Invited Perspective
POGO Travel Journal: Tenwek Hospital in Bomet, Kenya
Pediatric Orthopaedic Division, UPMC Children’s Hospital of Pittsburgh, Pittsburgh, PA
Correspondence: Amanda J. McCoy, MD, MPH, FCS (ECSA), FAAOS, Pediatric Orthopaedic Division, UPMC Children’s Hospital of Pittsburgh, 4401 Penn Ave., Pittsburgh, PA 15225. E-mail: [email protected]
Received: February 11, 2022; Accepted: February 11, 2022; Published: May 1, 2022
DOI: 10.55275/JPOSNA-2022-0021
Volume 4, Number 2, May 2022

Introduction
After completing my pediatric orthopaedic fellowship, I had the unique opportunity to serve at Tenwek Hospital in Bomet, Kenya. I am often asked “why?” by colleagues when I indicate that I spent my first few years of practice in a lower-resourced setting. As with most life decisions, the answer is complex. I moved to Kenya in late October 2018 and quickly started practice. I remained there until early August 2021 when I transitioned back to the U.S. During my last few months in Kenya, I realized that I wanted to stay involved in expanding global access to pediatric orthopaedic care. As such, I joined the POSNA Pediatric Orthopaedic Global Outreach (POGO) Committee. As a new member, I have had the wonderful opportunity to collaborate and network with my fellow POSNA members to maintain and develop creative strategies to promote the provision of pediatric orthopaedic care in all regions of the world. The following are some of my experiences at Tenwek as an early career pediatric orthopaedic surgeon.
Background
Tenwek Hospital (Figure 1) is a 300+ bed mission hospital located in Bomet, Kenya. It started as a single nurse complex in 19371 and has since expanded into a 300+ bed hospital complex, offering services from preventative care to complex cardiac surgery. I first learned about surgery and surgical education as a form of missions and outreach as a high school student. I heard an inspiring presentation by Dr. David Thompson, a missionary general surgeon, at my local church, Allegheny Center Alliance Church (ACAC) in Pittsburgh, PA. Dr. Thompson spent his early career serving at Bongalo Mission Hospital in Gabon.2 He went on to found the Pan-African Association of Christian Surgeons (PAACS), an organization dedicated to increasing the surgical capacity in sub-Saharan Africa by developing and administering surgical residency programs to train physicians in Africa, who will then go on to care for patients in their local regions.3 Simultaneously, I learned that ACAC had an on-going relationship with Tenwek, which was in the process of developing its surgical programs. Within a few years, I learned that Tenwek opened its general surgery residency program in association with PAACS and the College of Surgeons of Eastern Central and Southern Africa (COSECSA). COSECSA began in 1999 in association with The Royal College of Surgeons of Edinburgh to meet the training and examination requirements needed to develop an internationally accredited local surgical workforce to care for the increasing morbidity of surgical conditions.4
Figure 1. Tenwek Hospital is a 300+ bed mission hospital in Bomet, Kenya.

At the time I learned about Tenwek and surgical education as a form of missions and relief work, I had not even decided to pursue medical school. However, growing up in Pittsburgh, PA, one of America’s cities with the highest levels of social, economic, and health inequity for Black Americans,5 I developed a strong interest in caring for under-resourced populations and ameliorating health inequities. As I learned more about the world, I wanted to expand my understanding of health inequity from the local level to a more global scale. I decided to serve at Tenwek for my 2-month elective time during my chief year in residency. At that time, I had committed to a pediatric orthopaedic fellowship for the next academic year, but I was flexible in my career plans thereafter. During my 2 months at Tenwek, I was able to work with residents in the PAACS/COSECSA orthopaedics training program. With the increasing burden of Road Traffic Injuries (RTI) sustained by people of all ages, including children, and the contribution of RTIs to global morbidity and mortality,6–9 it is necessary for the orthopaedic workforce in this region of the world to expand. Given my privilege of growing up in a high-income country and having accessibility to medical education and specialized training, I felt compelled to contribute in some way to ease the morbidity associated with musculoskeletal conditions in low- and middle-income countries (LMIC) through clinical care and orthopaedic education.
