Current Concept Review
Injury Patterns in Rugby Union—America’s Fastest Growing Sport
1Department of Orthopaedics, University of Illinois Chicago, Chicago, IL; 2Department of Orthopaedic Surgery, University of California–San Diego, San Diego, CA; 3Department of Orthopaedics, San Antonio Military Medical Center, San Antonio, TX; 4Division of Orthopaedic Surgery, Rady Children’s Hospital, San Diego, CA
Correspondence to: Eric W. Edmonds, MD, Rady Children’s Hospital San Diego, 3020 Children’s Way, San Diego, CA 92123, E-mail: [email protected]
Received: January 13, 2022; Accepted: January 19, 2022; Published: February 1, 2022
DOI: 10.55275/JPOSNA-2022-0019
Volume 4, Number 1, February 2022
Abstract:
Rugby union is the fastest growing sport in the USA, and its growth is only expected to continue to climb with the approaching 2023 Rugby World Cup. Rugby union carries risk for general and sport-specific injury. Tackles and high-impact collisions are a regular component of the game, and although often compared to American football, rugby union carries a unique pattern of injuries, with certain injuries occurring at a significantly higher rate. This review is aimed at familiarizing our orthopaedic workforce to the sport of rugby union and the evaluation, diagnosis, and treatment of the rugby union athlete. Injury prevention strategies guided by epidemiology, risk factors, and mechanisms of injury in rugby union athletes are critical.
Key Concepts:
- Rugby union is a rapidly growing sport with a unique pattern of injury distinct from American football.
- Managing in competition head injuries is similar to all sporting competition and is relevant in preventing sequela such as chronic traumatic encephalopathy.
- Proper tackling form is imperative for injury prevention, particularly injuries to the head and shoulder.
- Lower extremity injuries, particularly those at the thigh and knee, account for the greatest amount of time lost to injury.
Introduction
Rugby union is played globally in 121 countries.1 As of 2018, there are 3.5 million registered rugby players worldwide and another 6.1 million unregistered rugby players.2 Historically an international competition, rugby union is currently the fastest growing sport in the United States, including more than 125,000 registered players in 2016.3 As the most popular contact sport worldwide, and involving frequent bouts of high intensity activity, rugby union carries risk for general and sport-specific injury. Tackles and high-impact collisions are a regular component of the game as is common in contact sports. Although often compared to American football, rugby union at the collegiate level carries an overall injury rate ratio of 3.1, highlighting the significantly higher rate of injury seen in rugby athletes.3 Rugby athletes experience a particularly increased risk of concussion and upper extremity injury, particularly at the shoulder.3 Additionally, within the collegiate ranks, men face a 30% higher rate of injury compared with women during rugby competition.4 And, there is a unique distribution of injuries by sex.4 For example, women suffer an anterior cruciate ligament (ACL) injury at 5 times the rate of men, whereas men are 2.5 times and 6.6 times more likely to suffer a fracture and open wound, respectively.4 Accordingly, the treating physician should be comfortable with the evaluation, diagnosis, and treatment of a wide range of injuries, from common time-loss injuries to nonfatal catastrophic injuries (Table 1).5–16 Additionally, a thorough understanding of the epidemiology, risk factors, and mechanisms leading to injuries in rugby union athletes is critical for the implementation of effective prevention strategies and protocols.
Table 1. Incidence (Per 1000 Player-Match Hours) and Severity (Days Prior to Return to Play) of Time-Loss Injuries Sustained by Rugby Union Players by Location of Injury5–16
| Location of Time-Loss Injury | Incidence (per 1000 player-match-hours) | Severity (days prior to return to play) |
|---|---|---|
| Head | 2-13 | 5-35 |
| Concussion | 0.6-12 | 3-22 |
| Fracture (nose, skull, mandible, maxilla, zygomatic, orbital, etc.) | <1 | 33-70 |
| Laceration/Abrasion | <1 | 6-38 |
| Thoracic | 4-9 | 8-16 |
| Spine | 11 | 12 |
| Cervical | 4-7 | 10-68 |
| Thoracic | <1 | 5-6 |
| Lumbar | 3-4 | 8-38 |
| Upper Extremity | 13-17 | 21-32 |
| Shoulder | 2-13 | 8-66 |
| Hand/Fingers | 1-5 | 22-43 |
| Lower Extremity | 45-47 | 15-19 |
| Thigh | 13-16 | 4-14 |
| Knee | 10-11 | 7-258 |
| Lower Leg/Achilles | 8-10 | 5-116 |
| Ankle | 5-10 | 8-18 |
Historical Background
Rugby union originated in England during the first half of the 19th century. Two primary variations currently exist, Rugby-15s and Rugby-7s, the latter being a faster-pace version with fewer players on the field (seven players versus standard 15 players). The game begins with a kick-off. Rugby-15s is divided into 40-minute halves, while Rugby-7s consists of 7-minute halves. Advancing down the field occurs through forward running of the ball-carrier, kicking, or within a scrum or maul.
Players on the field are divided into forwards and backs, with each position best suited for specific physical dimensions and athlete characteristics. Forwards primarily gain and retain possession of the ball, playing a critical role in tackling and rucking opposing players. Hookers and props, or front-row forwards, require significant upper-body strength to provide stability at the leading edge of formations such as the scrum. On the other hand, backs create and convert point-scoring opportunities. They are generally smaller, faster, and more agile than forwards (Figure 1).
Figure 1. Rugby positions (Image used with permission from USA Rugby.)

