Hunnewell 2, Boston, MA 02115. E-mail: [email protected]
Received: April 18, 2022; Accepted: April 18, 2022; Published: May 1, 2022
DOI: 10.55275/JPOSNA-2022-0042
Volume 4, Number 2, May 2022
Abstract:
This current concept review serves as an introduction and basis for the evaluation and treatment of upper extremity dysfunction in cerebral palsy. It provides a background on the management of the upper extremity manifestations of cerebral palsy following a 2021 lower extremity tutorial in JPOSNA® on the treatment of gait abnormalities in cerebral palsy. In this review, we will discuss one approach to the classification, assessment, and current management modalities, nonoperative and operative. In successive editions of JPOSNA®, we will present panel discussions of patients with classic presentations and their treatment. Our hope is that upper extremity care will be a parallel consideration for all patients with cerebral palsy.
Key Concepts:
- The upper extremity assessment and management should occur in parallel to lower extremity care in patients with cerebral palsy.
- Many patients with cerebral palsy upper extremity involvement will not require surgical care.
- The use of standardized assessments and careful assessment over time will guide treatment.
- Surgery at one level in the arm will affect the joints distal, particularly for muscles that cross two or more joints. The overall balance must be considered.
Introduction
Upper extremity management in patients with an evolving diagnosis of a neuromuscular disability is often relegated to after the establishment of gait and a lower extremity treatment plan, however, to make the most of early brain development it is best to occur in parallel.
Hands are used in very different ways to our feet. The upper extremity is less constrained. Our hands feel, interact, and manipulate our environment, relying on fine motor skills and a complex series of movements which are highly task specific. The assessment and management of the upper extremity manifestations of cerebral palsy require specific tools. Management within a multidisciplinary team has become the standard care model, and joint decision-making between the patient, family, and all healthcare providers is essential. In many cases, therapy and adaptive modifications are the mainstays of treatment. For a smaller subset of patients, surgical care can be considered. It should not be overlooked that the first things we notice when we meet someone is their face and then hands. As such, the psychological impact of the upper extremity manifestations of cerebral palsy on a patient’s self-esteem and social interactions must be acknowledged.
Classification
Patients with cerebral palsy can be categorized in many ways according to etiology, topology, and motor function. All are important when making decisions, particularly in the upper extremity. The Gross Motor Function Classification System (GMFCS) is the most widely utilized system for the differentiation of abilities and limitations in gross motor function in patients with cerebral palsy.1 Although very helpful to understand a patient’s global functioning level, it does not necessarily reflect how a patient uses their hand. The Manual Ability Classification System (MACS) is also a 5-level system using knowledge of the patient’s actual performance of tasks during daily activities and is upper extremity specific (Figure 1).2 A patient’s MACS may be similar to a patient’s GMFCS classification, but not necessarily. A GMFCS III patient with spastic diplegia may have postural differences in their upper extremities during gait. However, when not ambulating, they may freely use their hands for fine tasks without adaptation being classified as MACS I. Conversely, a GMFCS I level patient with hemiplegia may have relatively spared lower extremity function, although neglects their affected hand, has poor selective motor control, and requires mirroring to achieve any movements and functions at a MACS III level.
Figure 1. MACS Classification Chart (https://www.macs.nu/).

Another commonly used classification is the House (Table 1) or modified House classification.3 The House classification is an 8-level scale but there are less clearly defined transactions between groups than MACS, and the typical vs. maximal use is unspecified. The modified House classification (5-level) is used in the Shriner’s Hospital Upper Extremity Examination (SHUEE).4
Table 1. House Functional Classification of Upper Extremity Function in Patients with CP
| House Functional Classification | ||
|---|---|---|
| Level | Classification | Description |
| 0 | Does not use | Does not use |
| 1 | Poor passive assist | Uses as a stabilizing weight only |
| 2 | Fair passive assist | Can hold onto object placed in hand |
| 3 | Good passive assist | Can hold onto object and stabilize it for use by other hand |
| 4 | Poor active assist | Can actively grasp object and hold it weakly |
| 5 | Fair active assist | Can actively grasp object and stabilize it well |
| 6 | Good active assist | Can actively grasp and then manipulate it against other hand |
| 7 | Spontaneous use, partial | Can perform bimanual activities easily and occasionally uses the hand spontaneously |
| 8 | Spontaneous use, complete | Uses hand completely independently without reference to the other hand |
Assessment
An initial understanding of the etiology of the patient’s movement disorder as well as topography and motor pattern forms the foundation of the assessment of the upper extremity in a patient with cerebral palsy. Additionally, understanding the patient’s developmental stage, capacity, motivation, goals, and expectations requires time and observation. A patient’s tone and engagement will vary. Repeat examinations over time and multiple visits are the best way to determine the most appropriate care. Only once all are aligned, then surgery may be considered.
History
Patient evaluation should include what the patient uses their hands for, what they wish could be different, and does it get in the way. For higher functioning hands, delving into more specific tasks, particularly those that are age appropriate, and directly addressing aesthetics is essential. The need to use mirroring will help determine the independence of the limb. Mirroring is where the patient needs to perform identical movements of their less affected limb whilst trying to complete a movement with their affected side to assist with achieving the desired movement, for example opening and closing the hand. A limb that needs to mirror to move tends to be less independent. Mirroring combined with selective motor control allows expectation setting around independent function.
For those with more global involvement, it is important to consider function as a family and care unit. Taking away a small function may have a greater effect. Hooking to carry or using a switch may be finely balanced. Hooking is where a patient uses their contracted body part passively to hook. This may be to carry a bag on the forearm or to reach around a caregiver to assist with standing. At times, the function needed may be for the family and caregivers with dressing, hygiene, and preventing skin maceration and breakdown. For example, a lack of shoulder abduction makes dressing and armpit hygiene difficult.
A history of prior interventions and success or failure is also critical. Prescribing one more brace to sit on the shelf is not going to help. The use and effect of Botulinum toxin is also very helpful to ascertain. A patient with high dynamic tone will tend to have a better response to Botulinum toxin than a patient with fixed contractures will not. It is also important to know if the patient has Botulinum toxin injections to the upper extremity and when they were last performed. Assessment with and particularly without the effect is important.