After being asked “why?” I am often asked “how?” I made the transition to practicing in Kenya. I would have found it very challenging to move to Kenya without the logistical support of a missions or relief agency. In my case, I joined with a Christian mission organization, which utilized the traditional missionary model. As such, I engaged with my network of friends and family to raise approximately $50,000 per year to cover expenses and provide a small living stipend. I received a grant to cover my student loan payments through MedSend.10 Just prior to moving to Kenya, I attended a 2-week cross-cultural training session to help prepare me for the transition. To practice in Kenya, I applied for a Kenyan medical license and a Kenyan work visa; it took about 6 months to obtain both documents. About a year after my arrival, I sat for the COSECSA written and oral examinations, allowing me to be recognized officially as a qualified orthopaedic surgeon and surgical educator. As for the American Board of Orthopaedic Surgery (ABOS), with recent new provisions, I was also able to collect cases and sit for the oral examination in 2020.
In terms of health requirements, before my trip during my chief year in residency, I made an appointment with our medical center’s travel clinic. I had to receive a few vaccines and boosters. When I moved to Kenya 2 years later, these vaccinations were all still up to date. Fortunately, Bomet is not in a malaria endemic zone given its elevation at 6,800 feet. However, I did have malaria prophylaxis for the times when I traveled to lower elevations near water. Additionally, I was advised to bring antiretrovirals to use for prophylaxis for needle sticks. In many lower-resourced regions of the world, the water from the faucet is not potable. While living in Kenya, I grew accustomed to drinking and cooking with filtered rainwater that was collected on the roof of my apartment. In terms of food, I used appropriate caution and kept ciprofloxacin on hand.
My Experience
In Kenya, Kiswahili and English are national languages with many local tribal languages. Tenwek is in the region of the Kipsigis tribe. The Kipsigis are a sub-tribe of the Kalenjin tribe, one of the largest tribes in Kenya and located in the highland areas of the Great Rift Valley. Many international marathoners come from this area.11 Accordingly, Kipsigis, Kiswahili, and English were spoken in and around our hospital. When I first arrived at Tenwek, we were so clinically busy, that I did not have time to formally learn Kiswahili upon my arrival. Fortunately, all hospital work was conducted in English, and I could easily converse with most of my patients younger than 30 years old (excluding very young children). Later on, I was able to take formal Kiswahili classes. I consider myself somewhat proficient and can carry out simple conversation.
The PAACS/COSECSA orthopaedic residency program started at Tenwek in 2014. At its inauguration, it became the fourth orthopaedics residency program in Kenya. Medical training in Kenya is based on the British model. Students matriculate to medical school after the completion of high school. Medical school is typically 6-7 years in duration. After completion of medical school, graduates must complete a mandatory intern year where they learn the principles of medicine, pediatrics, obstetrics and gynecology, surgery, inpatient, and outpatient care. After completion of internship, a doctor may practice as a medical officer (MO) or pursue further residency training. Typically, most physicians practice as an MO for a few years before starting residency. At Tenwek, we had two residents per year in orthopaedics (Figure 2). The first 2 years of the 5-year program are heavily focused on general surgery with only 6 months of orthopaedics. In many practice situations, our residency graduates may be the only surgeon available. Thus, he or she must be prepared to insert chest tubes, manage abdominal trauma, and perform C-sections in addition to managing orthopaedics. Often our trainees’ general surgery skills far exceeded my own, which presented a wonderful opportunity for learning. For example, I learned that conjunctival pallor was a reliable means of assessing anemia in patients of any race.12 The physical examination findings for anemia that I learned in medical school were often applicable only to lighter skin populations. A lot of my efforts and energies during my time at Tenwek went into helping administer the orthopaedics residency program, from determining the curricular schedule, evaluating trainees, procuring educational material, and facilitating journal club to bedside, clinic, and intra-operative instruction.
Figure 2. Tenwek PAACS/COSECSA orthopaedic residents for the 2021 academic year.