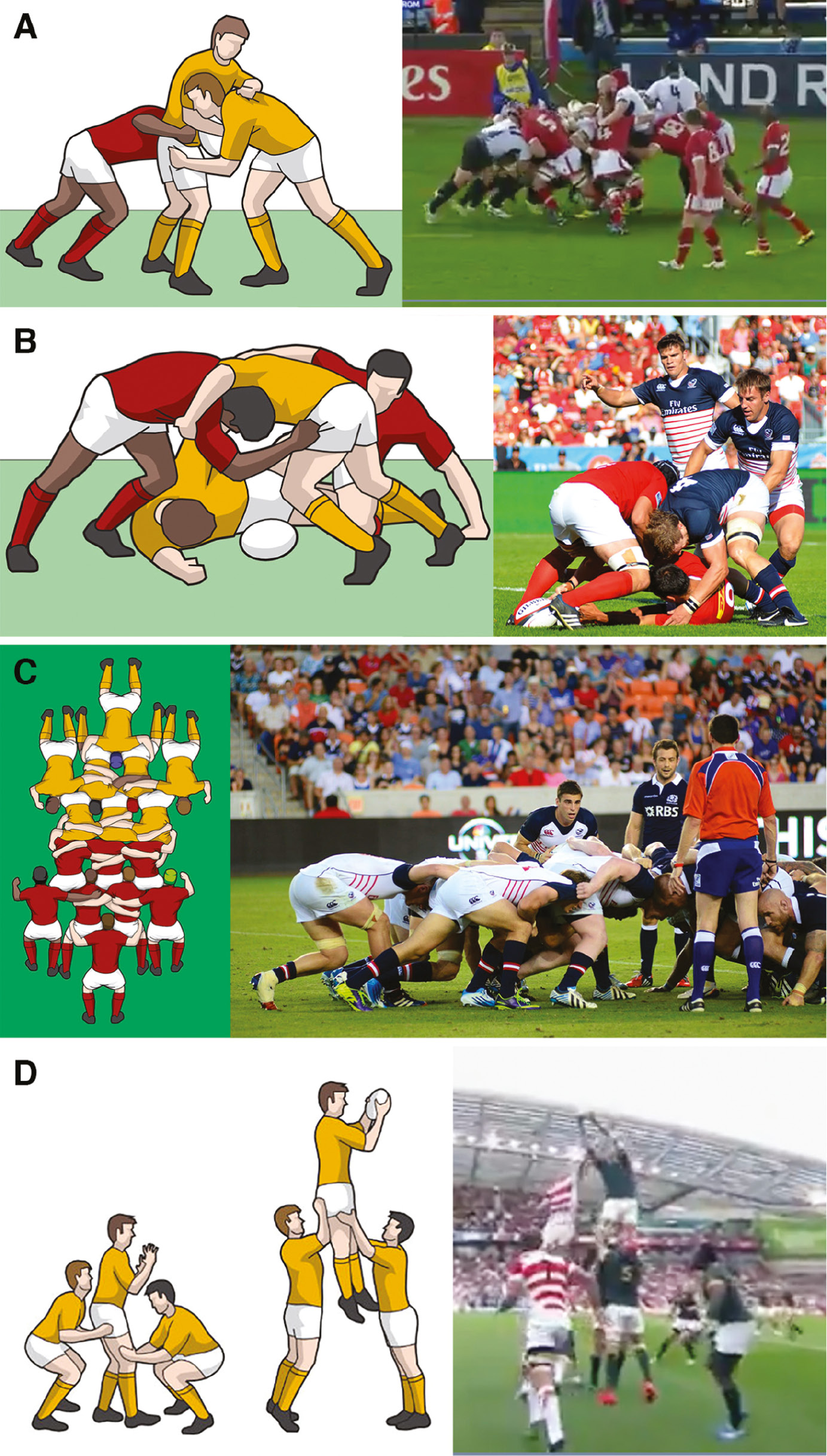
Tackling is a staple of the sport and has been the focus of much injury prevention reform. The tackler must attempt to completely wrap their arms around the ball-carrier to complete the tackle. Tackles above the shoulder are illegal, making the head and neck out of bounds. Mauls are open play formations that occur after the ball-carrier has come into contact with the opponent but has remained on their feet. Players from each team can then bind onto their teammates and attempt to make forward progression (Figure 2A). If the ball touches the ground, a ruck is formed (Figure 2B). Players from each team surround the ball and use their feet to either move the ball back or drive themselves forward. Players may not directly handle the ball in the ruck until it has passed to the team’s hindmost foot, at which time it may be picked up. Set pieces include scrums and lineouts. Scrums restart the game following a minor infringement. Eight forwards from each team crouch down and bind together in three rows before interlocking with the opposing team. The ball is rolled into the gap between the two front rows (also known as the tunnel) and the Hookers compete for possession by hooking the ball backwards with their feet. During this time, each side attempts to push the opposing team backwards to better position their Hookers (Figure 2C). A lineout resumes play after the ball leaves the field of play. Forward players from each team line up perpendicular to the sideline. The ball is thrown down the center of the line, at which time both sides compete for the ball (Figure 2D).
Figure 2A-D. Rugby formations and set pieces: A) Maul, B) Ruck, C) Scrum, D) Lineout (Images used with permission from USA Rugby.) Protective equipment in rugby union is optional and strictly regulated. Boots have soles with metal or plastic studs to allow grip on the pitch turf—a critical aspect to provide the leverage required during contact situations. Head gear consists of a thin scrum cap, not more than 10 millimeters in thickness. Mouthguards, non-rigid shoulder pads, shin guards, and chest pads are approved for use but not required.
Head Injuries
Head injuries constitute a considerable proportion of the overall injury rates in rugby union. The overall incidence rate has been reported to be up to 13 head injuries per 1000 player-match hours and accounting for as much as 16% of all time-loss injuries.5,6
Time-loss head injuries include concussions (~60%), fractures (~15%)—nose, skull, mandible, maxilla, zygomata, orbit—and lacerations/abrasions (~12%).6 On average, head injuries result in 4 to 5 weeks of missed play.6 The large majority of head injuries are attributed to contact events, with tackling events responsible for 64% of all head injuries and 74% of concussions.6 Foul play, including punching, head butting, and eye gouging, accounts for a significantly smaller proportion of head injuries (~11%).6 Incorrect head positioning, defined as “in front of the ball carrier,” resulted in 69.4 head injuries per 1000 tackles, compared to a rate of 2.7 head injuries per 1000 tackles with correct head positioning “behind or to one side of the ball carrier.”17 Incorrect head positioning places the head and face in an unprotected position, making them vulnerable to injury from the ball carrier’s driving legs. Incorrect head positioning occurs in approximately 10% of all tackles, indicating that education and strict enforcement of proper tackling technique may significantly reduce the rate of head injuries among rugby athletes (Figure 3).17
Figure 3. Head positioning during tackling.

