Current Concept Review
Biomechanical Basis for Treatment of Pediatric Foot Deformities Part II: Pathomechanics of Common Foot Deformities
1Bloomberg Children’s Center, Johns Hopkins Hospital, Kennedy Krieger Institute, Baltimore, MD; 2Department of Pediatric Orthopaedics, Massachusetts General Hospital, Boston, MA; 3Department of Paediatric Orthopaedics, Kasturba Medical College, Manipal, India
Correspondence: Benjamin Joseph, MCh Orth, FRCS Ed, 18 HIG, HUDCO Colony, Manipal, 576104, Karnataka, India. E-mail: [email protected].in
Received: March 15, 2022; Accepted: March 20, 2022; Published: May 1, 2022
DOI: 10.55275/JPOSNA-2022-0038
Volume 4, Number 2, May 2022
Abstract:
The biomechanical basis for causation and treatment of pes planus, convex pes valgus (vertical talus), pes cavus, paralytic deformities, and foot deformities in cerebral palsy are presented. In each instance, the altered alignment of the hindfoot and forefoot, the configuration of the medial longitudinal arch and the instability of the talonavicular joint differ. The patterns of muscle imbalance across the axes of movement in paralytic deformities and the concept of treatment aimed at muscle rebalancing across these axes are graphically illustrated. The common deformities of the foot encountered in cerebral palsy are described and, in particular, the different deformity patterns resulting from spasticity of the gastrocnemius. The importance of preserving the function of the soleus and avoiding over-lengthening of the gastroc-soleus is emphasized.
Key Concept:
- Common deformities of the foot are complex and have deformity components involving the hindfoot, the forefoot, the longitudinal arch, the talonavicular joint and the alignment of the talus.
PES PLANUS (FLATFOOT)
Pes planus or pes planovalgus is characterized by loss of the medial longitudinal arch, hindfoot valgus, and forefoot abduction (Figure 1).
Figure 1. Pes planus of the right foot in an adolescent following isolated paralysis of the tibialis posterior muscle due to poliomyelitis. The hindfoot valgus (A) and the forefoot abduction are evident (B, C).

Factors that Contribute to Collapse of the Arch
Body Weight
The frequency of flatfoot increases as the Body Mass Index (BMI) increases.1
Extrinsic Muscles
Contractures of muscles attached to either end of the arch (tibialis anterior and the gastrocnemius-soleus) can flatten the arch (Figure 2). In clinical practice, a contracted gastrocnemius-soleus muscle is frequently encountered in children with flatfeet but may be overlooked unless passive dorsiflexion of the ankle is tested with the knee extended and the foot in inversion (Figure 3).
If the gastrocnemius-soleus is short, the hindfoot rolls into valgus and the arch collapses. Compensatory hindfoot valgus helps avoid an equinus posture and enables the heel to rest on the ground. This reduces the lever arm of the gastrocnemius-soleus with weakness of push-off and a typical flatfooted gait (Figure 4).
Figure 2. The effects of abnormalities of extrinsic muscles on the medial longitudinal arch.
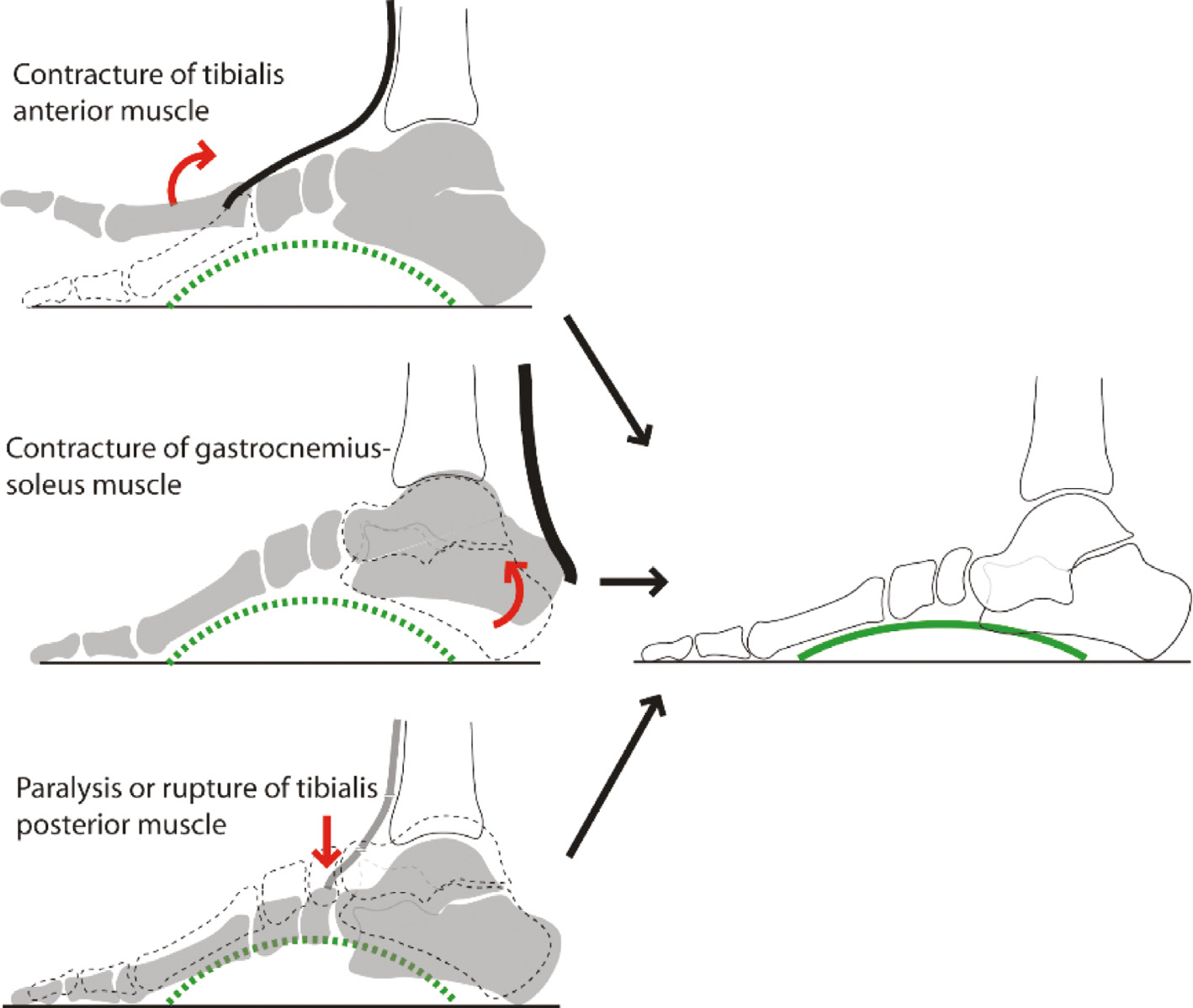
Figure 3. Technique of testing for contracture of the gastrocnemius-soleus with the knee extended and foot inverted.