Physical Examination
Examination starts with meeting the patient. Having them walk and run are familiar tasks and provide an assessment of upper extremity posturing during gait or documenting the seated posture for wheelchair ambulators. Holding the patient’s hand can help to detect dystonia and give a sense of tone.
Range of motion needs to be tested both actively and passively. Sometimes motion may only be uncovered by asking the patient to perform a task. Active motion demonstrates selective motor control and will be affected by high tone. At times, active motion can be demonstrated with the request to perform a task even if not able to isolate a single movement. For example, asking a patient to supinate may be less successful than asking them to touch their contralateral ear or receive coins into their palm. Families can assist with observed versus maximal range of motion clarification where persistent tone is suspected. Passive range of motion is assessed as the total motion at the end of a prolonged gentle stretch. A lack of passive range of motion indicates contracture or persistent tone. Tone can be graded with either the modified Ashworth5 (Table 2) or Tardieu scales. It is important to differentiate between contracture and spasticity with a slow gradual stretch.
Table 2. Modified Ashworth Scale for the Quantification of Tone
| Modified Ashworth Scale | |
|---|---|
| 0 | No increased tone |
| 1 | Slight increase in muscle tone - catch and release |
| 1+ | Slight increase in muscle tone - catch and minimal resistance |
| 2 | Increase in tone through most of range but the part is easily moved |
| 3 | Considerable increase in tone, passive movement is difficult |
| 4 | Affected part is in rigid flexion or extension |
Assessment should include the shoulder, elbow, forearm, wrist and hand as they form an interdependent chain. Due to the interdependence of finger and wrist extension, it is important to specifically focus on these movements, including grasp and release. Testing passive wrist extension whilst allowing the finger to flexion, gives an assessment of the wrist flexion contracture. Extending the fingers to neutral at the metacarpophalangeal (MCP) and interphalangeal (IP) joints and then remeasuring wrist extension gives a composite measure of wrist extension (defined as Eaton’s angle) with a discrepancy indicating finger flexor tightness. Grasp and release is tested with the wrist flexed, neutral and extended, including the ability to actively open the fingers and the need to use wrist flexion tenodesis for release.
Within the hand itself, it is important to assess the thumb, first web space, and digits for intrinsic spasticity. Thumb posture and instability at either the IP or MCP is classified by the House classification of the thumb (Table 3). Each component of the thumb posture and function is important for decision-making. Intrinsic tightness of the other digits is assessed with the MCP joints flexed and then flexing the PIP joint. Tightness indicates spasticity if rate dependent or contracture if fixed.
Table 3. House Thumb-in-Palm Classification
| House Thumb-in-Palm Classification | |
|---|---|
| Type | Description |
| I | Metacarpal adduction contracture |
| II | Metacarpal adduction and MCP flexion deformity |
| III | Metacarpal adduction and MCP hyperextension or instability |
| IV | Metacarpal adduction with MCP and IP flexion deformity |
Finally, in higher functioning limbs, looking at the size of the limb comparted to the contralateral side and performing either stereognosis or 2-point discrimination, although not correlated with outcomes, is very helpful for patient and family understanding of the impairment. This can be done with simple items found in the office, including a pen lid, quarter, and paperclip.
Nonorthopaedic Surgical Interventions
Management of the upper extremity in CP can be broadly divided into increasing the hand-brain connection, preventing or treating contracture, and increasing functional use. The patient and family goals are very important.
Stretching
Patients with abnormal tone posture with their joints in altered alignment, the typical posture is thumb in palm, wrist flexion and ulnar deviation, forearm pronation, elbow flexion and shoulder adduction with internal rotation. Taking joints through a full range of motion and undertaking end range of motion stretching helps to prevent contracture development and increases total range of motion.
Splinting
Splinting can be used for two main purposes: to provide a prolonged stretch or to position the limb for better function. Splints that are more conforming provide better support and containment than off-the-shelf splints with metal stays or material slings. The more specific a splint order, the more likely the patient will receive a splint with the purpose it was prescribed.
Splinting for function is usually aimed at the position of the wrist and thumb. The degree of constraint will depend on the patient’s spasticity, joint stability, and resting position. Dynamic (DMO) splints for daytime use are made from conforming nylon with panels and stitching to support joints and counter spasticity. Static splints may contain either thermoplastic or metal stays to provide a greater level of support. In general, thermoplastic components are more comfortable for patients and, with tone, are less likely to experience escape than when metal supports are used.
Splints for stretching are used during periods of low activity, most commonly at night, and are more constraining than daytime splints. When not tolerated at night, other time points may be selected, such as in the morning and during the commute to school. Stretching splints are commonly static but may be dynamic and focus on stretching a particular joint or group of joints. The more functions you are asking a splint to perform, there is a risk of being less effective and tolerance may decrease. Dynamic splints in spasticity can take a longer period to wean into and require more initial modification. With use, dynamic splints adjust to changes in joint range of motion. Static splints do not, and therefore, need more frequent periodic reassessment, although often with earlier tolerance. Frequent planned adjustments to static splints with the goal of increasing joint range of motion is static progressive splinting.
Serial casting is the purposeful application of casts on a weekly or every-other-week basis to provide a prolonged gentle stretch and increase joint range of motion. The evidence for the efficacy of serial casting is low.6 Prior to the institution of a serial casting, the goals of casting should be determined. The post-casting splint regime has to be established, otherwise gains made will be rapidly lost and contractures recur. Serial casts are applied by experienced practitioners after in-clinic stretching by a therapist. In the upper extremity, soft cast material can be used rather than fiberglass to reduce skin-related complications and the need for cast removal with a saw. Combining Botulinum toxin injections with the commencement of serial casting can assist with tone and pain management, a so called window of opportunity.
Occupational Therapy
Occupational therapy (OT) aims to maximize the patient’s ability to complete activities of daily living. There is evidence of cortical reorganization in hemiplegic cerebral palsy.7 Many occupational therapy interventions aim to increase executive cortical function and selective motor control. School occupational therapy tends to focus on tasks needed to be successful in the classroom and learning environment. Patients who receive school therapy may still benefit from outside therapy for attainment of skills not directly related to their educational environment.