Clinical Operations
Clinically, the orthopaedics service typically ran two operating rooms daily and three rooms on Mondays. We generally performed about one to two elective procedures a day with the rest of our procedures encompassing some variety of orthopaedic trauma or infection. When I reviewed my practice, I found that 60% was managing some variety of adult trauma—both acute and delayed. Of my adult trauma practice, I found that 30% of my cases were acute femur fixation. This correlates well with Agarwal-Harding et al.’s finding that femur fractures had an incidence of 15.7-45.5 per 100,000 person years in LMICs.6 At Tenwek, we care for a catchment area of nearly one million people. I suspect that we met or exceeded this estimate given that we performed nearly 300 Surgical Implant Generation Network (SIGN) nails annually, though we used SIGN nails slightly more frequently for tibias than femurs. However, in addition to using SIGN nails for adult femur fixation, we liberally used cephulomedullary nails, sliding hip screws, cannulated screws, large fragment plates, blade plates, and distal femur locking plates to care for the variety of femur fractures that presented to our institution. Though relatively well-equipped for a mission hospital, we often ran into equipment challenges, including fewer power tools and dull instruments, saw blades, reamers, and drill bits.
The other 40% of my practice was dedicated to pediatric orthopaedic care, which included a variety of conditions including acute trauma, delayed trauma, oncology, congenital deformity, and neuromuscular. As you can imagine, there were significant differences in presentation compared to what I observed in my training in the U.S. However, there were also marked similarities. I would like to highlight a few of each. Though I do not have strong supporting data, I did observe that slipped capital femoral epiphysis (SCFE) often occurred in relatively tall and thin adolescent boys and girls, unlike the patients that the Western literature describes as obese.13–15 These patients also presented at an older age, 15-16 years old, than described in the literature. I do hypothesize that skeletal ages described in Western literature are not always generalizable to other populations. We often observed that our young adult patients in their late teens and early 20s had closing physes. Outside of later skeletal maturity, I suspect that there may have been some proximal hip morphology, such as increased femoral retroversion, related to the frequent observance of SCFE in this thin population. Unfortunately, with the many clinical demands, there was not much time to investigate the relationship.
Though not of serious consequence, I did treat many children with pre-axial polydactyl of the feet. Often times, there was a duplication of the distal phalanx or proximal phalanx of the great toe with or without separation of the nail plate. These feet were simply reconstructed with or without a proximal phalanx or metatarsal osteotomy and pinning. Very few feet had bracketed epiphyses that would lead to recurrent hallux varus deformity. I found it interesting that we are traditionally taught that post-axial polydactyl is common in children of African descent in the U.S. Generational African Americans in the U.S., who are descendants of the trans-Atlantic slave trade, are typically West African in origin. However, Kenya is located in East Africa; thus, perhaps the incidence and type of polydactyl varies throughout the African sub-continent. This is an important reminder that we must not view Africa and Africans as a monolithic culture and people group.
Management of Infection
An unfortunate observation I made was the increased frequency and severity of musculoskeletal infection that I encountered in children and adults. With the increased incidence of trauma, we observed high incidences of open fracture. I would dare to say that half of the tibial shaft fractures that we treated were open. And unlike in the U.S., these open fractures often presented in a delayed fashion after first acquiring reliable transportation to be evaluated at a local dispensary, which may then prompt referral to a county or district hospital, and finally referral to our institution. As the lack of reliable transportation may have been the cause of the accident in the first place, this process can take days. All the while, the fractured tibia may or may not be adequately immobilized, thus potentiating the soft tissue injury and compromise. Furthermore, as it has been well-stated in the literature, time to tertiary care facility, time to intravenous antibiotics, and time to debridement all matter.15 Thus, we commonly had the development of acute, subacute, and chronic osteomyelitis in our open fracture patients with delayed presentation. Unfortunately, chronic osteomyelitis is a very challenging pathology to manage.
However, the amount of osteomyelitis and septic arthritis I observed in children at Tenwek could not simply be explained by the increased incidence of trauma. The incidence of pyogenic acute hematogenous osteomyelitis in LMICs is reported as 43-200 cases/100,000. Whereas the incidence of acute hematogenous osteomyelitis in Western countries is reported as 1-12 cases/100,000.16–18 With delayed presentations, children often presented with bone abscesses or even evidence of chronic osteomyelitis with draining sinus tract. Additionally, distinguishing chronic pyogenic infections from extrapulmonary tuberculosis (Figure 3) often is a diagnostic dilemma. One of the hardest, but frequent, scenarios we came across, were children with chronic osteomyelitis that developed a pathologic fracture (Figure 4). In this situation, we needed to try to treat the chronic infection, but also achieve bone healing. Without infectious disease doctors and peripherally inserted central catheters, the medical management of both acute and chronic osteomyelitis can be challenging.