Concussions have an overall incidence of 4.73 per 1000 player-match hours with a recent increase in rates, perhaps due to increased monitoring and/or reporting.8,18 Community (sub-elite) level rugby has also demonstrated a higher incidence of concussion when compared with elite/international level rugby, indicating an inverse relationship between incidence of concussions and level of expertise.8 Once again, proper technique and training seem to play a crucial role in injury prevention. Interestingly, concussion rates may occur at a greater rate in Rugby 7s, compared with Rugby 15s, which may be related to fatigue and tournament logistics.9 In the possibly concussed athlete, primary evaluation should focus on airway, breathing, and circulation, followed by an evaluation for cervical spine injury.19 Following clearance of the above, focus can be shifted to concussion evaluation. Neuropsychological testing is the primary diagnostic procedure used.19 CT and MRI on the other hand, are reserved for cases in which serious injury is suspected, characterized by the presence of a prolonged loss of consciousness (>30 minutes) or focal neurologic deficits.19 Severe injuries such as intracranial bleeds are exceedingly rare but have been reported.20 Once a diagnosis of concussion is established, standardized concussion protocols should be followed (understanding that currently there is often poor adherence to return-to-play recommendations).6,8 As with any concussion, long-term neurocognitive deficits with chronic traumatic encephalopathy have been seen in rugby union players.8 Thus, the rugby athlete with multiple or repetitive concussions should receive more conservative management with prolonged recovery periods before return-to-play.19
Recommendations to limit head injuries, concussions in particular, include implementation of pitch-side concussion assessment protocols, enhanced player compliance with return-to-play protocols, improved refereeing of illegal hits, more severe consequences for illegal hits, and improved player tackling technique. The majority of research on protective equipment (headgear, mouthguards) has not demonstrated a risk reduction for concussions.8,19
Thoracic Injuries
Thoracic/trunk injuries occur at a rate of eight to 11 injuries per 1000 player-match hours, with an average of 16 days of missed play.5,7 Rugby players are at high risk for thoracic injury given the minimal thoracic protective gear that is worn during training or matches, with full-backs and loosehead props being particularly susceptible to chest injuries.21 While the majority of contact-induced thoracic injury involves superficial musculoskeletal structures, the evaluating physician should also be aware of rare, yet potentially lethal internal organ injuries, including commotio cordis and pulmonary injuries.22
As a superficial structure in the anterior thorax, the sternum is susceptible to injury during rugby play. Anterior blows to the chest may result in sternal contusions. Sternal fractures are relatively rare given the elastic recoil of the ribs; however, when present, sternal fractures may be associated with rib fractures, pulmonary/cardiac contusion, pneumothorax, and extremity fractures.21 Sternoclavicular joint (SCJ) dislocations are rare entities, accounting for only 3% of all shoulder girdle injuries.21 Conventional radiographs are the primary diagnostic method of choice for sternal injuries. CT may detect subtle fracture lines and SCJ dislocation, while MRI is superior in detecting soft tissue injuries, bony contusions, and surrounding hematomas.21
Thoracic compression most commonly leads to rib fractures just anterior to the angle of the rib—its weakest point.21 First, rib fractures have the potential to cause injury to the underlying aorta and subclavian artery, requiring thorough physical examination. Ultrasound is an easily accessible and useful modality for evaluating rib fractures which present as gaps, steps, or displacements in the rib cortex. These injuries are typically treated conservatively, with primary attention given to managing symptoms. Costochondral injuries are also possible with anterolateral blows to the chest usually in the middle or lower ribs.21 The pectoralis major is susceptible to injury from a direct blow to the muscle during tackles. Ultrasound is sensitive for complete (grade III) ruptures, while MRI is highly sensitive for all grades (grades I-III). Complete ruptures of the pectoralis major, classically presenting as avulsion injuries at or near the humeral insertion, require surgical intervention.23 Partial tears may be treated conservatively, though this is associated with decreased strength.21,23
Spine Injuries
The incidence of spine injury, including cervical, thoracic, and lumbar, is 10.9 per 1000 player-match hours and 0.37 per 1000 player-training hours.11 Spine injuries result in an average of 12 days of missed play, with the most overall amount of time lost secondary to nerve root injuries sustained during matches and lumbar disc injuries sustained during training.11
In regard to incidence of injury, the cervical spine is most common, likely due to impacts caused during tackles and scrums, followed by the lumbar spine.11 Among match activities, the tackle (37%) and scrum (19%) account for the largest proportion of spine injuries, while weight-lifting is the most common cause of training injuries.11 Front-row forwards, including Hookers and loosehead props, are at particularly high risk for sustaining cervical spine injuries during scrums.11 A particularly devastating c-spine injury that can be encountered as a result of scrums is fracture-dislocation, most commonly of the C4-C5 or C5-C6 facet joints. Neck hyperflexion was previously thought to be the most frequent mechanism of cervical spine injury; however, recent work has demonstrated buckling, or vertex compression, of the cervical spinal column to be a more likely mechanism (Figure 4).24
Figure 4. Buckling injury during scrum resulting in extension of proximal vertebrae, flexion of distal vertebrae, to decelerate torso relative to head. (Right image used with permission from USA Rugby.)