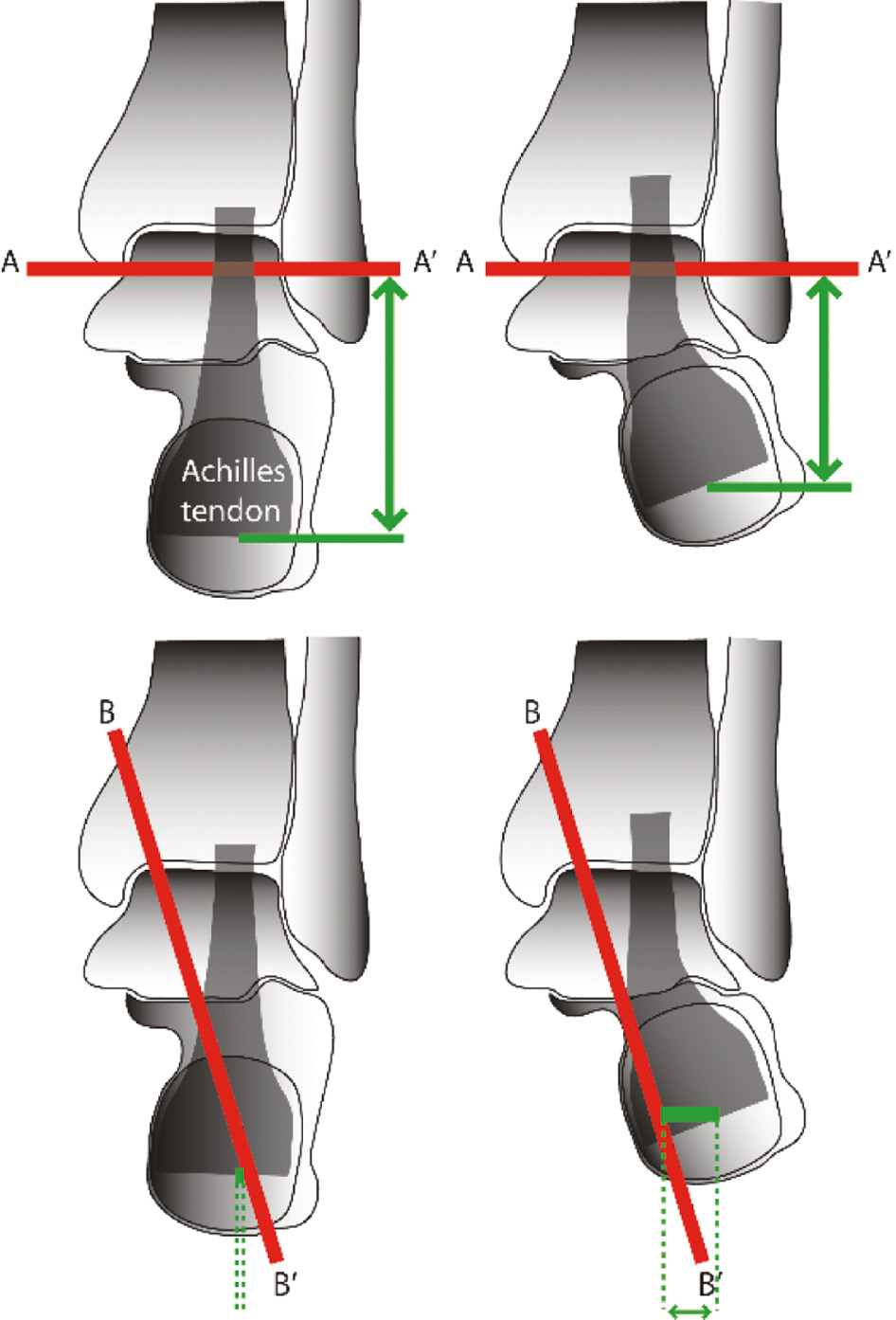
Figure 4. A short gastrocnemius-soleus leads to a valgus hindfoot and short lever arm of the muscle between the axis of the ankle joint (AA’) and the insertion of the Achilles tendon (green double arrow top right). The valgus moment of the muscle across the subtalar axis (BB’) is also increased (bottom right).
Active contraction of the tibialis posterior accentuates the arch and the arch collapses when the tibialis posterior is paralyzed (Figures 1 and 2).
Ligaments of the Foot
Flatfeet are common in syndromes with generalized ligament laxity. The plantar calcaneonavicular or spring ligament, stretching from the sustentaculum tali on the calcaneum to the navicular, is crucial in maintaining the arch. It forms an integral part of the acetabulum pedis and supports the head of the talus while weight-bearing. The support of the head of the talus by the spring ligament may be lost when the hindfoot is in valgus (Figure 5), and if the forefoot is abducted, the talus will then lie in complete plantarflexion (Figure 6).
Figure 5. The normal relationship of the tarsal bones viewed from the sole (left). A major portion of the head of the talus (dark orange) is not visualized, as it is resting on the plantar calcaneonavicular ligament (spring ligament) shown in green. When the hindfoot is in valgus, the calcaneo-pedal unit (CPU) abducts (black arrow middle figure). The spring ligament moves laterally along with the CPU, exposing the head of the talus (yellow arrow). In addition, if there is an abduction deformity of the forefoot (black arrow right), the greater part of the head of the talus is exposed and the support of the head of the talus by the spring ligament becomes tenuous.
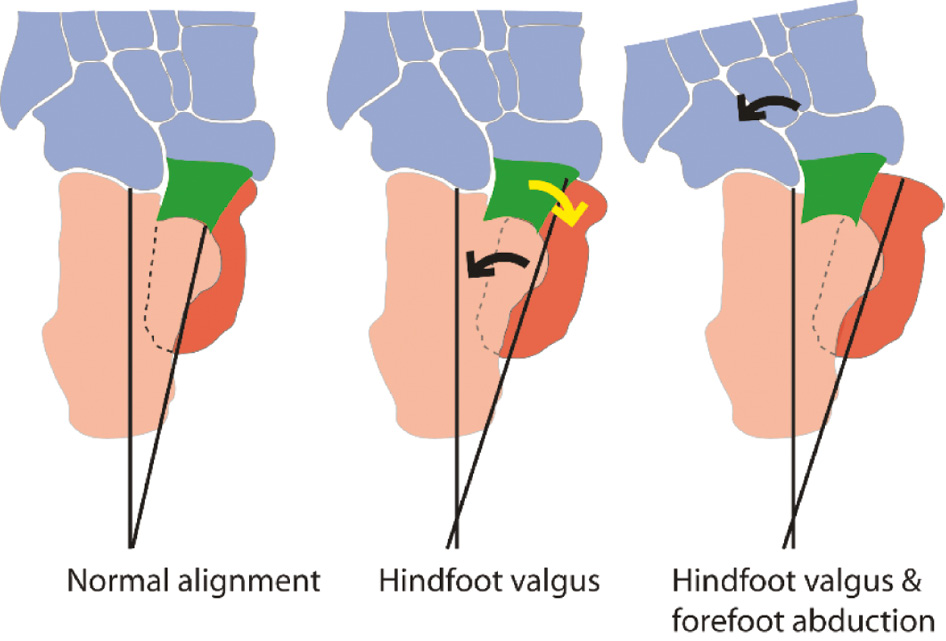
Figure 6. Lateral view radiograph of the foot of a child with severe flatfoot. The talus is markedly plantarflexed, the talonavicular joint is dislocated, and the hindfoot is in valgus.
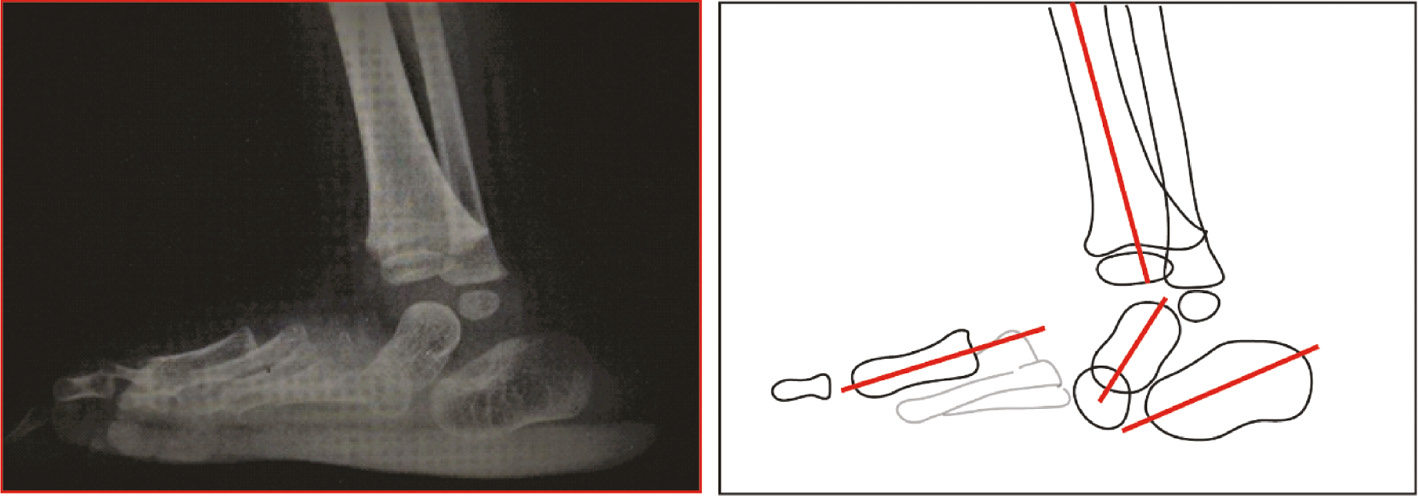
Biomechanical Basis and Rationale for Surgical Treatment of Flatfoot
Calcaneal Lengthening
Lengthening the lateral column of the foot to treat pes planus initially suggested by Dillwyn-Evans2 and promoted by Mosca,3 entails an open wedge osteotomy of the anterior end of the calcaneum. The anterior end of the calcaneum adducts along with the rest of the CPU restoring the support of the talar head by the spring ligament (Figure 7A, B, C). Restoration of the normal alignment of the talocalcaneonavicular joint results in a concomitant and obligatory reduction of the hindfoot valgus.
Figure 7. Diagrammatic representation of calcaneal lengthening (A, B, C) and the triple C procedure (D, E, F) as viewed from the sole. Calcaneal lengthening involves an open wedge osteotomy of the calcaneum (B, C) held open with a bone graft (yellow). The triple C procedure involves an open wedge osteotomy of the cuboid, a closed wedge osteotomy of the medial cuneiform, and a medial displacement osteotomy of the calcaneum (D, E, F). By adducting the forefoot, the support of the talar head by the spring ligament (green) is restored.