Figure 3. Radiograph of chronic extrapulmonary tuberculosis of the wrist in a 13-year-old boy confirmed with PCR testing.
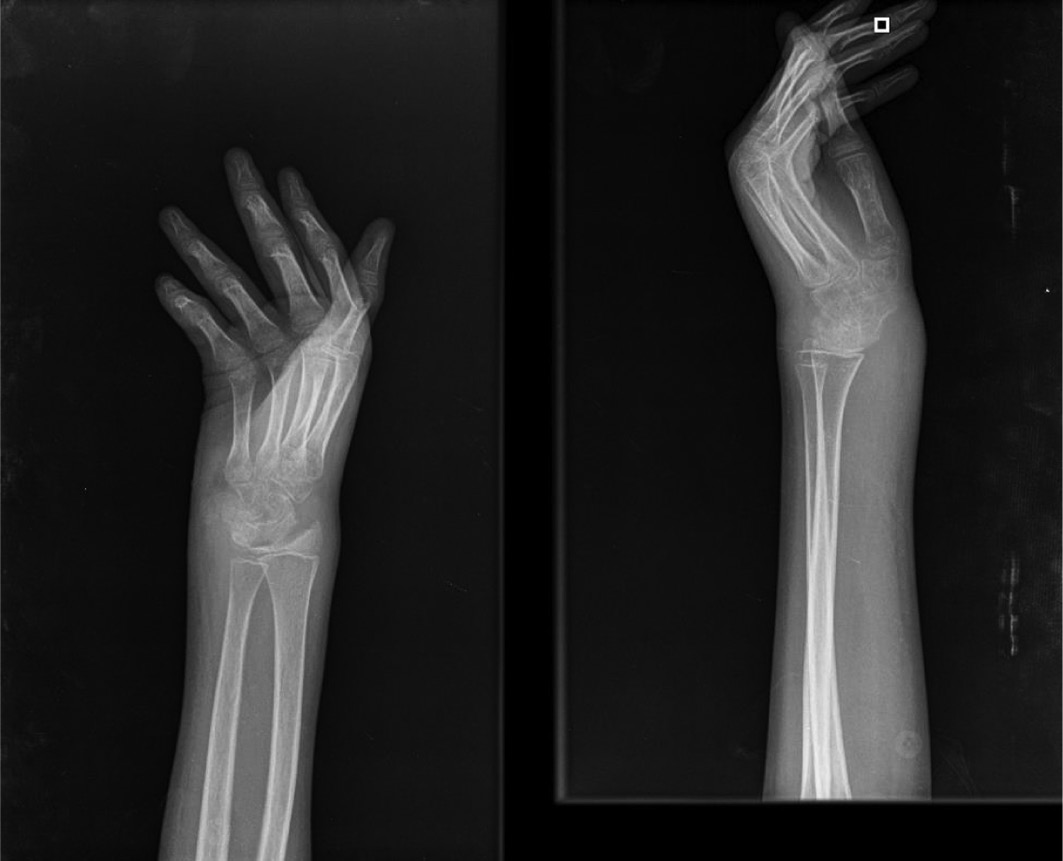
Figure 4. Radiograph of a 5-year-old boy with pathologic fracture of his left femur chronic osteomyelitis.

The effects of chronic osteomyelitis are far-reaching. Beyond the pain and discomfort associated with pathologic fractures and chronic draining sinuses (Figure 5), many patients are also limited in their educational and vocational opportunities. Because many secondary schools are boarding schools in Kenya, a student may be refused admittance if they have a chronic draining sinus as it is a sanitary and hygiene concern. Furthermore, in the case of fracture or stiffness from chronic infection, some secondary schools may not be able to accommodate the disability. For many in Kenya, manual labor is a primary form of employment. Thus, children with sequelae of chronic osteomyelitis are often excluded from these employment opportunities when they reach of age. However, non-manual labor often requires more formal education as a job requirement. Thus, unable to perform manual labor and unable to acquire the formal education required for non-manual labor, patients with chronic draining osteomyelitis are often at a loss.