Stingers occur in roughly 20% of players in any given season, with tackling as the most frequent inciting event.25 Normally a clinical diagnosis, radiographs should be obtained if symptoms persist for greater than one hour, localize to one nerve root, or include neck pain with limited cervical spine range of motion.26 Radiographs are also indicated in athletes with a history of more than one stinger episode, which should be followed by an MRI for spinal cord and brachial plexus evaluation.26 There is no current consensus regarding return to play following a stinger, though some advocate for immediate return to play in the presence of complete symptomatic resolution and full, painless cervical range of motion.25 On the other hand, absolute contraindications to return to play include a second stinger in the same match, persistent neurologic deficits, bilateral symptoms (stingers are exclusively unilateral), neck injury suspicion, continued neck pain or discomfort, and lack of full cervical range of motion.25
The incidence of pars interarticularis defects may be as high as 31% in rugby players secondary to repetitive microtrauma from supraphysiological loads.27 Symptoms are classically characterized by lower back pain exacerbated by lumbar hyperextension, and possible neurologic symptoms in the presence of spondylolisthesis.27 Evaluation of suspected acute pars defects should include MRI or single photon emission computed tomography (SPECT), as these are most sensitive for acute lesions, though CT is excellent for more progressive disease.27 Management includes both nonoperative (rest, orthosis, physical therapy) and rarely operative (Buck’s repair, Scott’s wiring technique, Morscher technique) intervention.27 Across all sports, return to play is 3.7 months for conservative management and 7.9 months for operative therapy, though more research is required to elucidate which is the optimal treatment strategy.27
Catastrophic cervical spine injuries (CCSI), defined as spine injuries resulting in death, tetraplegia, or permanent neurologic deficits, are rare in rugby union, with rates varying between 0.0008-0.0001 per 1000 player-match hours.11,24,28 The majority of CCSIs occur in front-row players (55%) and most commonly during the scrum (39%).28 Any trauma patient with potential cervical spinal cord injury should first be evaluated according to ATLS guidelines, which include evaluation for circulatory function, airway patency, and regular breathing.26 Additionally, in athletes with a history of cervical spine injury, a screening MRI should be used prior to rugby participation.29
Retired rugby players have a higher incidence of chronic neck pain and reduced neck mobility when compared to the general population. In addition, they possess higher rates of MRI-detected degenerative lesions, including foraminal stenosis and narrowing of the spinal canal.30 This highlights the long-term sequelae of repetitive cervical spine trauma in rugby athletes and the need for preventative measures. Implementation of specific prevention programs and scrum law changes has led to a significant decrease in catastrophic cervical spine injuries in French Rugby Union. These include the creation of an academy whose purpose is to train players, coaches, educators, and referees on front-row positioning, days of mandatory training for coaches and club officials regarding medical information and prevention, and scrum engagement changes that reduce impact on front-row players.28
Upper Extremity
Upper extremity injuries account for 14–28% of all rugby injuries, with an overall incidence of up to 13.1 injuries per 1000 player-match hours.12 Sprains and strains account for 53% of these injuries, with fractures (17%) and dislocations (11%) also being common.12 Among fractures, 90% occur in the forearm, wrist, or fingers, while shoulder injuries primarily consist of sprains/strains and dislocations.12 Shoulder injuries are the most common, accounting for 66% of all upper extremity injuries sustained in rugby union, followed by hand/finger (20%) and wrist (6%) injuries.12
The shoulder is the most commonly injured upper extremity structure, being three times as likely to be injured as the hand or finger, resulting in an average of 37 days of missed play.12,13 The high rate of shoulder injury is likely due to the shoulder being involved as a primary point of body contact in rugby skills such as tackling, ruck, maul, scrum, and lineout.12 Acromioclavicular (AC) joint injuries are the most common (3.7/1000 player-match hours) while dislocations are associated with the greatest recovery time until return to play (207 days of missed play).13
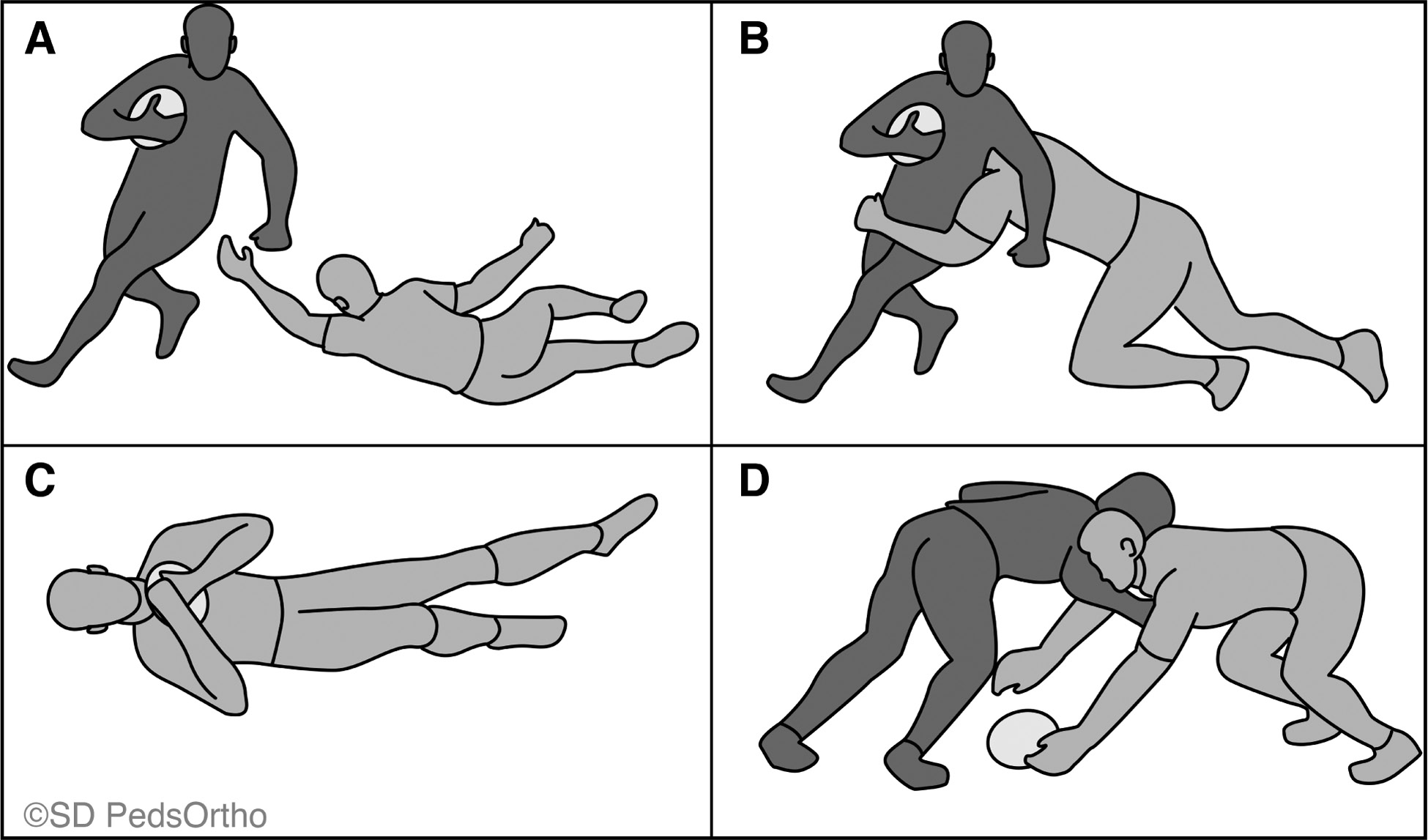