Occupational therapists also provide standardized assessments. There are many assessment tools available, some are specific to CP and others applied more widely. The Canadian Occupational Performance Measure (COPM) can be a very useful tool for objectively documenting treatment results, but it is not CP specific.8 For setting goals in CP, there are many measurement instruments. Most require a skilled OT to administer and score; however, some have specific training requirements or a licensing fee to use. Examples of CP specific assessments include the AHA9 and SHUEE.4
The SHUEE is a validated video-based evaluation (Figure 2) developed to be a standardized assessment of the hemiplegic upper extremity and help direct intervention. There are two main sections: 1) Active and Passive Range of Motion/modified Ashworth scale and 2) Functional analysis, broken down into spontaneous functional analysis (SFA), dynamic positional analysis (DFA), and Grasp and Release. SFA utilizes a modified House functional classification (Table 4) assessed during nine tasks, and DPA assesses segmental alignment during a series of 16 prescribed tasks. It is videoed and scored. Administration takes approximately 15–30 minutes. Scoring allows comparison between studies performed on the same subject over time, such as before and after an intervention. Individual component assessment provides guidance on selection of a surgical prescription.4
Figure 2. A patient undertaking SHUEE examination pre- (A) and post- (B) multilevel tendon transfers for rebalancing in upper extremity CP. In this case, an elbow flexor lengthening, pronator teres rerouting, forearm fractional lengthenings, 1st web space 4 flap Z-plasty, adductor release, thumb MCP sesamoidesis, and EPL rerouting. Clinical photograph courtesy of Carley Vuillermin, MBBS, MPH, FRACS, © Children’s Orthopaedic Surgery Foundation.
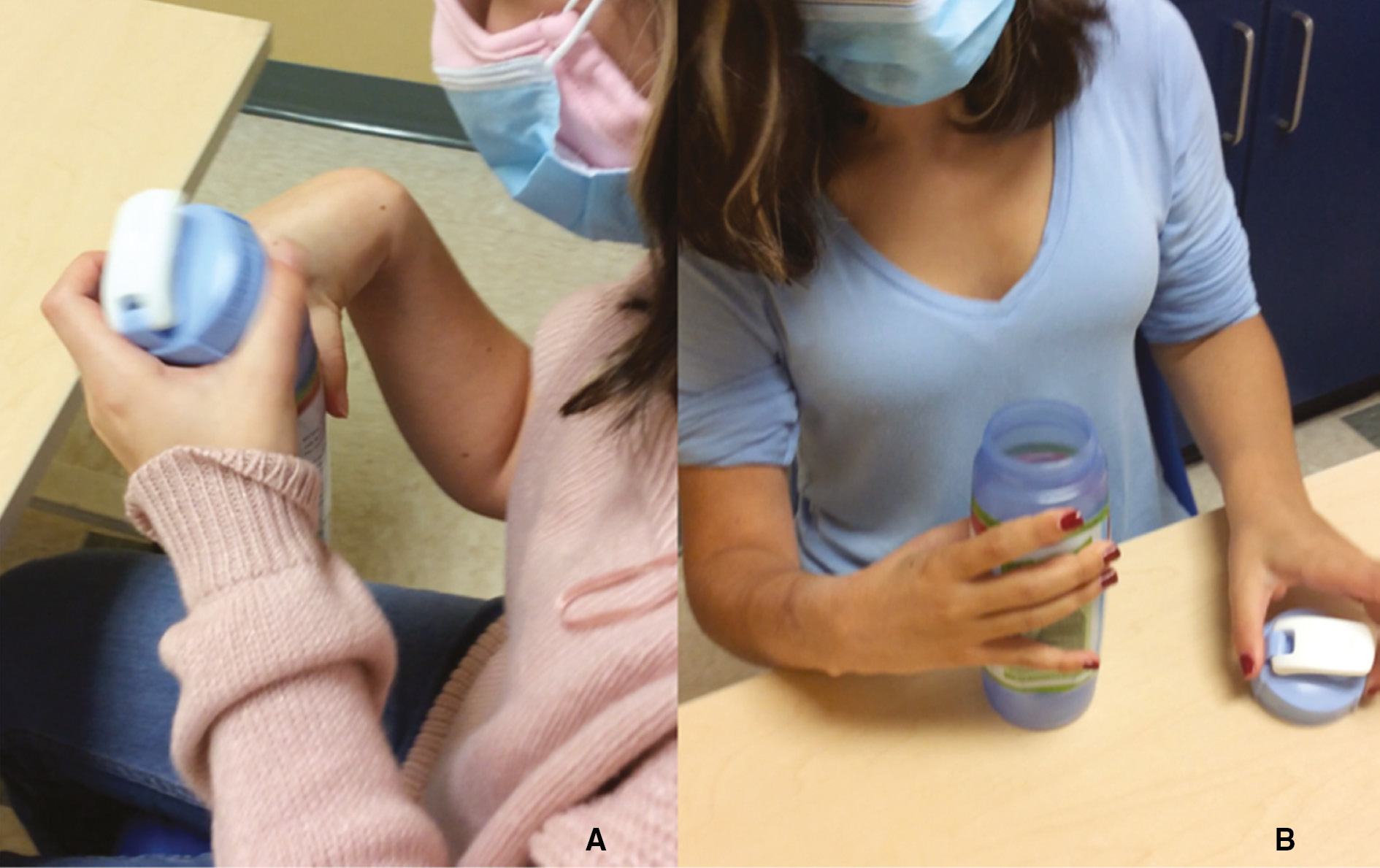
Table 4. Modified House Functional Classification as Used in the SHUEE Examination
| Modified House Functional Classification | |
|---|---|
| Level | |
| 0 | Complete neglect |
| 1 | Poor passive assist, stabilizing weight |
| 2 | Passive assist, hold object placed into hand |
| 3 | Poor active assist, grasp and hold weakly |
| 4 | Active assist, grasp and stabilize well |
| 5 | Spontaneous, independent function |
Constraint therapy is a treatment modality within occupational therapy. It is aimed at increasing the patients affected side hand use and is a purposeful period of intense therapy. There are many different constraint programs. All immobilize the unaffected arm, including the digits, and vary in number of therapy sessions per week from two to daily. One commonly undertaken regime is a 6-week program with 3 weeks of constraint followed by 3 weeks of bimanual training. During this period, the patient works with their therapist and at home on specific tasks. Many centers offer these programs as camps over the summer. There is some evidence for constraint improving unimanual capacity; however, children may find constraint frustrating and, in this situation, benefit from a bimanual program instead.10
Tone Management
Tone management is commonly undertaken in conjunction with physiatry or neurology colleagues. Management of tone can be systemic, intrathecal, or localized. Oral and intrathecal baclofen form the mainstays of medical treatment. Other agents are also used but less commonly. Botulinum toxin injections provide selective temporary tone management. Botulinum toxin use in the upper extremity may be limited by dose available, particularly in lower-weight patients needing lower extremity injections.