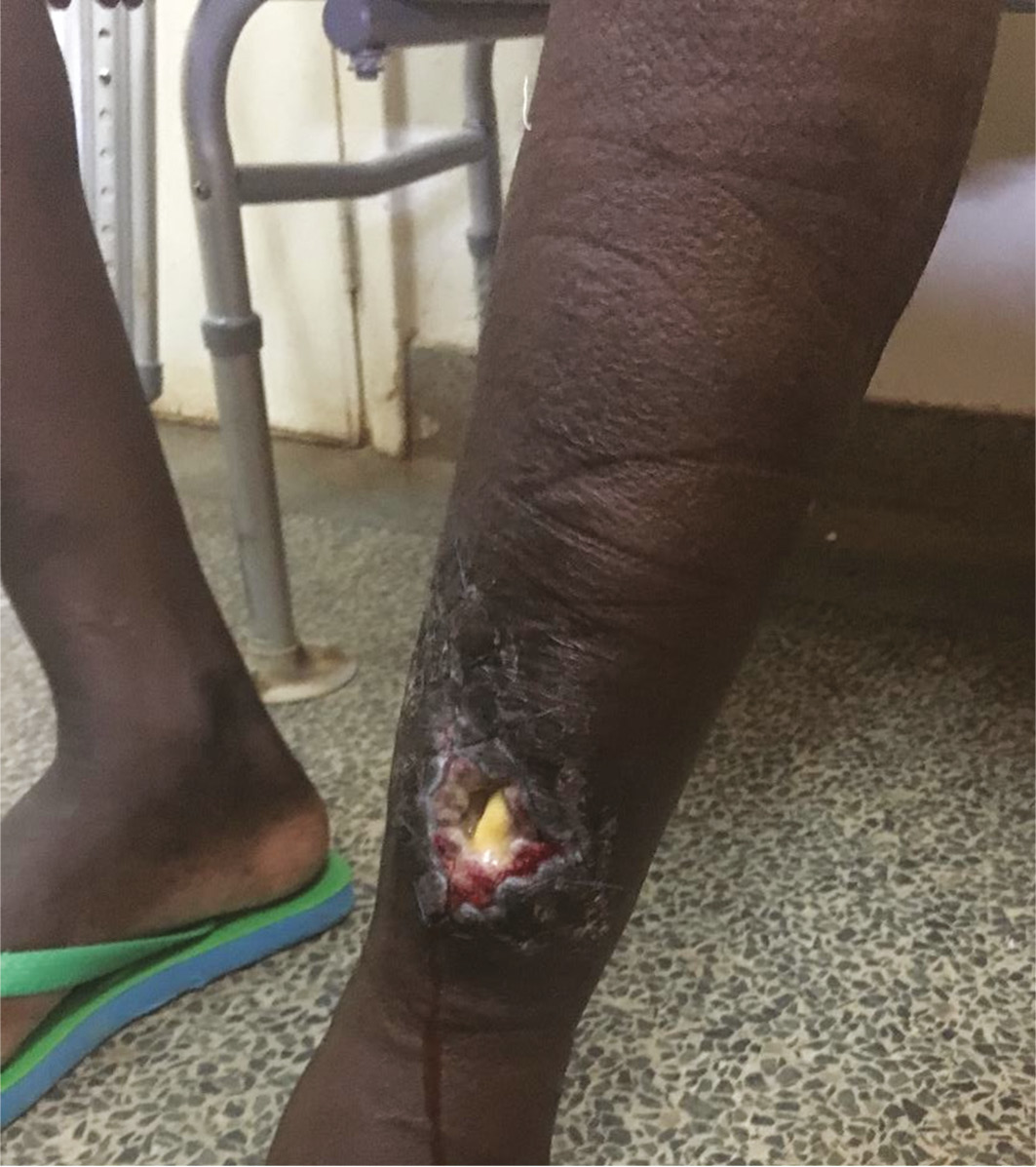
Figure 5. Clinical image of a patient with chronic osteomyelitis with draining sinus.