Four distinct mechanisms of traumatic shoulder injury have been described in rugby union. The “Diving Tackler” or “Try-Scorer” consists of hyperflexion of the outstretched arm and accounts for the majority of rotator cuff tears (Figure 5A).31 The “Tackler” involves extension of the abducted arm behind the player while executing a tackle (Figure 5B). Both the “Diving Tackler/Try-Scorer” and “Tackler” mechanisms result in a leveraging force on the glenohumeral joint resulting in anterior glenohumeral joint dislocations and superior labral tear from anterior to posterior (SLAP) lesions. The “Direct Impact” mechanism is the primary contributor to AC joint injuries and results from a direct blow to the arm or shoulder that is held by the side in neutral or slight adduction (Figure 5C).31 A significant proportion of anterior shoulder dislocations also occur during the “Poaching Position,” which results in a direct posteroinferior force from an opposing player to the shoulder with the arm flexed greater than 90 degrees, usually occurring in the crouched rucking position (Figure 5D). Education regarding proper tackling technique should focus on avoiding tackles with an outstretched and abducted arm and instead, tackling with internal rotation and antepulsion of the arm, thereby directing forces to the shoulder rather than the abducted humerus.31 Similarly, players should be discouraged from diving for the try line with the ball in hand of an outstretched and hyperflexed arm.
Figure 5A-D. Mechanisms of shoulder injury: A) Diving Tackler/Try-Scorer, B) Tackler, C) Direct Impact, D) Poaching Position
Glenohumeral subluxations/dislocations account for 1.5–1.6% of all injuries sustained by rugby union athletes, according to a French epidemiologic study on rugby injuries.32 These injuries often result in chronic instability, with recurrent dislocations occurring in approximately two-thirds of rugby athletes with a prior shoulder dislocation. On-field reduction is not recommended; closed reduction should be performed with appropriate analgesia to decrease voluntary and involuntary muscle contractions that may hinder reduction.33 Reduction maneuvers should utilize gentle, constant, in-line traction rather than jerking, forceful traction that may lead to iatrogenic injury. This should be followed by confirmatory radiographs demonstrating concentric reduction of the humeral head within the glenoid fossa. A thorough neurovascular examination should be performed, as 6% of cases are associated with nerve injury, most commonly to the axillary nerve.33 Conservative treatment consists of sling immobilization for several weeks, though optimal positioning of the arm in external rotation or internal rotation remains controversial. Interestingly, in-season functional bracing may not improve success rates of conservative treatment.34 Recently, primary surgical repair of first-time anterior glenohumeral dislocations has become popularized with studies showing lower rates of recurrence.33,35 The two most common shoulder stabilization procedures are the Bankart repair, a capsulolabral repair often performed arthroscopically, and the Bristow-Latarjet procedure, which involves a coracoid transfer to the anterior glenoid.36 While arthroscopic approaches have been demonstrated to be equivalent to open surgical approaches for shoulder stabilization, this remains controversial in collision sport athletes.37,38 Both procedures produce excellent functional outcomes with rugby athletes returning to sport at previous level of play. Ultimately, decisions on treatment modality should incorporate a holistic picture, including clinical and radiographic findings and patient preferences (i.e., return to play timing, patient goals, level of play). Studies have shown return to play rates after these procedures to be on average 13 months.35
Given the prevalence and often recurrent nature of upper extremity injuries in rugby union athletes, prevention strategies are needed. As mentioned above, education regarding player positioning during high-risk skills (e.g., tackle) is critical. Players should also receive tutorials regarding falling technique, such as learning to avoid falls onto the elbow locked in extension, which transmits forces to the glenoid through the humeral head.13 With regard to protective gear, foam/cotton felt pads have been used in the past to reduce impact to the shoulder in athletes returning to play post-injury. However, shoulder pads do not reduce force applied to the shoulder joint, and thus are unlikely to be effective in protecting the shoulder during impact.39
Lower Extremity
The lower extremity is the most commonly injured body region among rugby players, with an overall incidence of 47 injuries per 1000 player-match-hours and an average of 19 days of missed play.5 Injuries at the thigh, particularly those involving the hamstring muscle and thigh hematomas, account for the highest proportion of lower extremity injuries. However, these tend to be less severe when compared to knee injuries.15 Fractures, on the other hand, are relatively uncommon.40
Knee injuries account for approximately 20% of all days absent from play and training.15 The medial collateral ligament (MCL) is the most commonly injured knee structure, followed by chondral meniscus injuries, soft tissue hematomas, and loosely defined “sprained” knees.15,41 While the average knee injury results in 37 days of missed play, ACL injuries are significantly more severe and typically result in greater than 200 days of missed play. The majority of knee injuries occur during contact, including up to 86% of ACL injuries.15,42 Specifically, the tackle event is associated with greater than 50% of ACL injuries and 46% of MCL injuries. This is in contrast to other sports, such as soccer and basketball, in which the majority of ACL injuries occur in non-contact maneuvers involving pivoting or cutting. Within rugby, non-contact ACL injuries most commonly occur during an evasive side-stepping maneuver.