When Botulinum toxin is used in more highly functioning limbs, it is important to undertake occupational therapy to strengthen the antagonist groups starting 1–2 weeks after the injections. Commonly injected targets include pronator teres, wrist and finger flexors, thenar, and small intrinsic hand musculature. Strengthening programs therefore focus on supination, wrist, finger, and thumb extension. By strengthening the antagonist groups, the positional gains from the injections may be retained after the pharmacologic effects wear off. Botulinum toxin has been shown to be better than therapy alone.11 Botulinum toxin can also assist with tone management in the perioperative period and prior to serial casting.
In the lower extremity, selective dorsal rhizotomy is used in patients with generalized high tone. Although possible in the cervical spine, it is much harder and higher risk. For this reason, it is not commonly considered. Hyperselective neurectomy is a newer surgical treatment where the terminal branches of the peripheral nerves are selectively sectioned by cutting at least 2/3 of the terminal branches. By doing this, the afferent reflexes are decreased, and the motor nerves are believed to undergo terminal regeneration. When this is performed, a period of weakness is expected. Hyperselective neurectomy has been utilized for elbow and wrist spasticity. Due to the extensive dissection that would be required for the finger flexors, these muscles are not considered suitable targets for hyperselective neurectomy and are recommended to still be treated with musculotendinous lengthening.12,13
Orthopaedic Surgical intervention
Many patients will not seek or need surgical management of their upper extremity. Some patients and limbs are not suitable for a surgical approach, particularly those with predominant dystonia. Surgical interventions can be broken into two broad categories: those aimed at releasing and stabilizing joints for dressing, hygiene, and posture and those for stabilizing and rebalancing to improve function. It is important the goals are set and known preoperatively. Active involvement of a multidisciplinary team is essential. Patients must have skilled occupational therapy postoperatively to yield the benefit.
Procedures to Stabilize and Rebalance and to Improve Function
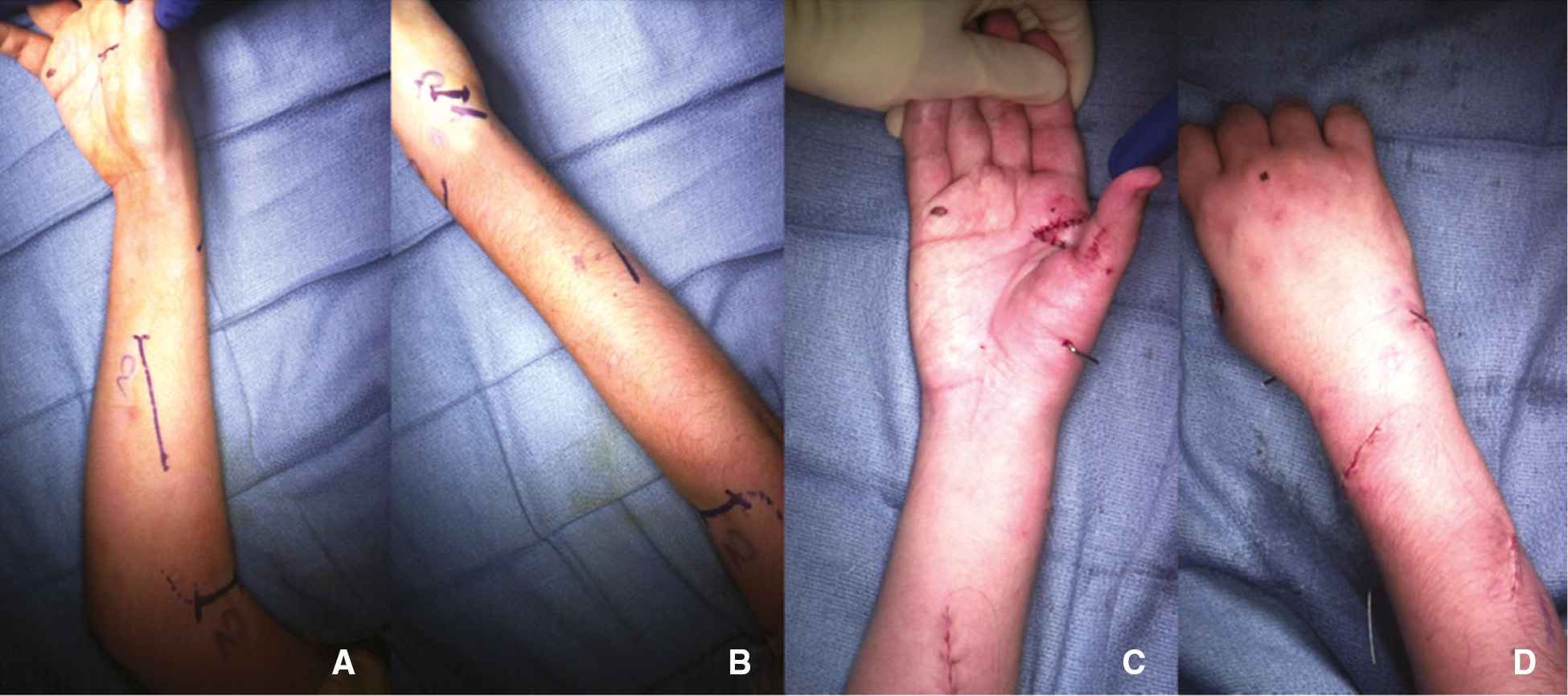
The current surgical management of the upper extremity in CP is also considered a single-event multilevel surgery (SEMLS) approach, and in well-selected patients it offers superior function to Botulinum toxin and therapy.14,15 When undertaking SEMLS, it is important to plan and mark out all incisions prior to the commencement of surgery, as tourniquet time can be a limiting factor (Figure 3). A combination of procedures is usually indicated; however, isolated procedures are sometimes indicated just as in the lower extremity. This is commonly to address hygiene-related concerns.