The approach for managing chronic osteomyelitis can be controversial, but principles are the same: remove necrotic and devascularized tissues, manage soft tissue dead space, confer stability, and treat infection.19 However, there are multiple methods of achieving this from temporary antibiotic coated nails and soft tissue antibiotic beads to large resections with bone transport. Unfortunately, most of these methods are not undertaken under the guidance and supervision of appropriately trained musculoskeletal providers. Regrettably, in some LMICs, access to these providers, the appropriate equipment, and appropriate facilities can represent a significant challenge. Thus, I would consider chronic osteomyelitis as an under-appreciated, under-recognized pandemic in LMICs, similar to that of trauma. When it comes to quantifying the impact of chronic osteomyelitis, it is a very challenging endeavor. However, if we study the burden of disease along with the interaction between chronic osteomyelitis and malnutrition, HIV, and diarrhea, then we can develop programs and strategies to reduce this burden.
Impact of Covid-19
Similar to the rest of the world, the COVID-19 pandemic substantially disrupted the economy, healthcare systems, and supply chains. At the onset of the pandemic, our hospital had 13 functioning ventilators for more than 300 beds and a catchment area of greater than one million people. Our ventilators actually represented a large proportion of ventilators available in the entire country. Furthermore, not all of our hospital’s beds were connected to oxygen. For example, in our adult ortho ward, only 2 out of 17 beds had oxygen access. As you can imagine, upon taking stock of our resources, the hospital leadership and stakeholders had long discussions about what equitable rationing of care would look like if we found ourselves overwhelmed with COVID-19 cases. One of our first priorities was to increase the amount of available oxygen by purchasing oxygen concentrators.
Though as an orthopaedic surgeon, I did not provide frontline respiratory care, the COVID-19 pandemic certainly changed our clinical pathways of managing patients. At baseline, we cared for a large burden of acute and delayed trauma at Tenwek. With the trauma comes accompanying pulmonary conditions including, but not limited to, pulmonary contusion, pulmonary embolus, pneumothorax, fat embolus, and acute respiratory distress syndrome. With delays in presentation, these respiratory conditions often presented at an advanced stage. Furthermore, trauma-related respiratory compromise was already occurring in a region with endemic tuberculosis and a high prevalence of rheumatic heart disease with valvular dysfunction often resulting in heart failure in young adults. At baseline, we had to work through a long list of differential diagnoses to care for our hypoxic patients. With COVID-19, we had yet another differential to add to our list. But, with the limited availability of PCR testing at the onset of the pandemic, we often were waiting days to confirm the diagnosis of suspected COVID-19. Though we did have a policy of mandatory surgical mask wear throughout the facility, like many places in the world, including the U.S., this was hard to enforce perfectly, particularly when patients had O2 saturations of 85% or less.
In a number of areas in Kenya, the economy is hand to mouth; crowded markets are necessary for many to earn a living wage. Like essential workers in the U.S., “work from home” was not always an option. To manage the crowded conditions, curfews were enforced nationally. Initially the curfew began at 7:00 p.m.; it was later liberated to 10:00 p.m. With the initiation of curfew, we cared for increasing numbers of injuries from disputes with the police in the enforcement of curfew and domestic disputes at home. The increase in domestic violence was not only seen in Kenya, but a similar phenomenon also occurred in the U.S.20 With fewer guns available, frequent weapons of choice included pangas (a machete-type knife used for harvesting grain) and other agriculture instruments, resulting in highly contaminated blood vessel, nerve, and tendon lacerations. The curfew also limited inter-county travel. For a very brief time, this temporarily reduced our trauma burden. But, later, we found ourselves managing an increased number of complications from delayed presentations as patients were not able to travel to our facility.
At Tenwek, we heavily relied on clinical visitors to help us manage our large clinical load. These typically were orthopaedic surgeons of all sub-specialties who would visit and help cover call anywhere from 1 to 4 weeks. It was helpful when visitors had multiple prior trips as it would decrease my call burden from every other night and weekend to one in three or one in four. Along with buffering the call schedule, visitors often brought with them very needed equipment, including SIGN nails. With international travel substantially shut down for a period of 6 months, we went without visitors. Thus, we had to determine other avenues of equipment procurement and negotiating customs. Fortunately, we were able to secure the required equipment. Prior to the COVID-19 pandemic, we regularly requested visitors to bring donated drills that their hospitals were releasing when they were updating their equipment. Even a refurbished drill system can be quite expensive, beyond the budget of Tenwek. However, we were able to secure sterilizable drill covers to place over standard hardware drills at a very affordable price.21 This unique solution enabled us to perform more procedures than if we were dependent on our donated supply, which was quickly diminishing with high use.