Triple C Procedure
The triple C procedure described by Rathjen and Mubarak4 entails a medial displacement osteotomy of the calcaneum, an open wedge osteotomy of the cuboid, and a closed wedge osteotomy of the medial cuneiform (Figure 7D, E, F) which corrects the forefoot abduction and the hindfoot valgus.5
Arthroereisis
While not commonly performed by pediatric orthopaedists, the operation corrects hindfoot valgus by preventing the sinus tarsi from closing (Figure 8).
Figure 8. Articulated model of the hindfoot bones shows that the sinus tarsi is closed when the subtalar joint is everted (A) and open when the joint is inverted (B). In arthroereisis, an implant placed in the sinus tarsi prevents the subtalar joint from everting (C).

The factors that contribute to causation of pes planus and the characteristics of the deformity are summarized in Tables 1 and 2.
Table 1. Factors That Contribute to Deformity
| Contributory Factors | Deformity | Structure Affected |
|---|---|---|
| Soft tissue contractures | Pes planus | Gastrocnemius-soleus muscle |
| Vertical talus | Gastrocnemius-soleus muscle Ankle and toe dorsiflexors Peronei Capsular contractures |
|
| Pes cavus | Tibialis posterior Plantar fascia |
|
| Spastic equinovarus | Gastrocnemius-soleus Tibialis posterior |
|
| Spastic equinovalgus | Gastrocnemius-soleus Peronei |
|
| Laxity of soft tissue | Pes planus | Spring ligament |
| Vertical talus | Spring ligament Tibialis posterior |
|
| Muscle imbalance across joints | Pes planus | Paralysis / weakness of tibialis posterior |
| Neurogenic vertical talus | Paralysis / weakness of tibialis posterior | |
| Pes cavus | Weakness of gastroc-soleus or tibialis anterior or intrinsic muscles | |
| Spastic equinovarus | Spasticity of gastrocnemius-soleus, tibialis posterior, tibialis anterior Weakness of peronei |
|
| Spastic equinovalgus | Spasticity of gastroc-soleus, peronei Weakness of tibialis anterior & posterior |
Table 2. Characteristics of Common Foot Deformities
| Deformity | Hindfoot Alignment | Forefoot Alignment | Position of the Talus | Talocalcaneo-navicular Joint | Medial Longitudinal Arch | Spring Ligament |
|---|---|---|---|---|---|---|
| Clubfoot & Spastic equinovarus | Varus | Adduction | Plantar-flexed | Navicular subluxed medially | Accentuated | Contracted |
| Flatfoot & Spastic planovalgus | Valgus | Abduction | Plantar-flexed | Navicular subluxed dorsally & laterally | Collapsed | Stretched |
| Vertical talus | Valgus | Abduction | Severely plantarflexed | Navicular dislocated dorsally & laterally | Reversed | Severely stretched |
| Pes cavus | Neutral / Varus / Valgus | Neutral /Adduction | Normal / dorsiflexed | Navicular subluxed plantarward | Accentuated | Normal /contracted |
CONGENITAL VERTICAL TALUS (CONGENITAL CONVEX PES VALGUS)
Congenital vertical talus is a complex deformity involving the hindfoot and forefoot (Figure 9).
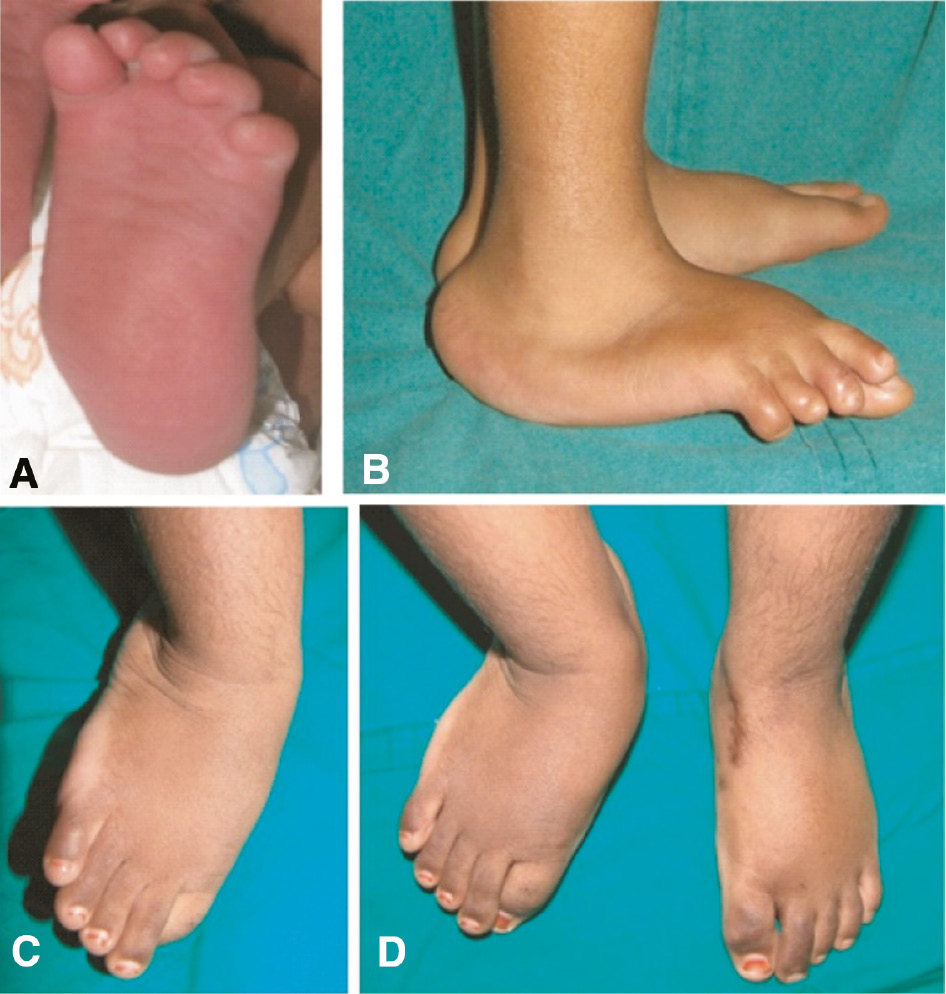
Figure 9. The deformities in congenital vertical talus include forefoot abduction (A) hindfoot equinus, forefoot dorsiflexion with reversal of the arch of the foot (B), hindfoot valgus and eversion of the foot (C). The medial border of the untreated right foot is convex while both borders of the left foot are straight following surgical correction (D).
Deformities of the Hindfoot
The severe hindfoot valgus, hindfoot equinus, and forefoot abduction in congenital vertical talus are an exaggeration of that seen in pes planus. This results in complete loss of support of the talar head by the spring ligament, and the talus lies vertically in plantarflexion (Figures 5 and 6).6,7
Deformities of Forefoot
The tibialis anterior and the toe extensors are contracted, which is a feature not seen in pes planus. This results in dorsiflexion of the forefoot in relation to the hindfoot. The navicular moves dorsally and dislocates dorsally. Contracture of the peronei contributes to the abduction deformity of the forefoot and lateral dislocation of the navicular.
The combination of deformities leads to the rocker-bottom appearance (Figure 10).
Figure 10. Contracture of both the ankle dorsiflexors and plantarflexor along with an ineffective tibialis posterior result in reversal of the longitudinal arch of the foot (green). The talus is severely plantarflexed with the head of the talus in the sole (red asterisk), and the navicular is dislocated dorsally (blue asterisk).