Figure 3. Marking of all incisions prior to insufflation of the tourniquet (A&B), sew as you go closure of wounds sequentially with tendon transfers being tensioned nearing final closure (C&D). This patient underwent ECU to ECRL transfer, 1st web space 4 flap Z-plasty, adductor contracture release, thumb MCP stabilization, pronator rerouting in a single 2-hour tourniquet time. Clinical photograph courtesy of Carley Vuillermin, MBBS, MPH, FRACS, © Children’s Orthopaedic Surgery Foundation.
Surgery at one level in the arm will affect the joints distal, particularly for muscles that cross two or more joints. The overall balance must be considered. An elbow release without a flexor pronator slide or forearm tendon lengthening will increase a wrist flexion contracture just as increasing wrist extension will exacerbate finger flexor tightness.
Tendon transfer principles need to be followed; however, by its nature, CP does not offer an ideal environment for tendon transfers. Where possible, the tendon transfer should have a subcutaneous route with a free straight line of pull. There must be sufficient excursion of adjacent musculotendinous units and skin to allow rebalancing procedures to function. For example, mobilizing the FCU along 2/3 of its ulna attachment leads to a straighter line of pull than only mobilizing 1/3 off of the ulna. A straighter pull also increases the supination moment.16
The better the selective motor control (phasic activation), the better the transfer will function. Ideally, a transfer is synergistic and needs to be considered differently in limbs with spasticity; muscles may not fire in their typical phase. A Flexor Carpi Ulnaris (FCU) that fires out of phase is an ideal wrist extension candidate. If the FCU is tonically active, then this muscle is not a good candidate for transfer, as it risks overcorrection. In this situation, Extensor Carpi Ulnaris (ECU) may be a better candidate for transfer for wrist extension. If uncertain on clinical examination, motion lab EMG can be utilized to determine phasic or continuous activity. It has been shown the FCU does not change phase after transfer.17 When the forearm is pronated, ECU is an ulna deviator and can become a wrist flexor. The ECU can become an isolated wrist extensor by transferring it across to Extensor Carpi Radialis Longus (ECRL) or Extensor Carpi Radialis Brevis (ECRB).
Tendon transfers can yield both primary and secondary effects. An FCU transfer around the ulna border for wrist extension also adds a supination moment.16 This needs to be considered if also doing a pronator rerouting. An Extensor Pollicis Longus (EPL) rerouting will increase thumb metacarpal palmer abduction; however, it may result in metacarpalphalngeal (MCP) or interphalangeal (IP) hyperextension if joint instability is present or if there is insufficient 1st web space mobility.
Considering the surgical management by anatomic level in functional limbs, it is important to plan the surgical components individually and their interplay with each other. Setting the surgical plan from proximal to distal and completing tendon transfers after joint stabilizations and fusions. It is the location of the joints, not the muscle, which determines this order. Releases may come before or after joint stabilizations; however, tendon transfers are best completed last to ensure proper balance and protection until casted. Although a typical pattern includes elbow flexion, forearm pronation, wrist flexion with ulna deviation, and thumb-in-palm deformity, many patients are not typical, and the degree of involvement most certainly varies. Lower or non-functional limbs more often display atypical patterns. Surgical selection should bear this in mind.
Shoulder Surgery
It is not common to need surgical care of the functional shoulder in a patient with hemiplegic cerebral palsy. If spasticity/posturing or contracture are problematic, then fractional lengthenings are preferred. However, in the less functional upper extremity, a complete release of the pectoralis major tendon is an excellent intervention and offers significant improvements in personal care.
Elbow Surgery
Dynamic elbow flexion posturing can be managed with fractional lengthening of the biceps and brachialis (Figure 4). Mild contractures (<45 degrees) can also be managed this way; however, more significant contractures may require a Z-lengthening of the biceps and a myotomy of the brachialis and possibly an elbow capsular release.18,19 The greater the surgical dose, the more likely to create weakness. Procedures on the elbow may at least temporarily reduce spasticity, as surgical exposure around tendons decreases their afferent stretch reflexes. Be careful performing elbow releases in upper extremities with external rotation posturing at rest. This can lead to limb excursions outside of the patient’s personal space and catching on doorways and the like.
Figure 4. Antecubital fossa exposure for biceps Z-lengthening (A) and brachialis fractional lengthening (B). Clinical photograph courtesy of Carley Vuillermin, MBBS, MPH, FRACS, © Children’s Orthopaedic Surgery Foundation.

Forearm Surgery
When considering the forearm segment, the active and passive range of supination helps with surgical decision-making.20 For more functional limbs with a discrepancy between active and passive supination, a pronator teres rerouting is the preferred treatment (Figure 5), whereas with lower functioning limbs, a pronator release could be considered.21 When releasing the pronator, it can be performed proximally as part of a flexor pronator slide22 or distally from the midshaft of the radius. Some patients with seated function only do not utilize supination, and the pronator may not need to be specifically addressed. Forearms that have active supination or sit in a supinated position should not have a release due to the risk of developing a hypersupination deformity.
Figure 5. Pronator teres rerouting. Pronator teres exposure along the middle 1/3 of the radius (A), mobilization (B), and rerouting 360 degrees with securing via drill holes and nonabsorbable suture back to the pronator footprint. Clinical photograph courtesy of Kenneth Noonan, MD.