Reflection
What do I take away from my experience? Overall, I am immensely humbled by the opportunity to serve a few years in my early career at Tenwek. I left with a deep sense of gratitude for many things, including personal health, family, and friendship but also the opportunity to train to become a medical professional, yet alone, a pediatric orthopaedic surgeon. I also left my time in Kenya with a slightly increased awareness of how deep the trenches of healthcare injustice and inequity are in our global and local landscapes. I have seen two-physician families in Kenya lose their children to diarrheal illness, almost unheard of in the U.S. I have performed amputations for compartment syndrome from complications of casting minimally displaced metaphyseal distal radius fractures—a very rare occurrence—and what some institutions in the U.S. call a “never occurrence.” At the same time, in the U.S., Black children have increased length of admission and more procedures for osteomyelitis even when adjusting for insurance status.22 Children living in areas of high social deprivation have worse upper extremity function, mobility, pain interference, and peer relations scores on self-administered PROMIS CATs at presentation for care of upper extremity fractures.23 Children with congenital extremity differences living in more socially deprived areas also have worse self-reported PROMIS scores for pain interference, peer relations, anxiety, and depression.24
Where do we go next? It is important to acknowledge that the local and global inequities that we observe around the world and in our own practice environments are related. The social and political conditions in existence today that have tolerated the development and persistence of such stark health inequity and injustice domestically and in many regions of sub-Saharan Africa are directly related to their respective histories of exploitation. Anti-blackness and its corollary, white supremacy, are global phenomenon. During my time in East Africa, I saw many examples of the persistence of anti-blackness. As a generational African American, I continue to witness and experience anti-blackness personally and professionally in the U.S. These legacies both stem from the racism that provided for the colonialization of sub-Saharan Africa, the displacement of indigenous people, and the enslavement of people of African descent throughout the Americas. Thus, to address healthcare inequity locally and globally, it is imperative that we know the history and understand the systems of structural inequity at their root.
For those looking to engage in global orthopaedics work, I urge you to not simply accept the resource limitations of a given region but try to understand the social and political forces behind it. For those of us in North America, specifically the U.S., let us seek to better understand the history of socially deprived areas from which our patients come to us. History that includes red-lining and restrictive title deeds that resulted in de jure segregation in many American cities.25
In addition to learning about the structural inequities behind healthcare inequality, we must study it. By quantifying and documenting the unequal burden of morbidity and mortality incurred by pediatric orthopaedic conditions, we have an opportunity to advocate. Some of this advocacy may be directly related to provision of pediatric orthopaedic care by capacity building through educational programs for providers and acquisition of facility resources. I am thankful to have recently joined the POSNA POGO committee, whose aim is to increase the availability and quality of pediatric orthopaedic care around the world through the POGO/COUR scholar program, research, advocacy, and building relationships with our non-Western peers. Other parts of this advocacy may focus on changing the environmental conditions where children live, learn, and play. I consider myself especially fortunate to be part of the cadre of pediatric orthopaedists dedicated to advancing the musculoskeletal care of children worldwide through education, research, quality, safety and value initiatives, advocacy, and global outreach to children in underserved areas.
Additional Links
Pan-African Academy of Christian Surgeons: https://paacs.net/what-we-do/training-sites.html
Disclaimers
There are no disclosures or conflicts of interest related to the experience related in this work.
References
- Lewis G. Miracle at Tenwek: The Life of Dr. Ernie Steury. Grand Rapids, MI: Discovery House Publishers; 2007.
- Thompson DC. On Call, 2nd Edition. Camp Hill, PA: Wingspread; 2007.
- Pan-African Academy of Christian Surgeons: Who We Are. 2021. https://paacs.net/who-we-are/.
- College of Surgeons of Eastern Central and Southern Africa: Our History. 2021. https://www.cosecsa.org/our-history/.
- Howell J, Goodkind S, Jacobs L, et al. Pittsburgh’s ineqaulity across gender and race. Gender Analysis White Papers. City of Pittsburgh’s Gender Equity Commission; 2019.
- Agarwal-Harding KJ, Meara JG, Greenberg SLM, et al. Estimating the global incidence of femoral fracture from road traffic collisions: a literature review. J Bone Joint Surg Am. 2015;97:e31. doi: https://doi.org/10.2106/jbjs.N.00314.