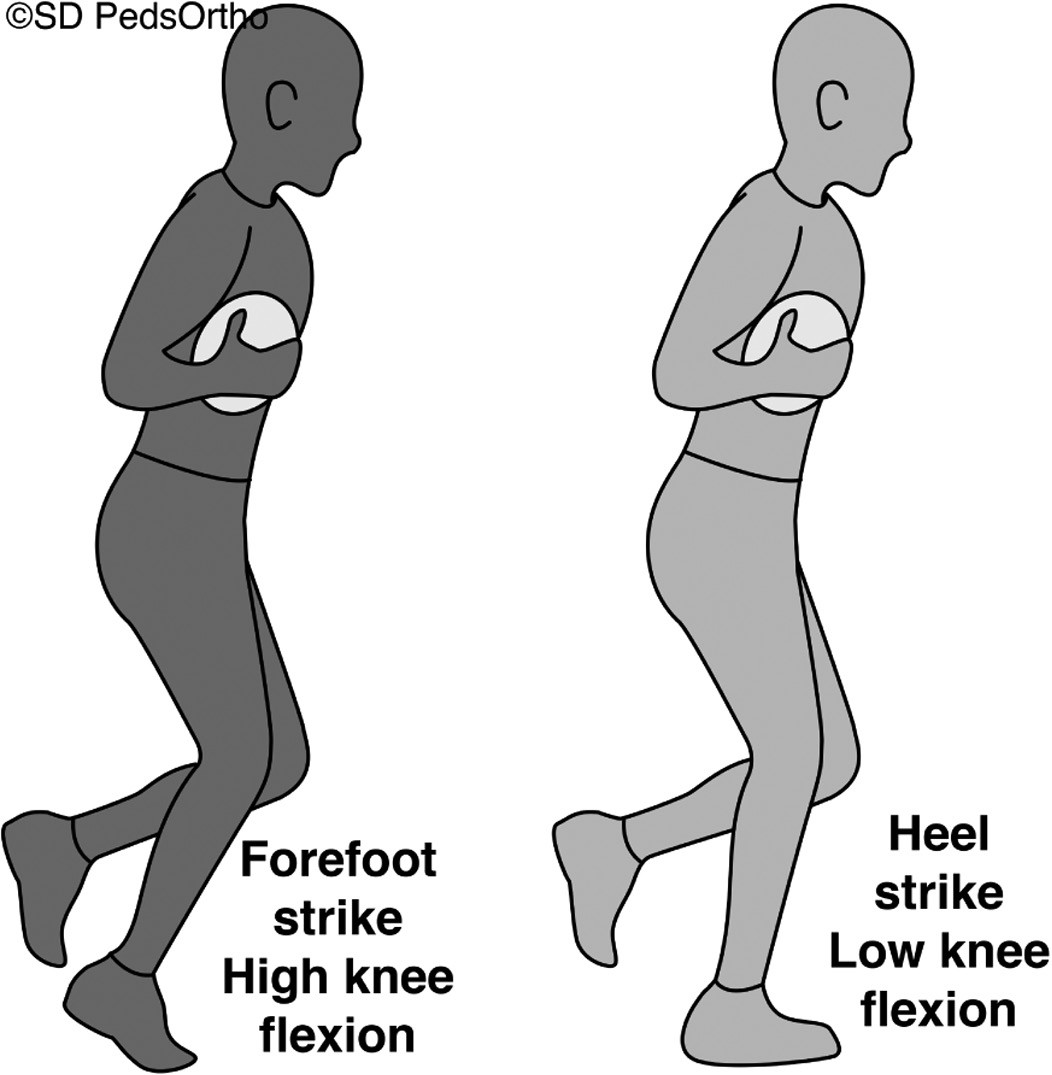
Early diagnosis and treatment of ACL injuries is crucial, as delays in diagnosis are associated with increased rates of concurrent injuries, including medial meniscal tears. The large majority of ACL injuries will require ACL reconstruction surgery.15 Interestingly, younger rugby athletes have demonstrated inferior outcomes following ACL reconstruction, exhibiting higher rates of hamstring autograft rupture, greater fear of reinjury, and greater time needed to overcome fear of reinjury.43 The treating physician should take into account the higher activity level, earlier return to sport, and poorer compliance with postoperative rehabilitation protocols common among younger rugby players that may be contributing to this discrepancy in outcomes. Rugby athletes should also receive training with regard to on-field lower extremity mechanics. Heel strike and low knee flexion angles upon initial ground contact are risk factors for non-contact ACL injury (Figure 6).42 Training programs should focus on minimizing such suboptimal landing forces that place increased stress on the ACL.
Figure 6. Running form to prevent non-contact ACL injury. Left: forefoot strike with greater knee flexion carrying lower risk of ACL injury. Right: heel strike with lesser knee flexion carrying greater risk of ACL injury.
Ankle injuries are also a significant source of morbidity in rugby, accounting for 10-20% of match and training injuries.16 Lateral ligament injuries are the most common while Achilles tendon ruptures and lateral malleolar fractures are associated with the greatest time to return to play. Approximately 50% of all ankle injuries occur during contact, with a high rate of recurrence. Effective preventative strategies with negligible performance deficits include taping, bracing, and proprioceptive training.16
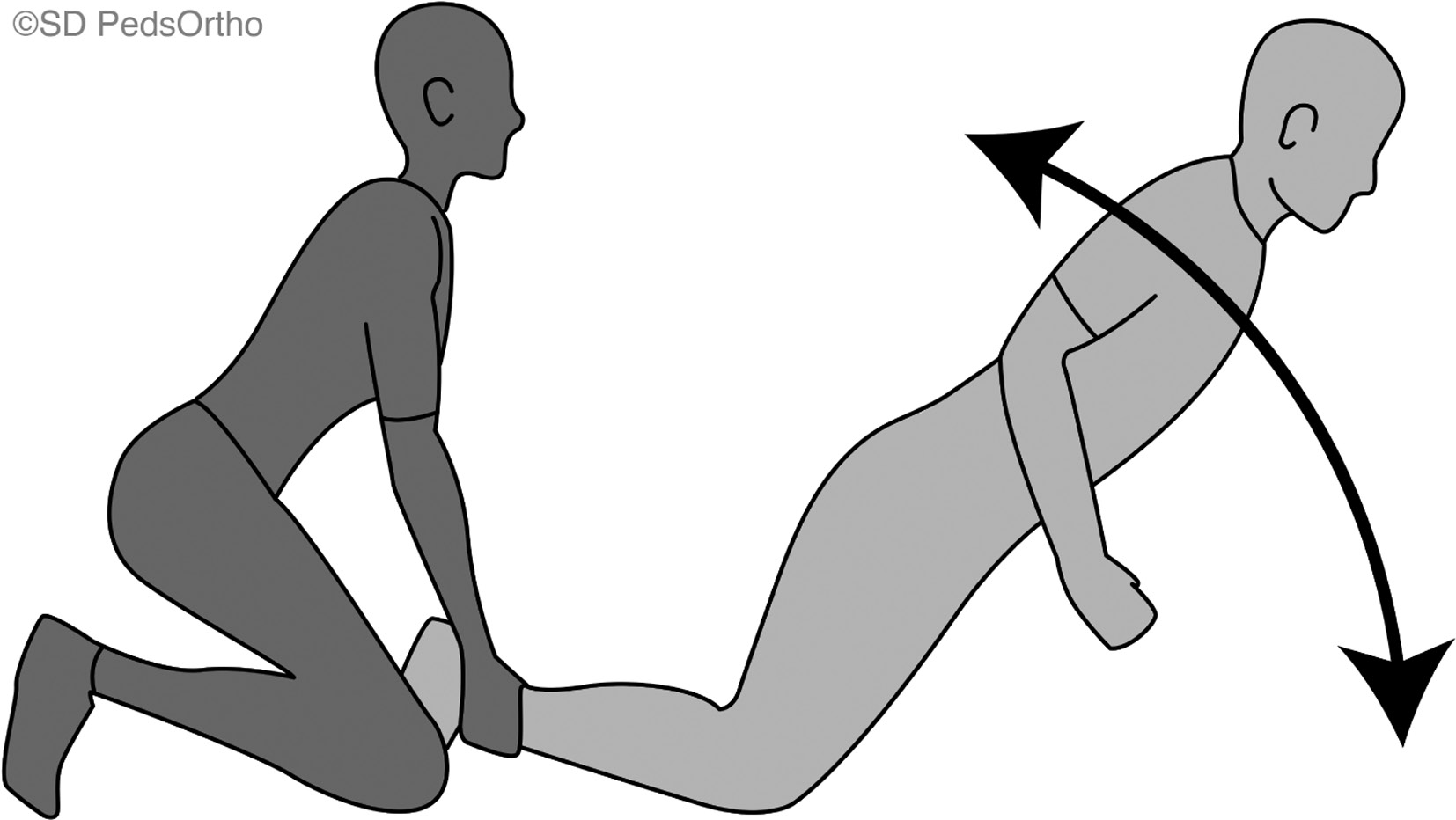
Rugby players sustain 5.6 hamstring musculotendinous injuries per 1000 player-match hours, the majority attributed to running activities.10 Backs are at higher risk than forwards for hamstring injuries, likely due to a greater frequency of maximum-effort sprints. Recurrent injuries are common, especially within the first month, and usually result in significantly extended recovery time. Thus, it is crucial to be judicious and gradually progressive with return to play protocols. Initial treatment normally consists of rest, NSAIDs, physical therapy, and an exercise program.10 Nordic hamstring exercises, consisting of warm-up stretching, flexibility training, and dynamic shifts between eccentric and concentric muscle strength training, have demonstrated reductions in the incidence and severity of hamstring injuries (Figure 7). Surgical intervention should be reserved for recurrent musculotendinous hamstring injuries that fail to respond to conservative management.