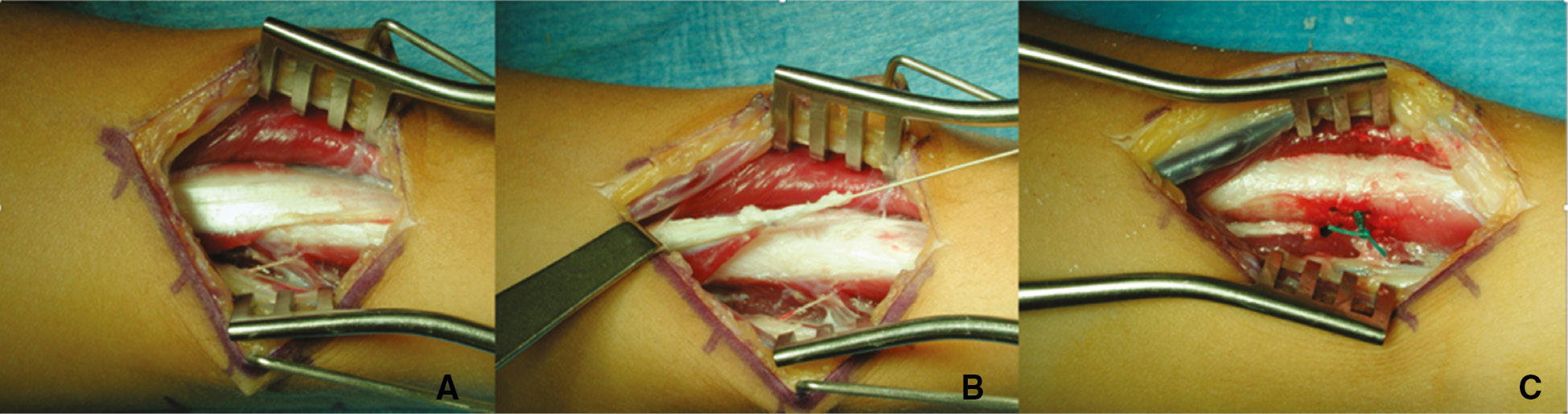
Figure 6. FCU mobilization for transfer. Note the musculotendinous unit inserts along the ulna shaft and as shown in this clinical photograph, needs to be mobilized for effective transfer. Also depicted, intramuscular FDS lengthenings. Clinical photograph courtesy of Kenneth Noonan, MD.

Wrist and Finger Surgery
The most common tendon transfer for wrist extension has been FCU transferred around the ulna border (Green transfer); however, late deformities may occur.23 The ECU is also a good candidate to provide wrist extension, particularly when there is tonic FCU activity. The ECU or FCU transfer is taken to either the ECRL or ECRB depending on the degree of ulna deviation. ECRL has a more radial insertion. Tension is aimed to be at or just above neutral.
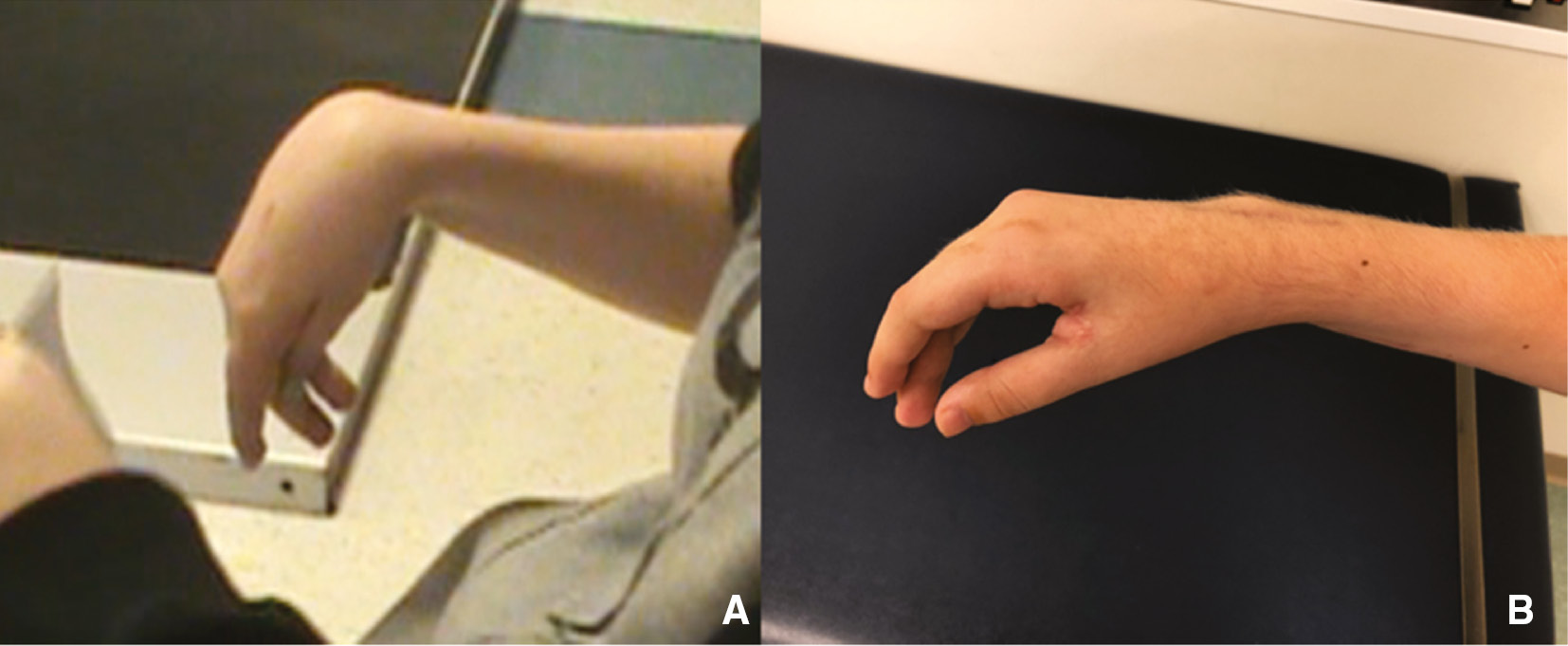
For wrists with severe contracture or poor control, a wrist fusion, most commonly with proximal row carpectomy, can give an excellent functional hand position (Figure 7).24 You must be very careful in patients who rely on tenodesis for grasp and release function not to perform a wrist fusion or understand this function will be taken away. A rigid wrist splint can mimic a wrist fusion; however, it is difficult to mimic the final balance. A skilled therapist or experienced upper extremity CP surgeon may be able to unpackage the need for tenodesis in grasp and release.