The factors that contribute to causation of vertical talus and their consequences are summarized in Tables 1 and 2.
Congenital vertical talus may occur as an isolated anomaly, as part of arthrogryposis, or in association with other syndromes. Paralytic congenital vertical talus may be seen in children with spina bifida.8 The underlying cause will have a bearing on treatment; isolated congenital vertical talus is likely to be more amenable to nonoperative treatment such as the Dobbs method. Arthrogrypotic vertical talus would need surgical release while tendon transfers may be needed for paralytic vertical talus.
Treatment
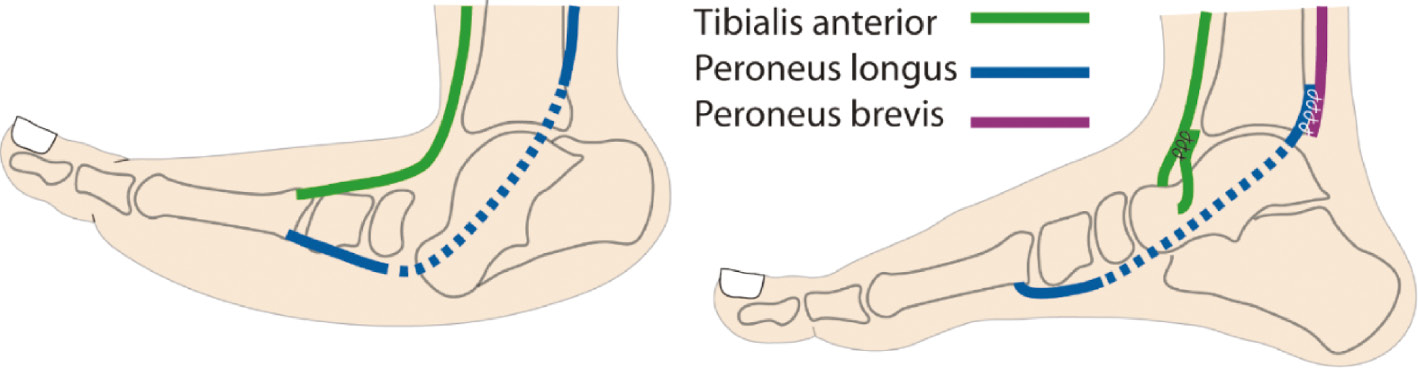
Serial manipulation of congenital vertical talus is diametrically opposite to that of clubfoot. The forefoot is adducted to correct the forefoot abduction and concomitantly minimize the hindfoot valgus through the reorientation of the CPU.9 The forefoot is also plantarflexed in an attempt to restore the arch of the foot. The talar head is used as a fulcrum while manipulating the forefoot.9 Once the forefoot deformities improve, reduction of the talonavicular dislocation is attempted. Tenotomy of the Achilles tendon is almost always needed to correct the equinus deformity. In the more recalcitrant cases, transfer of the tibialis anterior to the neck of the talus has been recommended.10 This removes a deforming force and converts it to a corrective force that pulls up the plantarflexed talus. Another salutary effect of this transfer is that it rebalances muscle forces acting on the first ray. Releasing the tibialis anterior from the first metatarsal results in unopposed action of the peroneus longus leading to plantarflexion of the first ray and accentuation of the longitudinal arch (Figure 11). This dynamic plantarflexion of the first ray will only occur if the peroneus longus is intact. Hence, if release of the peronei is deemed necessary, the peroneus longus can be divided proximally just above the ankle while the peroneus brevis is divided close to is insertion and the proximal stump of the peroneus brevis attached to the distal stump of the peroneus longus tendon.
Figure 11. Transferring the tibialis anterior to the neck of the talus facilitates restoration of the medial longitudinal arch. The peronei are sectioned at different levels and anchored to each other ensuring continuity of the peroneus longus tendon so that it can exert a plantarflexor force on the first metatarsal.
PES CAVUS
Pes cavus is characterized by a high medial longitudinal arch that fails to reduce in height on weight-bearing. Pes cavus may be a congenital anomaly without any underlying neuro-muscular disorder; this form does not progress and is usually asymptomatic. Neuromuscular pes cavus is, by far, more common and can occur in Charcot Marie Tooth disease (Hereditary Motor Sensory Neuropathy [HMSN]), poliomyelitis, spinal dysraphism. spina bifida, cerebral palsy, and Friedreich’s ataxia.11
Neuromuscular Pes Cavus
Neuromuscular pes cavus is associated muscle imbalance across the ankle, subtalar or metatarsophalangeal joints.
Patterns of Deformity
The longitudinal arch gets accentuated due to plantarflexion of the metatarsals or dorsiflexion of the calcaneum (Figure 12).
Figure 12. Mechanisms by which muscle paralysis can lead to a pes cavus deformity.