- Beveridge M, Howard A. The burden of orthopaedic disease in developing countries. J Bone Joint Surg Am. 2004;86:1819-1822. doi: https://doi.org/10.2106/00004623-200408000-00029.
- Joshipura M, Gosselin RA. Surgical burden of musculoskeletal conditions in low- and middle-income countries. World J Surg. 2020;44:1026-1032. doi: https://doi.org/10.1007/s00268-018-4790-8.
- Cordero DM, Miclau TA, Paul AV, et al. The global burden of musculoskeletal injury in low and lower-middle income countries: a systematic literature review. OTA Int. 2020;3:e062. doi: https://doi.org/10.1097/oi9.0000000000000062.
- MedSend: About. 2021. https://medsend.org/about/.
- Warner G. How One Kenyan Tribe Produces the World’s Best Runners. NPR. 2013. Published online November 1, 2013.
- Sheth TN, Choudhry NK, Bowes M, et al. The relation of conjunctival pallor to the presence of anemia. J Gen Intern Med. 1997;12:102–106. doi: https://doi.org/10.1046/j.1525-1497.1997.00014.x.
- Aversano MW, Moazzaz P, Scaduto AA, et al. Association between body mass index-for-age and slipped capital femoral epiphysis: the long-term risk for subsequent slip in patients followed until physeal closure. J Child Orthop. 2016;10:209-213. doi: https://doi.org/10.1007/s11832-016-0731-y.
- Manoff EM, Banffy MB, Winell JJ. Relationship between Body Mass Index and slipped capital femoral epiphysis. J Pediatr Orthop. 2005;25:744-746. doi: https://doi.org/10.1097/01.bpo.0000184651.34475.8e.
- Murray AW, Wilson NI. Changing incidence of slipped capital femoral epiphysis: a relationship with obesity? J Bone Joint Surg Br. 2008;90:92-94. doi: https://doi.org/10.1302/0301-620X.90B1.19502.
- Oliver K, Eugene U, Lynn L, et al. Chronic osteomyelitis in Sub-Saharan Africa—a review. Glob Surg. 2019;5:1-5. doi: https://doi.org/10.15761/GOS.1000207.
- Robertson AJF, Firth GB, Truda C, et al. Epidemiology of acute osteoarticular sepsis in a setting with a high prevalence of pediatric HIV infection. J Pediatr Orthop. 2012;32:215-219. doi: https://doi.org/10.1097/bpo.0b013e3182468cd7.
- Okubo Y, Nochioka K, Testa M. Nationwide survey of pediatric acute osteomyelitis in the USA. J Pediatr Orthop B. 2017;26:501-506. doi: https://doi.org/10.1097/BPB.0000000000000441.
- Penny JN, Spiegel D. Chronic osteomyelitis in children. In: Spiegel D, Gosselin RA, Foltz M, eds. Global Orthopaedics: Caring for Musculoskeletal Conditions and Injuries in Austere Settings. New York, NY: Springer; 2014.
- Sharma A, Borah SB. Covid-19 and domestic violence: an indirect path to social and economic crisis. J Fam Violence. 2020;1-7. doi: https://doi.org/10.1007/s10896-020-00188-8.
- Arbutus Medical Pro Drill Kit. https://arbutusmedical.com/drillcover-pro-system/.
- Young JD, Dee EC, Levine A, et al. Does universal insurance and access to care influence disparities in outcomes for pediatric patients with osteomyelitis? Clin Orthop Relat Res. 2020;478:1432-1439. doi: https://doi.org/10.1097/CORR.0000000000000994.
- Okoroafor UC, Gerull W, Wright M, et al. The impact of social deprivation on pediatric PROMIS health scores after upper extremity fracture. J Hand Surg Am. 2018;43:897-902. doi: https://doi.org/10.1016/j.jhsa.2018.06.119.
- Wall LB, Wright M, Samora J, et al. Social deprivation and congenital upper extremity differences – an assessment using PROMIS. J Hand Surg Am. 2021;46:114-118. doi: https://doi.org/10.1016/j.jhsa.2020.08.017.
- Rothstein R. The Color of Law: A Forgotten History of How Our Government Segregrated America. Liverright Publishing Corporation; 2017.