Figure 7. Nordic hamstring exercise.
Summary
Rugby union is the most popular contact sport in the world and the fastest growing sport in the United States. Even among contact sports, rugby union demonstrates a relatively high injury rate, with injuries ranging in severity from mild concussions to catastrophic spinal cord injuries. Compared with American football, overall injury rates in collegiate rugby are significantly higher with an increased distribution of concussions and upper extremity injuries seen in the rugby athlete. Injury rates also tend to be higher in men’s rugby when compared with women’s rugby and there is a unique distribution of injuries by sex. This review intends to provide the treating physician with the epidemiology of and mechanisms leading to common and serious injuries sustained by rugby athletes. Considerations for evaluation and treatment of injuries are provided as well as prevention strategies.
Additional Links
- World Rugby: https://www.world.rugby
- Rugby World Cup: https://www.rugbyworldcup.com
References
- Viviers PL, Viljoen JT, Derman W. A review of a decade of rugby union injury epidemiology: 2007-2017. Sports Health. 2018;10:223–227.
- World Rugby. Available at: https://www.world.rugby.
- Willigenburg NW, Borchers JR, Quincy R, et al. Comparison of injuries in American Collegiate football and club rugby: a prospective cohort study. Am J Sports Med. 2016;44:753-760.
- Peck KY, Johnston DA, Owens BD, et al. The incidence of injury among male and female intercollegiate rugby players. Sports Health. 2013;5:327-333.
- Williams S, Trewartha G, Kemp S, et al. A meta-analysis of injuries in senior men’s professional Rugby Union. Sports Med. 2013;43:1043-1055.
- Roberts SP, Trewartha G, England M, et al. Concussions and head injuries in english community rugby union match play. Am J Sports Med. 2017;45:480-487.
- Fuller CW, Laborde F, Leather RJ, et al. International Rugby Board Rugby World Cup 2007 injury surveillance study. Br J Sports Med. 2008;42:452-459.
- Gardner AJ, Iverson GL, Williams WH, et al. A systematic review and meta-analysis of concussion in rugby union. Sports Med. 2014;44:1717-1731.
- Fuller CW, Taylor A, Raftery M. Epidemiology of concussion in men’s elite Rugby-7s (Sevens World Series) and Rugby-15s (Rugby World Cup, Junior World Championship and Rugby Trophy, Pacific Nations Cup and English Premiership). Br J Sports Med. 2015;49:478-483.
- Brooks JH, Fuller CW, Kemp SP, et al. Incidence, risk, and prevention of hamstring muscle injuries in professional rugby union. Am J Sports Med. 2006;34:1297-1306.
- Fuller CW, Brooks JH, Kemp SP. Spinal injuries in professional rugby union: a prospective cohort study. Clin J Sport Med. 2007;17:10-16.
- Usman J, McIntosh AS. Upper limb injury in rugby union football: results of a cohort study. Br J Sports Med. 2013;47:374-379.