Apart from accentuation of the medial longitudinal arch, other deformities of the hindfoot and forefoot may be present. The pattern of these deformities is dictated by the pattern of muscle imbalance (Table 3).
Table 3. Patterns of Paralysis and Paralytic Deformities Associated with Pes Cavus
| Joint | Muscle Paralyzed | Deformity |
|---|---|---|
| Ankle | Tibialis anterior | Equinocavus |
| Gastrocnemius-soleus | Calcaneocavus | |
| Subtalar joint | Peronei | Cavovarus |
| Tibialis posterior | Cavovalgus | |
| Ankle & subtalar joint | Tibialis anterior & peronei | Equinocavovarus |
| MTP joints | Intrinsic muscles | Claw toes with secondary cavus |
In addition to muscle imbalance causing deformity, a forefoot deformity may induce a compensatory hindfoot deformity (Figures 8 and 9). Forefoot pronation secondary to a dropped first metatarsal seen in association with a compensatory hindfoot varus in HMSN is an example of this phenomenon. Primary and compensatory deformities are supple to begin with but tend to become rigid. The treatment strategies will vary depending on whether the deformity is supple or rigid. Differentiating a supple hindfoot varus from a rigid varus is possible by performing the Coleman block test (Figure 13).12
Figure 13. Appearance of left foot of a boy with a paralyzed tibialis anterior muscle (A). The first metatarsal is plantarflexed, the medial longitudinal arch is accentuated. Coleman Block test (B & C): On standing with both feet on the block, the left heel rolls into varus to enable the pronated forefoot to rest on the ground (B). When the plantarflexed first ray is not supported by the block and hangs free off the edge of the block, the normal alignment of the hindfoot is restored (C), indicating that the hindfoot deformity is supple.

Sensory Loss on the Sole in Association with a Cavus Deformity
Loss of sensation associated with a cavus deformity may occur when there is a lesion involving the first sacral segment of the spinal cord (e.g., as in low spina bifida). Loss of pain sensation alone with a cavus foot may be encountered in syringomyelia. A cavus deformity per se can result in high plantar pressures, increasing the risk of neuropathic ulceration. In addition, if there is a hindfoot varus or valgus deformity, the risk of developing plantar ulcers is much higher. In children with paralysis of the gastroc-soleus, the normal rockers of the foot in the stance phase are not seen, instead, there is uncontrolled dorsiflexion of the ankle after heel-strike. This results in shearing forces on the plantar surface of the heel which can result in ulceration (Figure 14).
Figure 14. In children with paralysis of the gastroc-soleus, the normal rockers in the stance phase are not seen. Uncontrolled dorsiflexion of the ankle produces shear forces under the heel (red arrow).

Angles measured on weight-bearing lateral radiographs will show the abnormal alignment of the hindfoot (Figure 15).13
Figure 15. Meary’s angle (left) of 15-30 degrees is considered moderate cavus, and an angle greater than 30 degrees is regarded as severe cavus. Calcaneal pitch (right) > 30 degrees is indicative of pes cavus.

Treatment of Pes Cavus
The deformity may be corrected by releasing soft tissue contractures (e.g., plantar fascia and the intrinsic muscles). Bony surgery will be needed in long-standing cases (dorsal wedge osteotomy of the base of the first metatarsal or the medial cuneiform and medial and proximal displacement osteotomy of the calcaneum).14 The tendency for progression or recurrence of deformity can be minimized by restoring muscle balance (Table 4).
| Tendon Transfer | Rationale |
|---|---|
| Transfer of peroneus longus to the peroneus brevis | Removes the muscle causing the first metatarsal to drop when the tibialis anterior is weak |
| Retains evertor power | |
| Jones transfer (transfer of the extensor hallucis longus (EHL) tendon to the neck of the first metatarsal) | The transferred EHL elevates the metatarsal countering the metatarsal drop in the presence of tibialis anterior weakness |
| Hibbs transfer of the extensor digitorum longus (EDL) tendons to the 2nd to 5th metatarsal necks | The transferred EDL elevates the metatarsals |
| Transfer of the flexor hallucis longus (FHL) from the distal phalanx to the proximal phalanx | The transfer reduces clawing of the hallux |
| Tibialis posterior muscle transfer to the dorsum of the foot | The transfer augments the power of ankle dorsiflexion in children with a weak tibialis anterior muscle |
| The transfer removes a deforming force if the hindfoot is in varus |
Neuropathic ulceration in children with sensory loss may be prevented by correcting deformities and making the foot plantigrade and restoring power of plantarflexion with an early tendon transfer to reduce shear forces under the heel.
PARALYTIC DEFORMITIES OF THE FOOT
Paralytic deformities of the foot develop if there is muscle imbalance across the axis of the ankle joint or the subtalar joint. The patterns of deformities are quite predictable when a particular muscle is paralyzed and depends on the relationship of tendons to the axes of the ankle and subtalar joints. The further a tendon runs from the axis of the joint, the greater the force moment that is generated by the muscle (Figure 16). A clear understanding of this concept is very useful for understanding why a deformity has developed and it is also vital for planning treatment.
Figure 16. Articulated model of the hindfoot showing the relationship of three tendons to the axes of the ankle (AA’) and subtalar joints (BB’). The extensor hallucis has a good dorsiflexor moment as it runs anterior to the axis of the ankle joint (AA’ above), but it has virtually no inversion or eversion moment as it runs almost in line with the subtalar axis (B’ below). The peroneus brevis and the tibialis posterior have strong evertor and invertor moments, respectively, as they run at a distance from the subtalar axis.