Figure 7. Patient pre- (A) and post- (B) wrist fusion, 1st web space release with 4 flap Z-plasty and EPL rerouting. Clinical photograph courtesy of Carley Vuillermin, MBBS, MPH, FRACS, © Children’s Orthopaedic Surgery Foundation.
As previously discussed, the finger balance is intrinsically linked to wrist position. Finger balance should be determined with the wrist in the anticipated functional position. If a wrist fusion is to be performed, the digit rebalancing occurs after wrist fusion. Where multiple levels are being addressed, the setting of tendon transfers should occur from proximal to distal. Non-transferred wrist flexors may need fractional lengthening, Z-lengthening, or in the case of a wrist fusion, tenotomy.
When working to achieve digit balance, the options are fractional lengthening, flexor pronator slide, Z-lengthenings and superficialis-to-profundus transfer (STP). Fractional lengthening with either one or occasionally two intramuscular tenotomies allows the most gentle and functional lengthening of the digits. The location of the musculotendinous junction is highly variable.25 Avoiding more than 1-1.5 cm of lengthening and preserving the muscle tendon continuity is essential for function. Stretching of the digits should monitor this and not extend above neutral. The flexor pronator slide is powerful and used for lower functioning limbs. It is a technically demanding release which moves the entire flexor pronator origin distal whilst preserving all neurovascular structures.22 The superficialis-to-profundus transfer is a very powerful lengthening; however, the uncovering of intrinsic spasticity commonly results in an unsightly hand, and the author has tended not to use this procedure in patients with cerebral palsy. It continues to hold its place for some surgeons, particularly in stroke care.
Surgery for Thumb-in-Palm-Deformity
The thumb is probably the hardest to achieve balance and function. Even experienced surgeons face undercorrection and deterioration.26,27 The thumb is commonly addressed late in an extensive surgical procedure and has many factors at play. The common deformity is a spastic thumb adductor with 1st metacarpal adduction, metacarpal flexion deformity, or extension instability, and the EPL of the adducted thumb no longer effectively extends the MCP joint. Each component needs to be addressed. If the metacarpal adduction has led to a contracture of the first webspace, then a Z-plasty may be performed. This may be a 2 flap or 4 flap Z-plasty (Figure 8). The 2 flap Z-plasty is faster; however, and it gives a less gradual contour to the web. The adductor can either be lengthened at its insertion into the base of the proximal phalanx at the MCP through the 1st web space deepening approach or via a palmer incision off the 3rd metacarpal. Instability of the MCP should be addressed. Capsulodesis procedures will stretch out over time; therefore, either a fusion or sesamoidesis is favored.
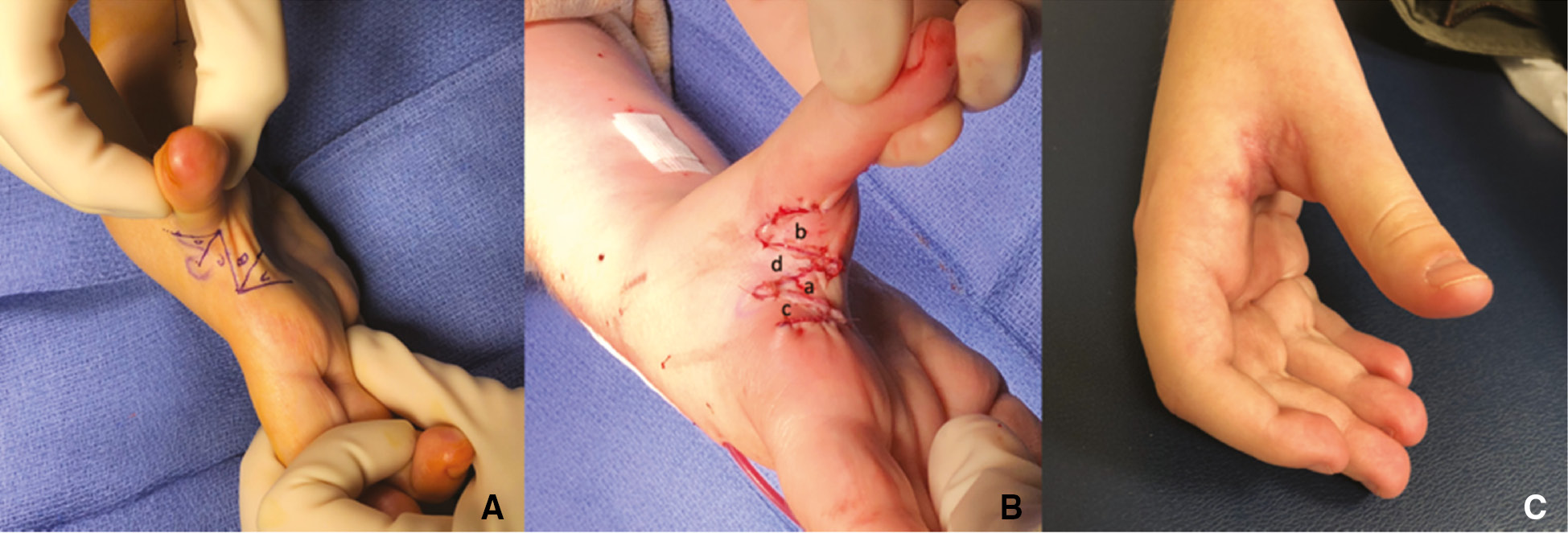
Figure 8. Presurgical markings for 4 flap Z-plasty, initial flaps a,b,c,d (A), rotate and inset to c,a,d,b (B), surgical outcome at 6 months (C). Clinical photograph courtesy of Carley Vuillermin, MBBS, MPH, FRACS, © Children’s Orthopaedic Surgery Foundation.
Finally, the thumb extrinsics, EPL and FPL, are addressed. FPL is commonly lengthened via a Z-lengthening in the forearm and the EPL to restore its function as an extensor and abductor, rerouted through the 1st dorsal compartment. The EPL tendon may be either divided distally or at the dorsal wrist. It is not uncommon once rerouted to excise a centimeter for balance prior to repairing it.
Summary
Management of the upper extremity in patients with cerebral palsy requires deliberate assessment and preoperative planning. The success of surgery is highly dependent on preoperative goals and postoperative rehabilitation. This article has not described individual surgical techniques. However, it aims to review the current concepts in this field, including non-surgical modalities, and allows the surgeon to tailor treatment to their patient. In future editions of JPOSNA®, we will use this framework and expand upon the clinical decision-making with a case-based tutorial.