- Usman J, McIntosh AS, Quarrie K, et al. Shoulder injuries in elite rugby union football matches: Epidemiology and mechanisms. J Sci Med Sport. 2015;18:529-533.
- Singh VR, Trewartha G, Roberts SP, et al. Shoulder injuries in English Community Rugby Union. Int J Sports Med. 2016;37:659-664.
- Dallalana RJ, Brooks JH, Kemp SP, et al. The epidemiology of knee injuries in English professional rugby union. Am J Sports Med. 2007;35:818-830.
- Sankey RA, Brooks JH, Kemp SP, et al. The epidemiology of ankle injuries in professional rugby union players. Am J Sports Med. 2008;36:2415-2424.
- Sobue S, Kawasaki T, Hasegawa Y, et al. Tackler’s head position relative to the ball carrier is highly correlated with head and neck injuries in rugby. Br J Sports Med. 2018;52:353-358.
- Chéradame J, Piscione J, Carling C. Incidence and risk factors in concussion events: A 5-Season Study in the French Top 14 Rugby Union Championship. Am J Sports Med. 2021;49:1921-1928.
- Scorza KA, Cole W. Current concepts in concussion: initial evaluation and management. Am Fam Physician. 2019;99:426-434.
- Bates TJ, Lee P, Ellison TM, et al. Acute subdural hematoma in an elite-level rugby union player. Trauma Case Rep. 2020;26:100295.
- Hayashi D, Roemer FW, Kohler R, et al. Thoracic injuries in professional rugby players: mechanisms of injury and imaging characteristics. Br J Sports Med. 2014;48:1097-1101.
- Cooper S, Woodford NW, Maron BJ, et al. A Lethal blow to the chest as an underdiagnosed cause of sudden death in United Kingdom Sports (Football, Cricket, Rugby). Am J Cardiol. 2019;124:808-811.
- Thompson K, Kwon Y, Flatow E, et al. Everything pectoralis major: from repair to transfer. Phys Sportsmed. 2020;48:33-45.
- Kuster D, Gibson A, Abboud R, et al. Mechanisms of cervical spine injury in rugby union: a systematic review of the literature. Br J Sports Med. 2012;46:550-554.
- Ahearn BM, Starr HM, Seiler JG. Traumatic brachial plexopathy in Athletes: current concepts for diagnosis and management of stingers. J Am Acad Orthop Surg. 2019;27:677-684.
- Bowles DR, Canseco JA, Alexander TD, et al. The prevalence and management of stingers in College and Professional Collision Athletes. Curr Rev Musculoskelet Med. 2020;13:651-662.
- Tawfik S, Phan K, Mobbs RJ, et al. The incidence of pars interarticularis defects in athletes. Global Spine J. 2020;10:89-101.
- Reboursiere E, Bohu Y, Retière D, et al. Impact of the national prevention policy and scrum law changes on the incidence of rugby-related catastrophic cervical spine injuries in French Rugby Union. Br J Sports Med. 2018;52:674-677.
- Schroeder GD, Canseco JA, Patel PD, et al. Updated return-to-play recommendations for collision athletes after cervical spine injury: a modified delphi consensus study with the cervical spine research society. Neurosurgery. 2020;87:647-654.
- Brauge D, Delpierre C, Adam P, et al. Clinical and radiological cervical spine evaluation in retired professional rugby players. J Neurosurg Spine. 2015;23:551-557.
- Montgomery C, O’Briain DE, Hurley ET, et al. Video analysis of shoulder dislocations in rugby: insights into the dislocating mechanisms. Am J Sports Med. 2019;47:3469-3475.
- Bohu Y, Klouche S, Lefevre N, et al. The epidemiology of 1345 shoulder dislocations and subluxations in French Rugby Union players: a five-season prospective study from 2008 to 2013. Br J Sports Med. 2015;49:1535-1540.
- Lin KM, James EW, Spitzer E, et al. Pediatric and adolescent anterior shoulder instability: clinical management of first-time dislocators. Curr Opin Pediatr. 2018;30:49-56.
- Kwapisz A, Shanley E, Momaya AM, et al. Does functional bracing of the unstable shoulder improve return to play in scholastic athletes? Returning the unstable shoulder to play. Sports Health. 2021;13:45-48.
- Sabharwal S, Patel NK, Bull AM, et al. Surgical interventions for anterior shoulder instability in rugby players: A systematic review. World J Orthop. 2015;6:400-408.
- Rossi LA, Tanoira I, Gorodischer T, et al. Recurrence and revision rates with arthroscopic bankart repair compared with the Latarjet Procedure in Competitive Rugby Players With Glenohumeral Instability and a Glenoid Bone Loss <20. Am J Sports Med. 2021;49:866-872.
- Leroux TS, Saltzman BM, Meyer M, et al. The influence of evidence-based surgical indications and techniques on failure rates after arthroscopic shoulder stabilization in the contact or collision athlete with anterior shoulder instability. Am J Sports Med. 2017;45:1218-1225.
- Blonna D, Bellato E, Caranzano F, et al. Arthroscopic bankart repair versus open bristow-latarjet for shoulder instability: a matched-pair multicenter study focused on return to sport. Am J Sports Med. 2016;44:3198-3205.
- Usman J, McIntosh AS, Fréchède B. An investigation of shoulder forces in active shoulder tackles in rugby union football. J Sci Med Sport. 2011;14:547-552.
- Brooks JH, Fuller CW, Kemp SP, et al. Epidemiology of injuries in English professional rugby union: part 1 match injuries. Br J Sports Med. 2005;39:757-766.
- Awwad GEH, Coleman JH, Dunkley CJ, et al. An analysis of knee injuries in rugby league: the experience at the newcastle knights professional rugby league team. Sports Med Open. 2019;5:33.
- Montgomery C, Blackburn J, Withers D, et al. Mechanisms of ACL injury in professional rugby union: a systematic video analysis of 36 cases. Br J Sports Med. 2018;52:994-1001.
- Takazawa Y, Ikeda H, Saita Y, et al. Return to play of rugby players after anterior cruciate ligament reconstruction using hamstring autograft: return to sports and graft failure according to age. Arthroscopy. 2017;33:181-189.