The normal relationship of the tendons crossing the ankle and subtalar joint can be depicted diagrammatically as shown in Figure 17.
Figure 17. Diagrammatic representation of a horizontal section through the ankle at the level of the malleoli. The axis of the ankle joint (AA’), the axis of the subtalar joint (BB’), and the position of tendons crossing the ankle are shown.
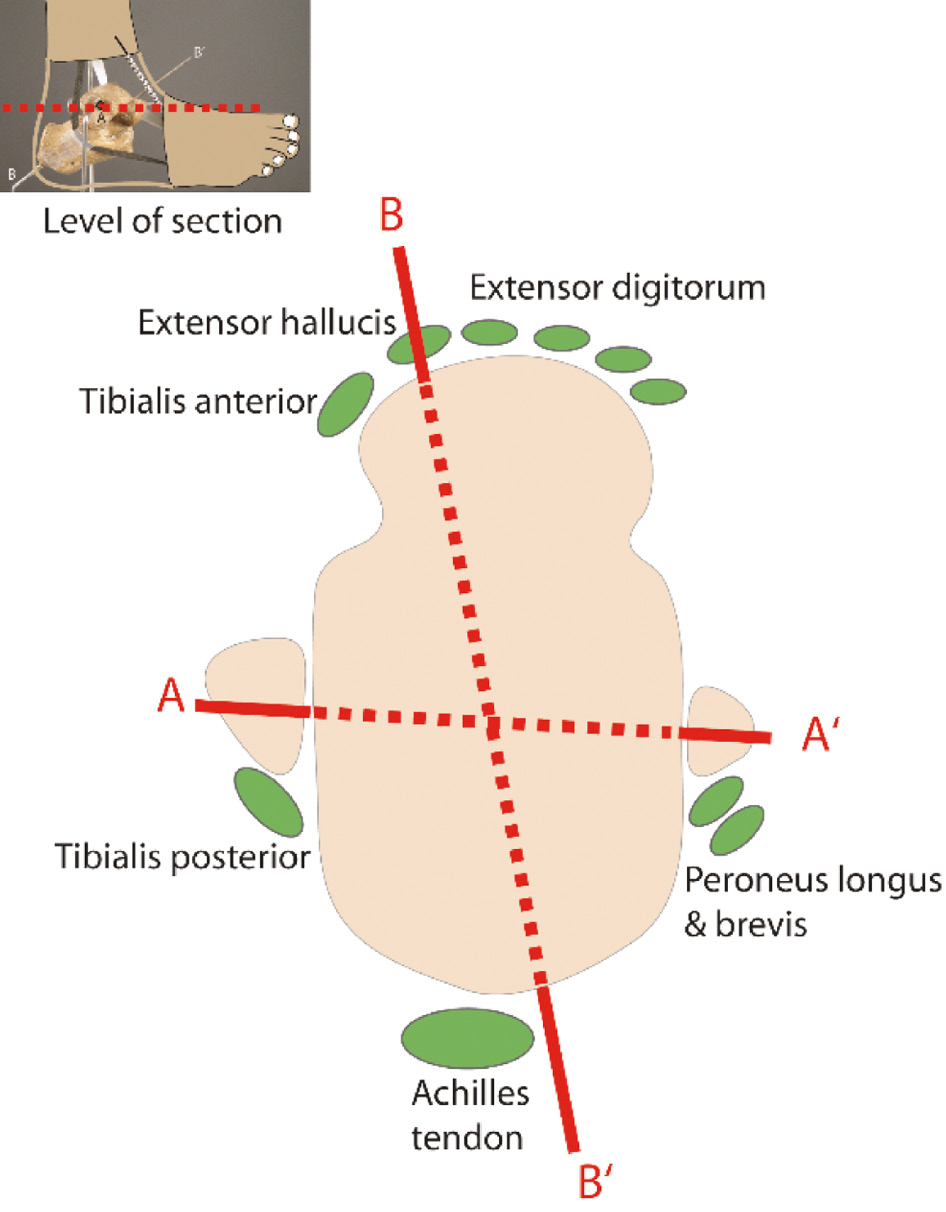
Tendons that run anterior to the axis of the ankle are dorsiflexors while those that run posterior to this axis are plantarflexors of the ankle. Similarly, all tendons running medial to the subtalar axis are invertors and tendons running lateral to the subtalar joint are evertors (Figure 18).
Figure 18. Action of muscles and their relationship to the axes of the ankle and subtalar joints.

The same template is used to plan tendon transfers to retore muscle balance across these axes and correct paralytic deformities (Figures 19 and 20).
Figure 19. Rationale of peroneus tendon transfer for isolated tibialis anterior paralysis.
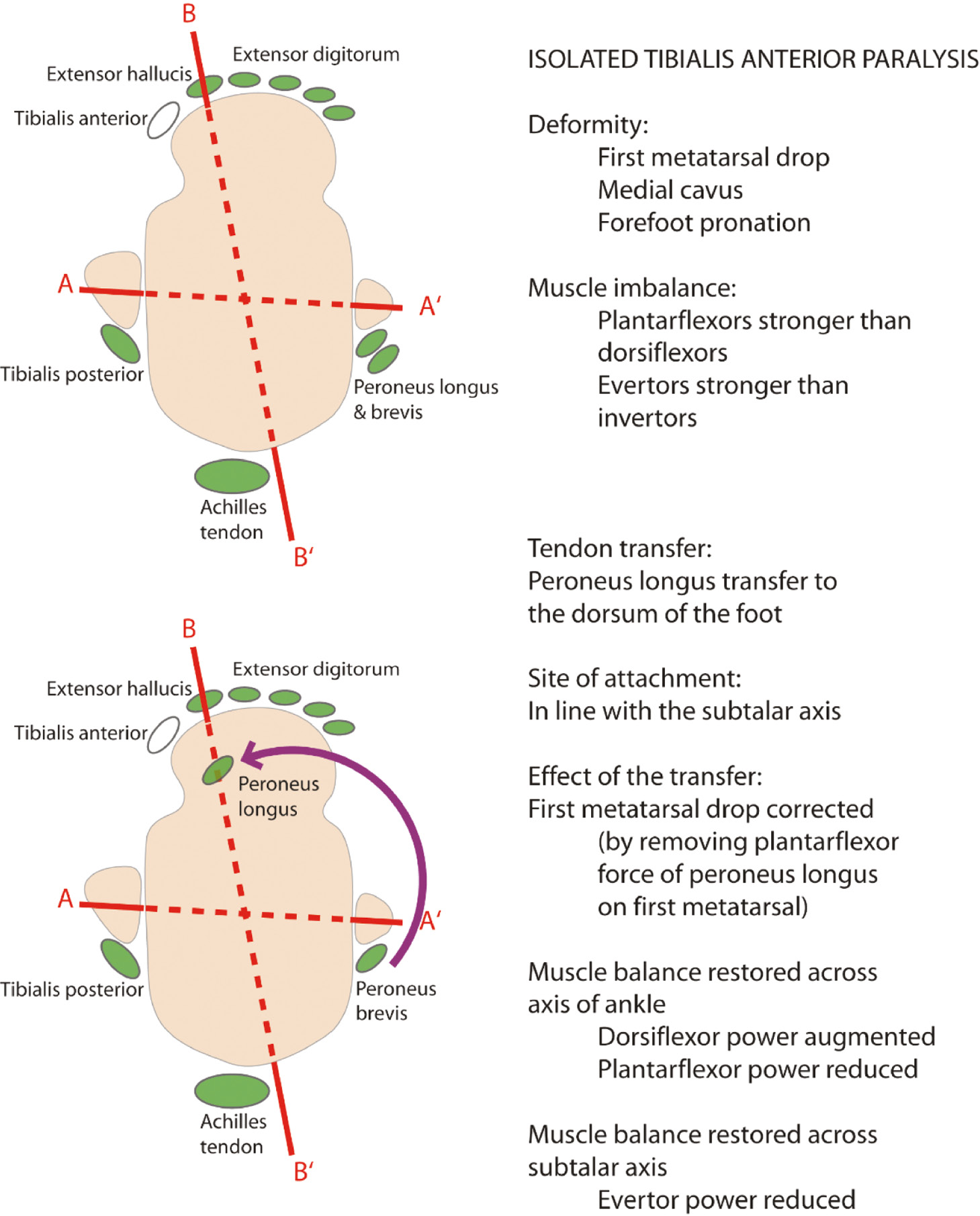
Figure 20. Rationale of performing a tibialis posterior transfer for peroneal nerve palsy.