Additional Links
- The Manual Ability Classification System (MACS)—https://www.macs.nu/, https://www.macs.nu/youtube.php
- The Canadian Occupational Performance Measure (COPM)—https://www.thecopm.ca/
- Assisting Hand Assessment (AHA) website—http://www.ahanetwork.se/
Disclaimer
The author has no conflicts of interest to disclose.
References
- Palisano RJ, Rosenbaum P, Bartlett D, et al. Content validity of the expanded and revised Gross Motor Function Classification System. Dev Med Child Neurol. 2008;50(10):744–750.
- Eliasson AC, Krumlinde-Sundholm L, Rösblad B, et al. The Manual Ability Classification System (MACS) for children with cerebral palsy: scale development and evidence of validity and reliability. Dev Med Child Neurol. 2006;48(7):549-554.
- House JH, Gwathmey FW, Fidler MO. A dynamic approach to the thumb-in palm deformity in cerebral palsy. J Bone Joint Surg Am. 1981;63(2):216-225.
- Davids JR, Peace LC, Wagner LV, et al. Validation of the Shriners Hospital for Children Upper Extremity Evaluation (SHUEE) for children with hemiplegic cerebral palsy. J Bone Joint Surg Am. 2006;88(2):326-333.
- Bohannon RW, Smith MB. Interrater reliability of a modified Ashworth scale of muscle spasticity. Phys Ther. 1987;67(2):206-207.
- Lannin NA, Novak I, Cusick A. A systematic review of upper extremity casting for children and adults with central nervous system motor disorders. Clin Rehabil. 2007;21(11):963-976.
- Papadelis C, Butler EE, Rubenstein M, et al. Reorganization of the somatosensory cortex in hemiplegic cerebral palsy associated with impaired sensory tracts. Neuroimage Clin. 2017;17:198-212.
- The Canadian Occupational Performance Measure. Available at: http://www.thecopm.ca. Accessed April 10, 2022.
- Krumlinde-Sundholm L, Holmefur M, Kottorp A, et al. The Assisting Hand Assessment: current evidence of validity, reliability, and responsiveness to change. Dev Med Child Neurol. 2007;49(4):259-264.
- Hoare BJ, Wallen MA, Thorley MN, et al. Constraint-induced movement therapy in children with unilateral cerebral palsy. Cochrane Database Syst Rev. 2019;4(4):CD004149.
- Fehlings D, Rang M, Glazier J, et al. An evaluation of botulinum-A toxin injections to improve upper extremity function in children with hemiplegic cerebral palsy. J Pediatr. 2000;137(3):331-337.
- Gras M, Leclercq C. Spasticity and hyperselective neurectomy in the upper limb. Hand Surg Rehabil. 2017;36(6):391-401.
- Leclercq C, Perruisseau-Carrier A, Gras M, et al. Hyperselective neurectomy for the treatment of upper limb spasticity in adults and children: a prospective study. J Hand Surg Eur Vol. 2021;46(7):708-716.
- Smitherman JA, Davids JR, Tanner S, et al. Functional outcomes following single-event multilevel surgery of the upper extremity for children with hemiplegic cerebral palsy. J Bone Joint Surg Am. 2011;93(7):655-661.
- Van Heest AE, Bagley A, Molitor F, et al. Tendon transfer surgery in upper-extremity cerebral palsy is more effective than botulinum toxin injections or regular, ongoing therapy. J Bone Joint Surg Am. 2015;97(7):529-536.
- Van Heest A, Stout J, Wervey R, et al. Follow-up motion laboratory analysis for patients with spastic hemiplegia due to cerebral palsy: analysis of the flexor carpi ulnaris firing pattern before and after tendon transfer surgery. J Hand Surg Am. 2010;35(2):284-290.
- Van Heest AE, Murthy NS, Sathy MR, et al. The supination effect of tendon transfer of the flexor carpi ulnaris to the extensor carpi radialis brevis or longus: a cadaveric study. J Hand Surg Am. 1999;24(5):1091-1096.
- Carlson MG, Hearns KA, Inkellis E, et al. Early results of surgical intervention for elbow deformity in cerebral palsy based on degree of contracture. J Hand Surg Am. 2012;37(8):1665-1671.
- Dy CJ, Pean CA, Hearns KA, et al. Long-term results following surgical treatment of elbow deformity in patients with cerebral palsy. J Hand Surg Am. 2013;38(12):2432-2436.
- Gschwind C, Tonkin M. Surgery for cerebral palsy: Part 1. Classification and operative procedures for pronation deformity. J Hand Surg Br. 1992;17(4):391-395.
- Strecker WB, Emanuel JP, Dailey L, et al. Comparison of pronator tenotomy and pronator rerouting in children with spastic cerebral palsy. J Hand Surg Am. 1988;13(4):540-543.
- Thevenin-Lemoine C, Denormandie P, Schnitzler A, et al. Flexor origin slide for contracture of spastic finger flexor muscles: a retrospective study. J Bone Joint Surg Am. 2013;95(5):446-453.
- Patterson JM, Wang AA, Hutchinson DT. Late deformities following the transfer of the flexor carpi ulnaris to the extensor carpi radialis brevis in children with cerebral palsy. J Hand Surg Am. 2010;35(11):1774-1778.
- Van Heest AE, Strothman D. Wrist arthrodesis in cerebral palsy. J Hand Surg Am. 2009;34(7):1216-1224.
- Arnaout A, Leclercq C. Fractional lengthening of the forearm flexor muscles: anatomic study. J Hand Surg Am. 2021;3:S0363-5023(21)00444-5.
- Davids JR, Sabesan VJ, Ortmann F, et al. Surgical management of thumb deformity in children with hemiplegic-type cerebral palsy. J Pediatr Orthop. 2009;29(5):504-510.
- Alewijnse JV, Smeulders MJ, Kreulen M. Short-term and long-term clinical results of the surgical correction of thumb-in-palm deformity in patients with cerebral palsy. J Pediatr Orthop. 2015;35(8):825-830.