The two examples of planning tendon transfer around the foot and ankle in Figures 19 and 20 show how the underlying muscle imbalance can be corrected with appropriate tendon transfers.
Intrinsic Muscle Paralysis
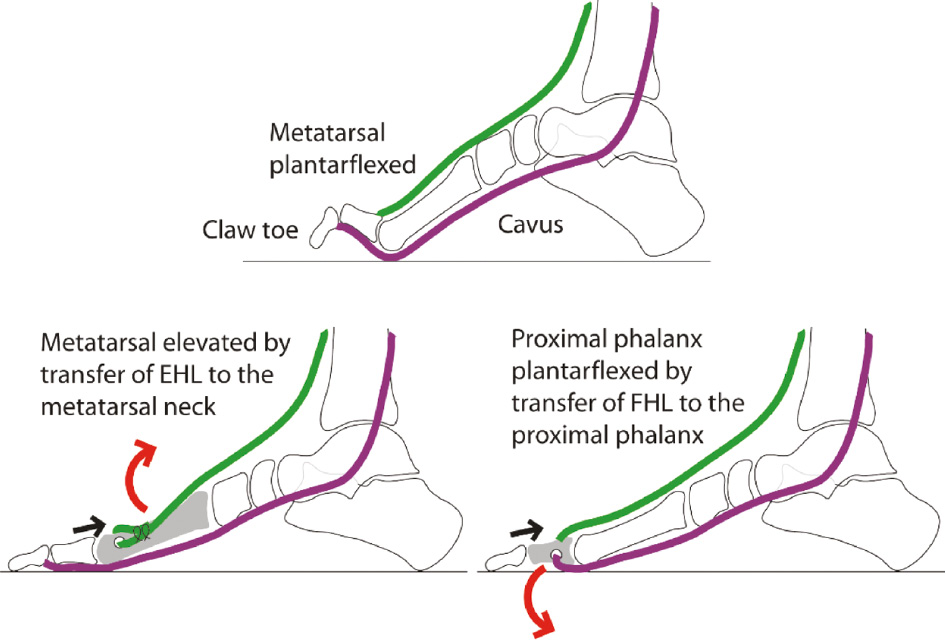
Paralysis of intrinsic muscles of the foot will result in clawing of the toes where the metatarsophalangeal joint (MTP) is hyperextended and the interphalangeal joints (IP) is flexed.17 Clawing can be reversed by preventing hyperextension of the MTP joint by pulling up the metatarsal or flexing the proximal phalanx by performing simple tendon transfers (Figure 21).
Figure 21. Tendon transfers for correcting clawing of the great toe.
FOOT DEFORMITIES IN CEREBRAL PALSY
Foot deformities are very common in children with cerebral palsy, and they arise due to muscle imbalance across the joints of the foot secondary to spasticity and muscle weakness.18 The deformities tend to be sequential and progressive with growth. Initially, the deformities are flexible and dynamic, and over time, myostatic contractures develop in the spastic muscles. The deformities then become more rigid and if left untreated, structural skeletal abnormalities develop.
The consequences of foot deformities in ambulatory children with cerebral palsy include lever arm dysfunction, poor power generation, and increase in energy expenditure during gait. The energy inefficiency of walking, in turn, leads to reduction in the ambulatory capacity of the children.18
The three common foot deformities noted in cerebral palsy are equinus, equino planovalgus, and equino-cavovarus.
Equinus & Equino Planovalgus Deformities
Equinus arises due to spasticity of the gastroc-soleus muscle. The relative contributions of the gastrocnemius and soleus differ based on the type of cerebral palsy. Gastrocnemius is the main contributor in spastic diplegic cerebral palsy while both gastrocnemius and soleus are spastic in hemiplegic cerebral palsy. Spasticity of either component of the gastroc-soleus can initially result in dynamic equinus, where the child walks on his or her toes but stands with the heel resting on the ground (Figure 22A–C).
Figure 22. Consequences of spasticity and contracture of the gastrocnemius muscle. Dynamic equinus in a three year old (A-C), mid-foot break in a seven year old (D-F), and valgus deformity of the hindfoot (G-I) in a fourteen year old.

The effect of a contracture of the gastrocnemius can manifest in different ways. Firstly, the child may stand and walk throughout the stance phase of gait with the foot in equinus with only the toes resting on the ground. Secondly, a mid-foot break may develop. The forefoot dorsiflexes while the hindfoot remains plantarflexed (Figure 22D–F), the medial longitudinal arch is reversed and only the forefoot rests on the ground. Thirdly, the hindfoot may develop a valgus deformity secondary to the contracted gastrocnemius and this enables the entire sole to rest on the ground (Figure 22G–22I). Often, a mid-foot break and hindfoot valgus develop concomitantly in older children with spastic diplegia (Figure 23). This equino planovalgus deformity of cerebral palsy has features similar in many ways to a severe planovalgus deformity with a tight Achilles tendon in otherwise normal children.
Figure 23. Forefoot abduction and forefoot dorsiflexion associated with equinus and valgus of the hindfoot and a mid-foot break seen on weight-bearing radiographs of an adolescent with cerebral palsy.

The valgus of the hindfoot and forefoot abduction lead to loss of support of the talar head and subluxation of the talonavicular joint. The hindfoot valgus leads to a reduction of the lever arm of the gastroc-soleus resulting in weakness of push off. The factors that contribute to development of equino-plano-valgus deformity in cerebral palsy are shown in Table 1 and 2.
Treatment
For young children 8 and below with flexible dynamic equino-plano-valgus:
Bracing using an ankle foot orthosis and physical therapy are the primary treatment options. If the response to these measures is poor, chemo-denervation of the gastrocnemius, serial casting followed by physiotherapy and bracing are tried.
For children over 8 years with a gastrocnemius contracture and fixed equino-plano-valgus:
Lengthening of the gastroc-soleus needs to be undertaken with caution as overcorrection (Figure 24) or undercorrection may occur.19
Figure 24. Severe calcaneus deformity in an adolescent who had undergone lengthening of the Achilles tendon.

In spastic diplegia, the gastrocnemius is contracted and usually the soleus is not. Consequently, unnecessary lengthening of the soleus, an important power generator, should be avoided as it can lead to iatrogenic crouch gait. Gastrocnemius recession is usually the procedure of choice. In patients with hemiplegia, both the gastrocnemius and the soleus are often contracted and, hence, lengthening of the Achilles tendon is justified.
For children over 12 years with rigid deformity:
Soft issue surgery as above and bony surgery as outlined in Table 5.
Table 5. Indications and Rationale of Operative Procedures for Equino-Plano-Valgus
| Indications | Procedure | Biomechanical Rationale | Comment |
|---|---|---|---|
| Mild or moderate spastic plano-valgus Ambulatory child |
Calcaneal lengthening20,21 | Corrects forefoot abduction and hindfoot valgus | Controversy as to whether it is effective if deformity is severe22,23 |
| Moderate spastic plano-valgus Ambulatory child |
Calcaneal lengthening + Talonavicular capsular reefing + Advancement of tibialis posterior |
Addresses soft tissue laxity in the medial column | Useful if forefoot abduction is not fully corrected following calcaneal lengthening |
| Persistence of forefoot abduction after calcaneal lengthening Poor ambulatory capacity |
Calcaneal lengthening + Talonavicular arthrodesis |
Corrects forefoot abduction and provides stable medial column | Minimizes risk of recurrence of forefoot adduction |
| Severe spastic equino-plano-valgus | Triple C procedure | Individual osteotomies can be adjusted to deal with varying severity of hindfoot valgus, planus and forefoot abduction | Preserves joint mobility |
| Severe deformity and limited ambulatory capacity | Subtalar arthrodesis | The hindfoot deformities can be well corrected | Loss of flexibility Low chance of recurrence |
| Limited ambulatory capacity Severe deformity not amenable to other procedures |
Triple arthrodesis | All deformities can be addressed at the respective joints at which they occur | Stiffens the foot |
There are some reports of satisfactory outcomes of subtalar arthroreisis, but the procedure has not been shown to be successful in other studies.24 Consequently, the procedure is not widely used for spastic equino-plano-valgus.
Spastic Equinovarus
Spastic equinovarus deformity is most frequently seen in hemiplegic cerebral palsy (Figure 25).
Figure 25. Severe spastic equinovarus in child with hemiplegic cerebral palsy.

It develops due to spasticity of the gastro-soleus and the invertors of the foot with weak dorsiflexors and evertors.
Treatment of spastic equinovarus has been summarized in Table 6.
Table 6. Indications and Rationale of Operative Procedures for Spastic Equinovarus
| Indications | Procedure | Biomechanical rationale | Comment |
|---|---|---|---|
| Young child Supple deformity (no contracture) |
Physiotherapy Chemo-denervation of gastrocnemius, tibialis posterior and anterior Orthosis |
Reduction of spasticity of deforming muscles & restore muscle balance | |
| Early contractures Deformity partially correctable |
Split transfer of the tibialis anterior (TA) or tibialis posterior (TP) to the lateral border of the foot | Restores muscle balance | Choosing which tendon to transfer (TA or TP) is based on their relative contribution to the deformity.25,* Split tendon transfers are preferred to whole tendon transfers to avoid risk of overcorrection. |
| Equinovarus deformity associated with skeletal deformity | Muscle rebalancing + Mid-tarsal osteotomy + Calcaneal osteotomy |
Corrects forefoot adduction and hindfoot varus | Unlike for pes plano-valgus no single osteotomy can achieve correction; multiple osteotomies may be required to improve alignment** |
| Severe, rigid deformity in adolescent | Muscle rebalancing + Triple arthrodesis |
All the deformities can be addressed | Severe deformity can be corrected but foot is rendered stiff |
*: This can be evaluated by a combination of clinical examination, observational and instrumented gait analysis, and EMG studies. TA overactivity is treated with a split tibialis anterior tendon transfer (SPLATT). TP overactivity is treated with a split tibialis posterior tendon transfer (SPLOTT). If both invertors show overactivity during gait on EMG, a SPLATT is combined with an intra-muscular lengthening of the TP.26
**: Surgeries for hindfoot correction include lateral slide osteotomy or a lateral closing wedge osteotomy of the calcaneus. Surgeries for rigid forefoot adduction and supination include dorsolateral closing wedge cuboid osteotomy and medial opening wedge osteotomy of the medial cuneiform.
Summary
In Part 1 we outline the normal foot mechanics and relationship between the hindfoot and the forefoot. As such, a basic understanding of the normal mechanics of the foot is needed to recognize the abnormal forces which lead to foot deformity. In the current Part 2 we identify common foot deformities which result from altered mechanics and present different options in order to correct. The factors that contribute to the causation and the cardinal clinical features of common deformities of the foot in children are summarized in Tables 1 and 2.
Disclaimer
No funding was received by the authors. The authors have no conflicts of interest to disclose.
References
- Tenenbaum S, Hershkovich O, Gordon B, et al. Flexible pes planus in adolescents: body mass index, body height, and gender--an epidemiological study. Foot Ankle Int. 2013;34(6):811–817.
- Evans D. Calcaneo-valgus deformity. J Bone Joint Surg Br. 1975;57(3):270-278.
- Mosca VS. Calcaneal lengthening for valgus deformity of the hindfoot. Results in children who had severe, symptomatic flatfoot and skewfoot. J Bone Joint Surg Am. 1995;77(4):500-512.
- Rathjen KE, Mubarak SJ. Calcaneal-cuboid-cuneiform osteotomy for the correction of valgus foot deformities in children. J Pediatr Orthop. 1998;18(6):775-782.
- Moraleda L, Salcedo M, Bastrom TP, et al. Comparison of the calcaneo-cuboid-cuneiform osteotomies and the calcaneal lengthening osteotomy in the surgical treatment of symptomatic flexible flatfoot. J Pediatr Orthop. 2012;32(8):821-829.
- Drennan JC, Sharrard WJ. The pathological anatomy of convex pes valgus. J Bone Joint Surg Br. 1971;53:455-461.
- Patterson WR, Fitz DA, Smith WS. The pathologic anatomy of congenital convex pes valgus. Post mortem study of a newborn infant with bilateral involvement. J Bone Joint Surg Am. 1968;50:458-466.
- Duckworth T, Smith TW. The treatment of paralytic convex pes valgus. J Bone Joint Surg Br. 1974;56(2):305-313.
- Dobbs MB, Purcell DB, Nunley R, et al. Early results of a new method of treatment for idiopathic congenital vertical talus. J Bone Joint Surg Am. 2006;88(6):1192-1200.
- Kissel CG, Blacklidge DK. Tibialis anterior transfer “into talus” for control of the severe planus pediatric foot: a preliminary report. J Foot Ankle Surg. 1995;34(2):195-199.
- Aminian A, Sangeorzan BJ. The anatomy of cavus foot deformity. Foot Ankle Clin. 2008;13:191-198.
- Coleman SS, Chestnut WJ. A simple test for hindfoot flexibility in the cavovarus foot. Clin Orthop Relat Res. 1977;123:60–62.
- Aktas S, Sussman MD. The radiological analysis of pes cavus deformity in Charcot Marie Tooth disease. J Pediatr Orthop B. 2000;9:137-140.
- Watanabe R. Metatarsal osteotomy for the cavus foot. Clin Orthop Relat Res. 1990;252:217-230.
- Guyton GP, Mann RA. The pathogenesis and surgical management of foot deformity in Charcot-Marie-Tooth disease. Foot Ankle Clin. 2000;5(2):317-326.
- Schwend RM, Drennan JC. Cavus foot deformity in children. J Am Acad Orthop Surg. 2003;11(3):201-211.
- Mulder JD, Landsmeer JM. The mechanism of claw finger. J Bone Joint Surg Br. 1968;50(3):664-668.
- Sees JP, Miller F, Overview of foot deformity management in children with cerebral palsy. J Child Orthop. 2013;7(5):373-377.
- Firth GB, McMullan M, Chin T, et al. Lengthening of the gastrocnemius-soleus complex: an anatomical and biomechanical study in human cadavers. J Bone Joint Surg Am. 2013;95(16):1489-1496.
- Kadhim M, Miller F, Pes planovalgus deformity in children with cerebral palsy: review article. J Pediatr Orthop B. 2014;23(5):400-405.
- Mosca VS. Lateral column lengthening as treatment for planovalgus foot deformity in ambulatory children with spastic cerebral palsy. J Pediatr Orthop. 2000;20:501-505.
- Kim JR, Shin SJ, Wang SI, et al. Comparison of lateral opening wedge calcaneal osteotomy and medial calcaneal sliding-opening wedge cuboid-closing wedge cuneiform osteotomy for correction of planovalgus foot deformity in children. J Foot Ankle Surg. 2013;52:162-166.
- Luo CA, Kao HK, Lee WC, et al. Limits to calcaneal lengthening for treating planovalgus foot deformity in children with cerebral palsy. Foot Ankle Int. 2017;38(8):863-869.
- Smith PA, Millar EA, Sullivan RC. Sta-Peg arthroereiesis for treatment of the planovalgus foot in cerebral palsy. Clin Podiatr Med Surg. 2000;17(3):459-469.
- Michlitsch MG, Rethlefsen SA, Kay RM. The contributions of anterior and posterior tibialis dysfunction to varus foot deformity in patients with cerebral palsy. J Bone Joint Surg Am. 2006;88(8):1764-1768.
- Vlachou M, Dimitriadis D. Split tendon transfers for the correction of spastic varus foot deformity: a case series study. J Foot Ankle Res. 2010;3:28.
